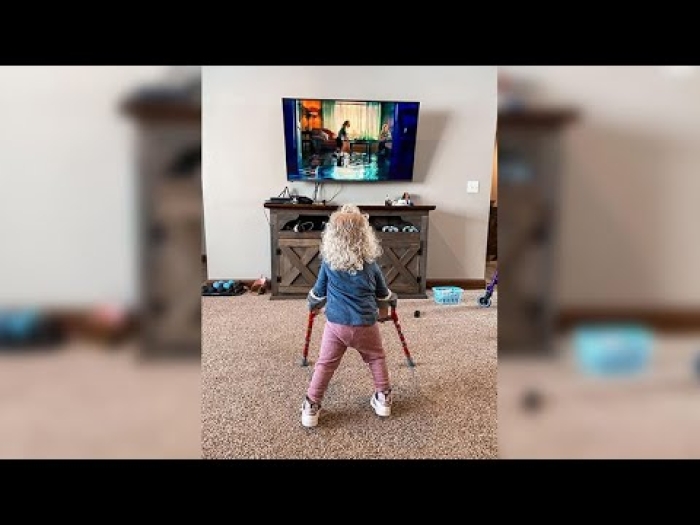
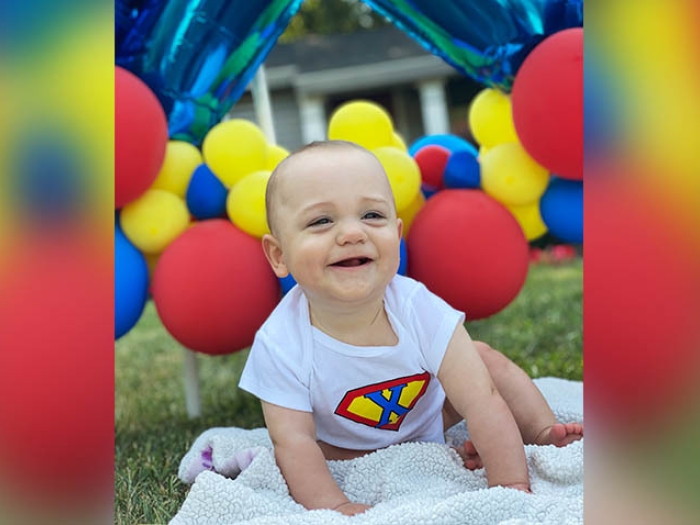
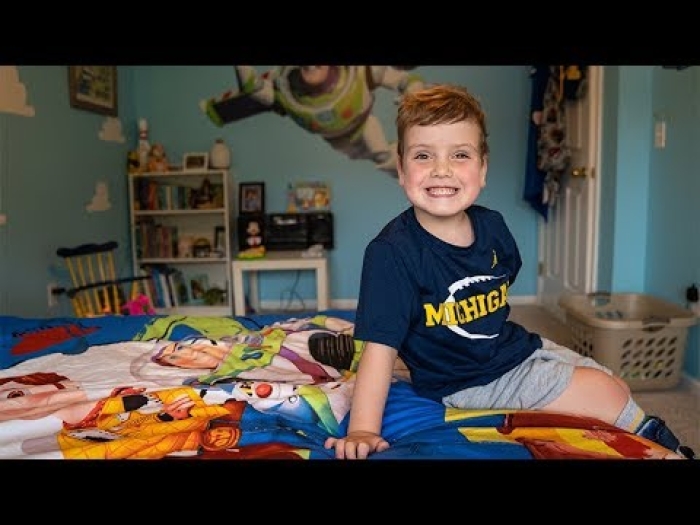
Nurses are the beating heart of any hospital. In the Newborn Intensive Care Unit, which houses the youngest and tiniest patients, the job becomes even more crucial.
1:00 PM
Author |
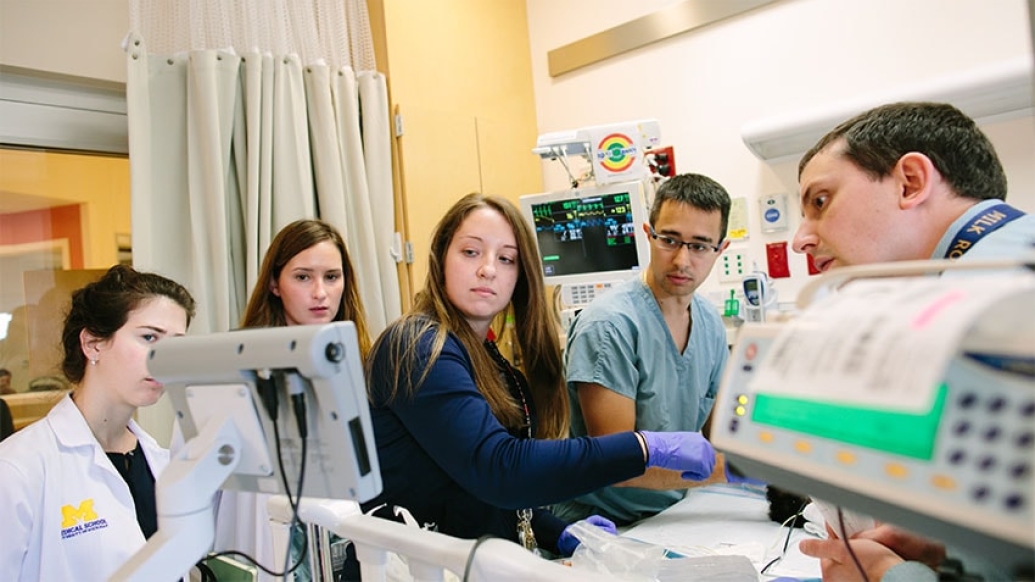

