If you have leg pain triggered by physical activity, it’s possible that you have poor circulation, which is closely linked to peripheral artery disease, or PAD.
1:00 PM
Author |
Leg pain is something we all experience at one time or another.
But when might a pesky cramp or ache be the sign of something more serious?
MORE FROM MICHIGAN: Sign up for our weekly newsletter
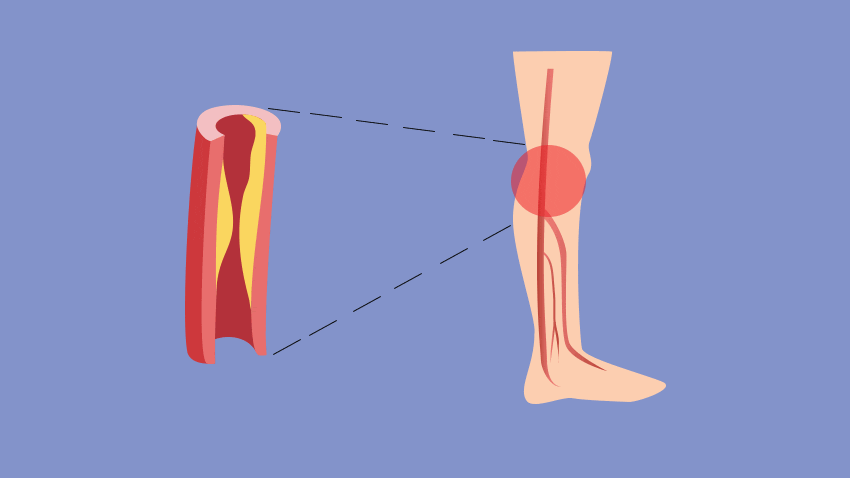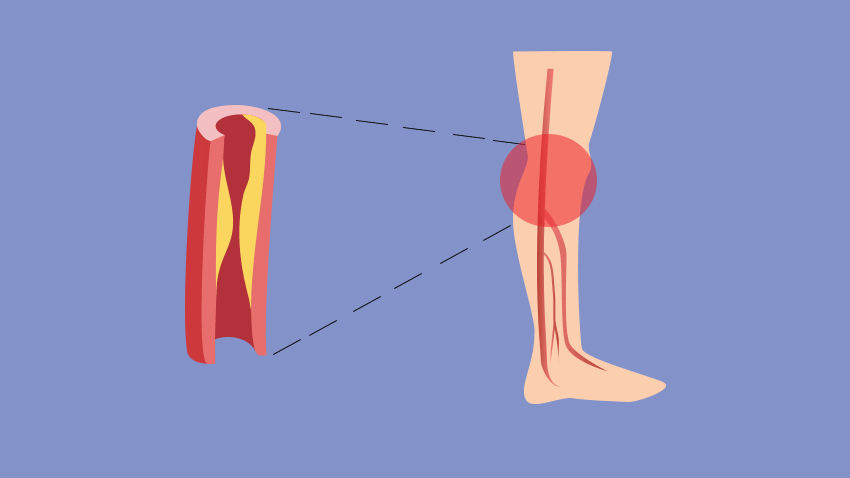
If you've been told your leg pain is a result of poor circulation — a reduction in the blood, oxygen and nutrients moving through your body — it's likely that you have peripheral artery disease, or PAD, says Peter Henke, M.D., a vascular surgeon at the University of Michigan Frankel Cardiovascular Center.
Nearly 12 million people in the United States have PAD, but many don't realize it because symptoms are often mild.
PAD occurs when plaque builds up in the arteries and prevents blood from getting to the muscle and tissue. Although this plaque buildup can occur in arteries throughout the body, it is most commonly found in the lower extremities, typically in the muscle and tissue of the calf.
They aren't the only spots: "PAD can also occur in the thigh, hip and buttocks," says Henke, noting these locations are less common.
No matter the affected area, the discomfort shouldn't be ignored.
Says Henke, "If you're diagnosed with PAD, it's a sign that your blood vessels are not healthy, which means you're more likely to develop other serious cardiovascular issues such as coronary heart disease or heart attack."
He addressed some common questions about PAD.
What are the signs and symptoms?
One of the most telling symptoms of PAD is pain that comes on with activity and subsides when the activity is stopped.
Other indications include:
-
Pain in the legs or feet that wakes you up at night and subsides when your legs are dangled over the bedside
-
Numbness or loss of sensation in the affected limb
-
Sores that heal slowly or fail to heal
-
Differences between limbs in their color or warmth
-
Decreased rate of hair and nail growth on the affected limb
-
Foot pain at rest
How is PAD diagnosed?
"PAD is diagnosed using the ankle-brachial index," says Henke. This simple and safe test measures the blood pressure at the ankle and upper arm.
SEE ALSO: Peripheral Artery Disease Treatment Gives Barber a New Look
A normal resting ankle-brachial index is 1.0 to 1.3, which means that your blood pressure at your ankle is the same or greater than the pressure at your arm and suggests that you do not have significant narrowing or blockage of blood flow.
If your blood pressure in your ankle is lower than 0.9, you may have PAD.
Who is at risk for PAD?
The same people with a high risk of heart attack and stroke are also at risk for PAD.
Among them: those 50 and older, smokers, people with high blood pressure and high cholesterol, and overweight or obese individuals, says Henke.
Other contributing risk factors may include:
-
Diabetes
-
Family history of vascular disease such as PAD, aneurysm, heart attack or stroke
-
High levels of homocysteine, an amino acid in your blood
-
Inactive lifestyle
Can you stop or prevent PAD?
There are some surefire things you can do, says Henke. Most involve lifestyle changes.
-
Stop smoking
-
Control your blood pressure and cholesterol
-
Eat a healthy diet
-
Get regular exercise, particularly walking
Henke recommends asking your health care provider about taking a daily aspirin to prevent clots or other appropriate drugs to reduce your blood pressure and cholesterol.


Explore a variety of healthcare news & stories by visiting the Health Lab home page for more articles.

Department of Communication at Michigan Medicine
Want top health & research news weekly? Sign up for Health Lab’s newsletters today!





