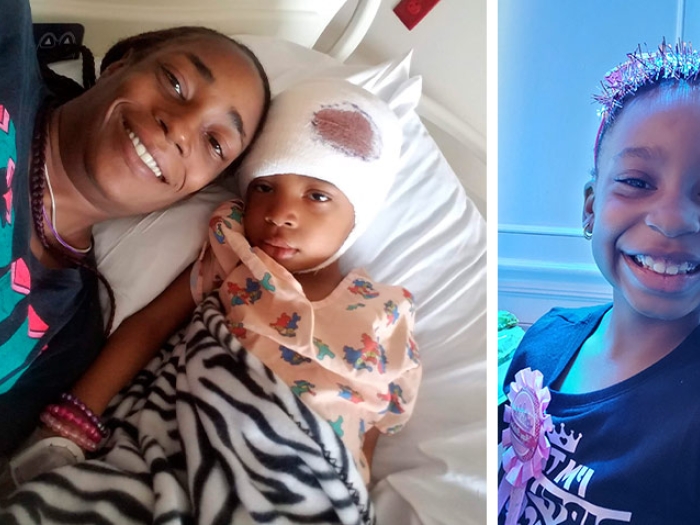
Severe pediatric epilepsy led one family to a hemispherectomy — a complex and specialized surgery. Within days of the procedure, their lives were transformed.
7:00 AM
Author |

Rehab Mohamed was only 18 months old when she suffered a severe stroke while recovering from heart surgery. It was while she was admitted to the hospital for the stroke that Rehab experienced her first seizure.
MORE FROM MICHIGAN: Sign up for our weekly newsletter
"It was the first time I had ever seen someone have a seizure, and it was terrifying," says Nabila Mohamed, Rehab's mom.
Doctors later determined that Rehab had developed epilepsy as a result of the stroke and put her on medication to manage the symptoms. Fortunately, the medication did its job.
For the most part, at least: "Rehab would still have seizures sometimes when she would develop a fever," says Nabila, "so we focused on controlling any fevers, keeping her cool and using medicine to keep her temperature down when she would get sick."
As Rehab grew older, though, the seizures came back. And they were no longer associated only with fevers.
By the time the child was 11, recurrences were frequent.
"She rarely made it through more than a few days of school at a time," Nabila says.
Nabila brought her daughter to the Comprehensive Pediatric Epilepsy Program at University of Michigan C.S. Mott Children's Hospital to seek help for Rehab, who by that point was experiencing four to five seizures a day.
A big decision
Doctors at Mott were prepared to offer comprehensive care.
SEE ALSO: Following 5-Year-Old Abbee Through Her 10th VEPTR Surgery
"We knew almost immediately that Rehab could be a good candidate for surgery," says Renée Shellhaas, M.D., M.S., the pediatric neurologist and epileptologist who evaluated Rehab, along with Hugh Garton, M.D., a pediatric neurosurgeon.
Rehab's initial consultation at U-M led to an expedited surgical evaluation that included neuromonitoring, SPECT scans to show blood flow in the brain, neuropsychometric testing, and speech and language evaluation. All signs were promising that surgery could be a good option for Rehab.
Still, the family's concerns lingered.
"We were very scared — it was not something we were willing to consider for a while," says Nabila. "You want your child to get better, but the possible side effects are hard to think about. For a long time, we weren't able to get past the fear."
After a year of thoughtful consideration, they decided they were ready to take the next step. So was the team at Mott.
"Dr. Shellhaas was wonderful," says Nabila. "She was very encouraging and patient with us."
Moving forward
Rehab underwent additional testing to help surgeons determine how to best perform the procedure.
They were able to pinpoint the part of the brain where the seizures were primarily coming from — and, importantly, that the right hemisphere of her brain was healthy and not involved in the seizures.
A collaborative medical review then followed.
"We presented Rehab's case at our Refractory Epilepsy Conference," notes Garton, referring to a multidisciplinary group of pediatric epilepsy specialists, including neurology, neurosurgery, neuropsychiatry, speech pathology, radiology and social work, that meets weekly to discuss complex epilepsy surgery cases to ensure that each patient benefits from multiple perspectives and areas of expertise.
Ultimately, it was determined that a hemispherectomy would be Rehab's best option.
During the procedure, which lasted about six hours, Garton disconnected the left hemisphere of Rehab's brain to prevent the spread of electrical current from the left hemisphere to the right so that the abnormal activity from her injured hemisphere wouldn't cause clinical seizures.
The complex procedure is only performed in specialized epilepsy centers such as U-M.
"Anytime we're operating in the brain, precision and accuracy are the incredibly important considerations," notes Garton, who utilized unique intraoperative MRI technology to get ultra-detailed images of the brain during the surgery from right in the operating room. "The ability to get that type of imaging in the OR helps us confirm that we've dealt with all the tissue that must be disconnected to stop the seizures, and helps us avoid the need for additional surgery."
Rehab remained in the hospital for a month after surgery, two weeks of which was focused on intensive inpatient rehabilitation to prepare her for life outside the hospital.
"At first, Rehab wanted to go home; she was ready to be done with the hospital," notes Nabila. "But she actually ended up really enjoying her rehabilitation. We all loved it."

Life after surgery
Aside from two very mild seizures during her initial recovery, Rehab has been seizure-free since the surgery for almost two years.
SEE ALSO: Getting the Diagnosis of a Brain Tumor at Age 18
In addition to the seizures, Rehab also struggled with being able to remember things before her surgery.
"Her memory was so poor, but now she remembers everything. She always likes to be on time, asks lots of questions and wants to learn everything."
Rehab now attends school regularly, and in her free time she enjoys reading the Qur'an with her six siblings and helping out in the kitchen.
Nabila wants other families of kids with severe epilepsy to have hope, and know that things can get better — even when the idea of taking action seems scary.
"It was a hard decision for us to undergo surgery; we really struggled with it," she notes. "But it was the right decision, and I only wish we'd done it sooner."

Explore a variety of healthcare news & stories by visiting the Health Lab home page for more articles.

Department of Communication at Michigan Medicine
Want top health & research news weekly? Sign up for Health Lab’s newsletters today!