For the men and women who care for babies in the Newborn Intensive Care Unit, no day is ever the same. As a Level IV NICU, C.S. Mott Children's Hospital is certified as capable of providing the highest-level care for premature and critically ill infants.
MORE FROM MICHIGAN: Sign up for our weekly newsletter
A key part of this care? Nurses. Ask anybody in the hospital, and they'll tell you that the NICU nurses are extraordinary.
Take a look at a day in the life of the men and women who care so deeply for Mott's littlest Little Victors.
Every day starts out with a huddle.

Faith Sowers, R.N., leads the morning bed meeting — the "official" start of the NICU day. Physicians, nurses, respiratory therapists, unit hosts, lactation consultants and other specialists gather in a hallway in front of a large bulletin board to touch base on important matters of the day, including how full the unit is, any issues encountered the day before, expected arrivals and transfers, and discharges.
Rounding is a team sport.
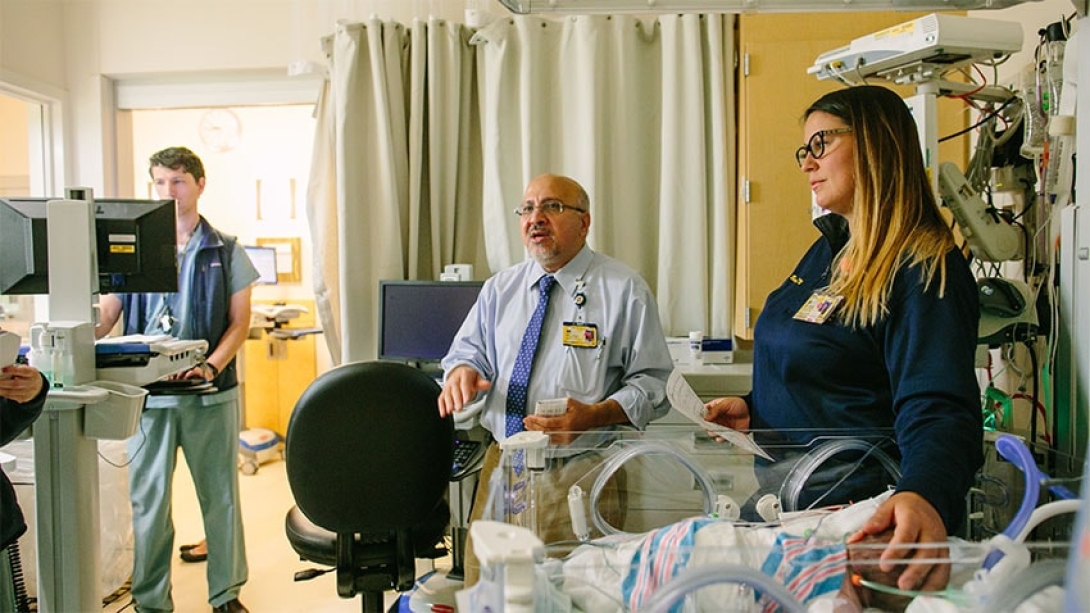
After the morning bed meeting, rounds begin. Above, Becky Butynski, R.N., reviews one of her patients with the patient rounding team, which includes physicians, respiratory therapists and nurses. The team travels from room to room to discuss each child's health, what has happened in the past day, and goals for the coming day and beyond. Depending on the patient's needs, rounds can also include a dietitian, pharmacist and care management nurse.
U-M practices family-centered rounds, meaning families are part of the team and are involved in the discussion and decision-making process.
It takes the best nurses to teach the best nurses.
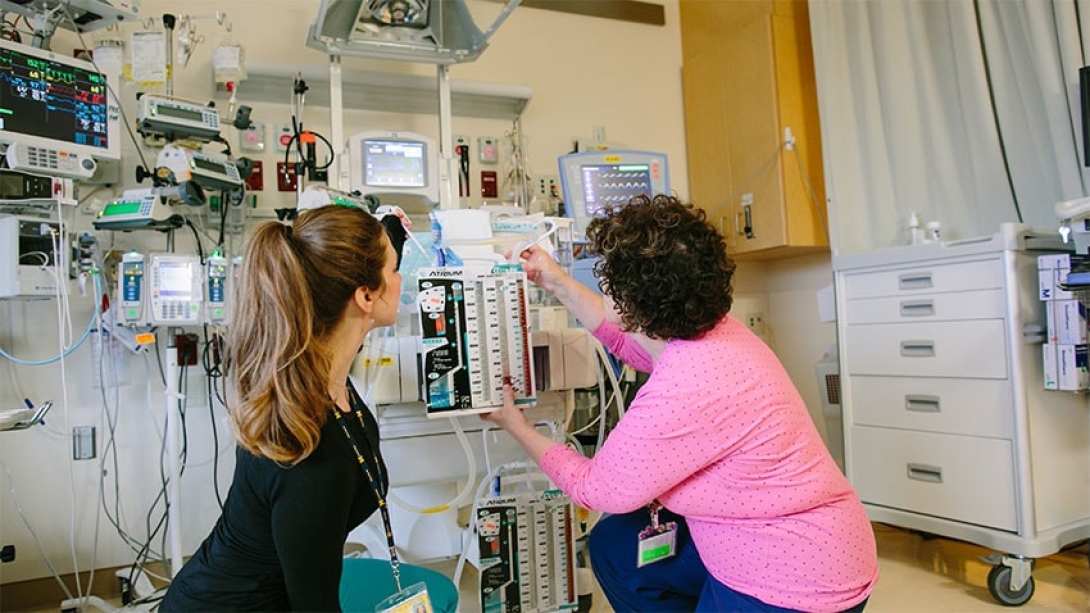
