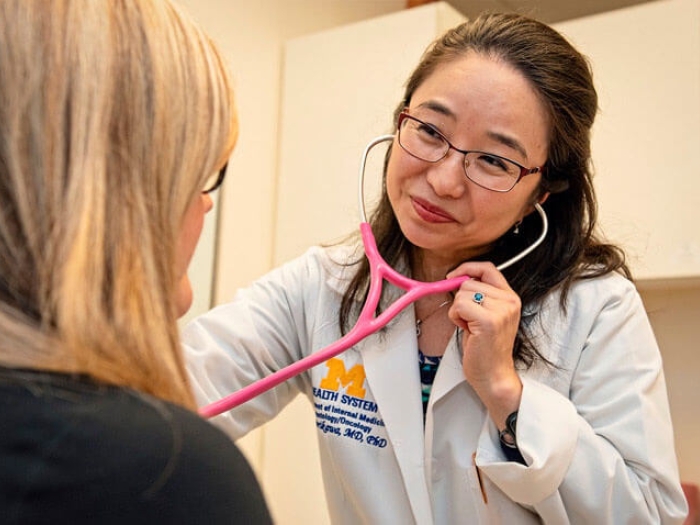
Hospitals and health systems nationwide, including Michigan Medicine, now tap advocates who bring compassionate and customized help to cancer patients.
7:00 AM
Author |

A cancer diagnosis comes with a lot of details to manage, whether you're getting care at a small community hospital or a large academic medical center. There will be medication and treatment times to keep track of, appointments to get to, diets to follow and instructions to remember.
MORE FROM MICHIGAN: Sign up for our weekly newsletter
Not to mention the need to balance family, pets, home and jobs.
All these moving pieces mean cancer patients need someone watching over them to help get it right.
Which is why, thanks to research on the complicated health care systems in the United States, more and more individuals will be partnered with an advocate — a patient navigator — to make it easier to get through treatment and focus on wellness.
"When patients are overwhelmed, it is difficult for them to be engaged in their care. You have much better care when patients are informed and involved in the decision-making process. This is what is happening with patient navigators," says Craig E. Cole, M.D., of the University of Michigan Comprehensive Cancer Center, who treats patients with multiple myeloma.
A trend toward personalized care
Patient navigator is a term used to describe anyone working in health care who helps patients better manage the details of their care.
In some cases, navigators are nurses. Other times, they are nonclinical staff assigned to patients to get to know their diagnosis and treatment plan, personal needs and goals, and to be a point person.
"With the increasing complexity of medical care and increasing age of our patients, people almost always require some type of navigation to get the full benefits of today's complex therapies," Cole says. "Treatment is not as straightforward as it was 10 years ago. The delivery of care is so much better with care coordinators to serve as trusted advocates for patients."
With the increasing complexity of medical care and increasing age of our patients, people almost always require some type of navigation to get the full benefits of today's complex therapies.Craig E. Cole, M.D.
Patient navigators at U-M
U-M's cancer center established a patient navigator program to assist patients in particularly challenging situations, which often come with certain cancer types such as multiple myeloma, sarcoma, head and neck cancer, and melanoma.
SEE ALSO: How Cancer Research Gave Hope to a Patient Previously Out of Options
"We meet with each patient within the disease group very early in their treatment process," says Jill Paladino, manager of the patient navigator program. "We'll do a brief check-in, assess the person's barriers to receiving care and troubleshoot with the patient."
These nonclinical navigators maintain regular communication with patients and families, coordinating care that is considerate of a patient's cultural beliefs and lifestyle. Navigators empower patients to manage their health.
Patients may experience different barriers to health care based on their personal situation, including but not limited to:
-
Having to come to treatment without a partner or caregiver
-
Living a far distance away and needing appointments to be on the same day
-
Difficulty remembering or staying organized because of treatment and side effects (i.e., "chemobrain")
-
High stress because of financial strain or family circumstances
-
Language barriers
-
Physical disability that makes getting around difficult
"We know every patient's needs are different," Paladino says.

Explore a variety of healthcare news & stories by visiting the Health Lab home page for more articles.

Department of Communication at Michigan Medicine
Want top health & research news weekly? Sign up for Health Lab’s newsletters today!