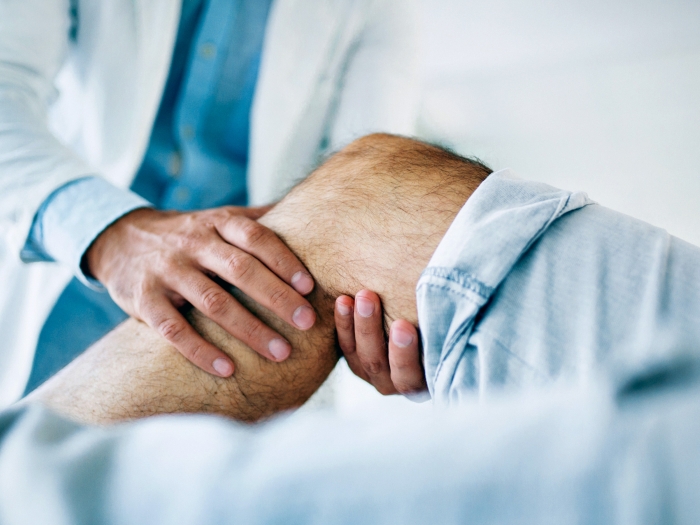
He couldn’t feel the wounds open on his sides. Without surgery he would be permanently bed-ridden.
2:23 PM
Author |

Adjusting to life in a wheelchair never came easy to Doug Calka. An adrenaline junkie who spent years racing dirt bikes, the Michigan native finds ways to keep moving.
"I still try to do most things myself," he said. "I cut the lawn on my own with my zero-turn mower. I just make modifications to everything I do."
The 54-year-old weekend warrior lost control on an 80-foot jump he'd "made 100 times before" during a race nearly 10 years ago.
"I knew I was going too fast and got too high," Calka said. "While I was in the air, I pushed my bike away and landed square on my feet. I heard my back crack, and I was done."
Instantly, Calka knew what he had lost. Only later did he realize it was much more than the feeling in his legs.
"It's a chance every rider takes, signing a waiver when you come in," he said. "There isn't much worse of an outcome than being paralyzed from a crash because this didn't just affect me. It affected my wife and daughter. A mistake I made changed their life more than I ever thought."
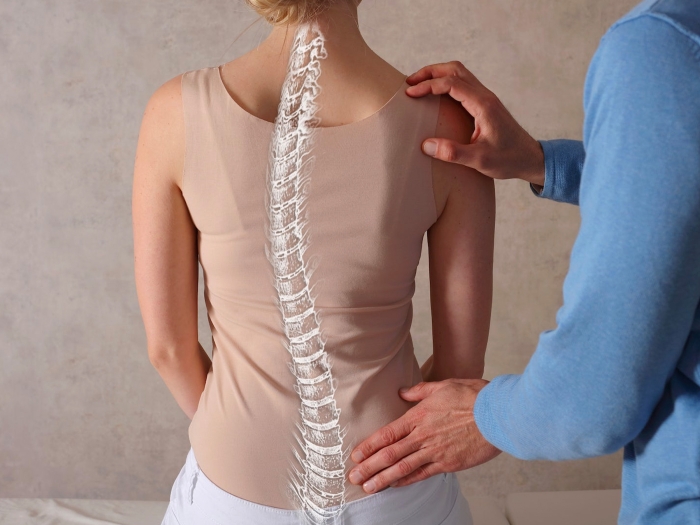
The T12 spinal fracture paralyzed Calka from the waist-down. His family home in Romeo required a complete remodel. Everyday activities like working and sleeping became a hassle. His wife, Sue, effectively became his caregiver.
"When you really love somebody, you do whatever it takes, for better or worse," said Sue, who married Calka in 1993. "We're still learning how to handle it, but we don't use it as an excuse. You keep moving on and keep living. I'm so grateful he is still with me."
Pandemic downturn
Years into the adjustment, and just before hospitals limited services at the onset of the pandemic, Calka noticed his dog licking his hip. Calka couldn't feel that a pressure sore had developed on his right side.
"Thank God for dogs," he joked. "But then the wound got bigger and bigger, to the point where I had to stop working because I was bleeding through my bandage and my clothes, on the car seat going home. Finally, I just couldn't keep working."
Unable to receive proper care for the open wound, Calka developed osteomyelitis, an infection that can occur when a bone becomes exposed. Patients with spinal cord injuries are more prone to such infections without pain as a protective mechanism, said Jaimo Ahn, M.D., Ph.D., an orthopaedic surgeon at Michigan Medicine.
"We normally think of pain as something undesirable, something we want to get rid of," Ahn said. "But the irony, of course, is that once it's gone to the extent that we don't know something is wrong, then we can't protect ourselves."
Calka was treated with several antibiotics before receiving care at Michigan Medicine. The bacteria affecting his bones, however, began developing resistance to the drugs, said Shiwei Zhou, M.D., a physician in the Division of Infectious Diseases at Michigan Medicine.
SEE ALSO: "They Put Him Back Together Again"
"He would feel better on the antibiotics, but without fixing the problem, we can only drive more resistance," Zhou said. "It was just a matter of time before we ran out of antibiotics."
Zhou has a name for this: the overflowing sink. The source of the problem is the open wound, which leads to spill-over issues, like infection. Using antibiotics, she can contain the infection, but someone needs to "turn off the spigot" before the bacteria become resistant.
"I have a couple other patients who were not as lucky as Doug," she said. "They were too far along in their infection that surgery isn't an option for them, and I am managing them with antibiotics almost as a palliative measure. At some point, I can't fix the issue. It's incredibly frustrating and scary."
The care team cycled through options, and Calka continued to decline. His daily conversations were cut short by labored breathing, and he made constant trips to the hospital for more blood transfusions. It all felt like treading water
We had to do this [surgery] because if we hadn't, the infection could spread more deeply into his pelvis and beyond. Removing that would have left Mr. Calka bed-bound permanently.Jaimo Ahn, M.D., Ph.D.
"The hole in my hip was so large, one doctor could put his whole hand in there," he said. "I got an appointment at the ER because there was no doubt I was dying. I was at the bottom of the rope barely hanging on by a worn-out hand."
One last shot
At the advice of a friend, Calka called U-M's Section of Plastic Surgery for a consultation, and he was later admitted to the hospital.
"When I met Dr. Ahn, I told him point blank, 'I'm done,'" Calka said. "He was calm, understood my issue and asked me my goal. I told him I just wanted to be comfortable and live a decent life with my family."
Working with Zhou and Jeffrey Kozlow, M.D., Ahn decided to perform a hip disarticulation. More simply, he would separate Calka's body at the hip.
SEE MORE: Organ Donation Saves Three Lives in One Family
"This wasn't a 100% curative decision," Ahn said. "We had to do this because if we hadn't, the infection could spread more deeply into his pelvis and beyond. Removing that would have left Mr. Calka bed-bound permanently."
The veteran surgeon removed Calka's femur bone, cutting away as much of the infection as he could find. Then Kozlow, a plastic and reconstructive surgeon, used the remaining healthy tissue to create a flap that would cover the area and prevent further infection.