Great nurses don't happen — they're trained. Senior NICU nurses at Mott spend a decent chunk of their time training and orienting student nurses and new employees. Here, Deb Robinson, R.N., shows a new nurse how to check chest tube status.
Everything goes in the chart.

An accurate chart is critical to keeping everyone on the team informed of a baby's health status. Given the complex medical needs of NICU babies, nurses spend a sizable portion of the day documenting crucial information in each patient's digital chart so the team has access to all available information and can make informed medical decisions.
Make way, Little Victor coming through!

Kathy Sailus, R.N., and Stacey Tilbury, N.N.P., transport a baby to his room. Baby Evan was transported by Survival Flight from another hospital in Michigan. About 25 percent of the babies who pass through the NICU in a year are transfers from other hospitals.
Sailus and Tilbury are NICU nurses who have volunteered to go through additional training to be part of the Survival Flight team to assist when critically ill infants need to be transported to U-M from other facilities.
Batman has a bat phone. The NICU has a NEST phone.

Wendy Kenyon, R.N., right, hands off the NEST phone to nurse supervisor Lisa O'Leary, R.N. A senior nurse is in charge of the phone at all times, allowing for a direct line of contact between the Newborn Evaluation, Stabilization and Treatment (NEST) team in the birth center (one floor up) and the NICU. When a baby is being delivered with an anticipated need for the NICU, the nurse with the NEST phone can mobilize the appropriate staffing and resources to care for the hospital's newest charge.
Some things call for a costume change.