The aftermath
Calka noticed improvements almost immediately after surgery. He stopped throwing up, could hold a conversation and his hands no longer shook uncontrollably.
"When you don't have feeling below your waist, maybe you don't recognize immediately that you've had a leg completely removed," he said. "But it's all those other things that told me everything was going to be OK. And I'm like, 'Wow, I'm feeling so much better.'"
Hip disarticulation is not a novel procedure, but it is rare for hospitals to coordinate the many disciplines required to execute it. Ahn credits Zhou for bringing together all the specialists needed to create this type of life-altering plan for patients with bone infections like Calka.
"It is very helpful to get together once a month and discuss their care as a group so we can use all of our brains to come up with collective decisions, rather than working solely as individual doctors and providers," he said. "In this situation, it allowed us to accomplish our goal, which was to give Mr. Calka a new lease on life for him and his family."
The recovery process is slow. Calka started physical therapy, and he gradually made his way back to work. No sweat, he noted, seeing as he was "laying on [his] death bed" for an entire year before the surgery. Instead, when he looks down or others comment on his leg, Calka is motivated.
"This was a life-changer, and no one helped me like Dr. Ahn and this team," he said. "I'm working my way back. You learn from these things; you become a better person and pull yourself up. Every day is a gift."

Explore a variety of healthcare news & stories by visiting the Health Lab home page for more articles.

Department of Communication at Michigan Medicine
Want top health & research news weekly? Sign up for Health Lab’s newsletters today!