Once Kenyon had the NEST phone safely in the hands of another nurse, she headed down the hall to place a PICC line. A PICC line is a tiny catheter inserted into the baby's vein to allow for long-term delivery of IV antibiotics and blood draws. Kenyon is part of a specially trained team of nurses designated for inserting the equipment. Mott credits the team of nurses who've received extra training in placing PICC lines as part of the reason for the hospital's below-average bloodstream infection rate.
The birth center is our "crystal ball."

Charge nurse Sarah Poley, R.N., takes stock of the patient census and reviews needs for the next 24 hours. Today, Poley noted that the birth center was particularly full of expectant moms. Poley works with the labor and delivery teams to anticipate potential needs for acute care for premature babies and newborns with critical care needs.
Nurses are hands-on in procedures big and small.
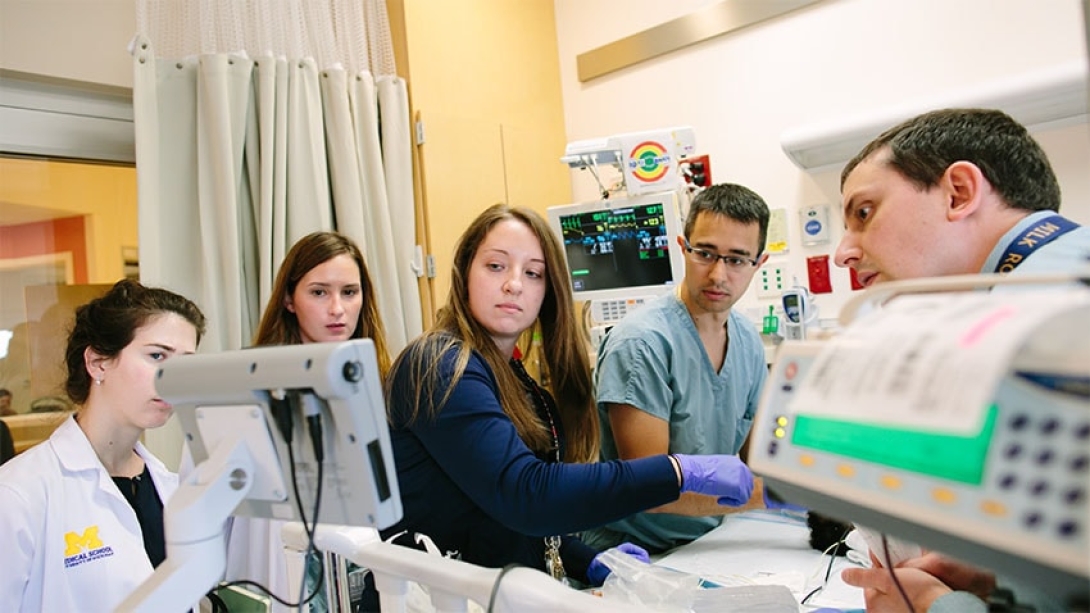
Katie Pounders, R.N., works with a team to do a controlled intubation procedure for an infant having trouble breathing. The team placed a flexible plastic tube into the baby's windpipe to help the infant breathe more effectively. Premature lung development and the need for supported breathing is one of the most common challenges NICU babies face.
Nurses help send patients from point A to B, and back to A.

Bonnie Shears, R.N., right, discusses a complex transport plan with O'Leary, the nurse supervisor. Shears, who has been a nurse in the NICU for more than 25 years, pieced together a complex plan to support the needs of her patient during his transport down to radiology for a fluoroscopy procedure.
They monitor monitors on monitors on monitors.

Julie Guminik, R.N., sorts through tubes and cords connecting an infant to a bank of monitors upon the baby's return from a trip down to radiology.
Safety first: In the NICU, everything is checked twice.

There is at least one "flex nurse" on the unit at all times to help fill in and support other nurses as they care for their patients. Here, flex nurse Lorri Gonzalez, R.N., works with Louise McInnes, R.N., to verify information in preparation for a blood transfusion. The process requires two nurses double-checking the numbers on the blood product against the patient's records to ensure it is the right blood type.
Here, we all become family.

For babies like Logan, who has spent more than 200 days in the NICU, nurses become a part of the family. As his parents prepare for his discharge, baby Logan's family brought in a quilt for his nurses to sign so he could one day read all the dreams his nurses had for him even when he was just a 1.1-pound baby.

Explore a variety of healthcare news & stories by visiting the Health Lab home page for more articles.

Department of Communication at Michigan Medicine
Want top health & research news weekly? Sign up for Health Lab’s newsletters today!