Science teacher Keith Piccard’s life used to revolve around seizures. Now, a decade after surgery, he focuses on his career and family instead.
7:00 AM
Author |
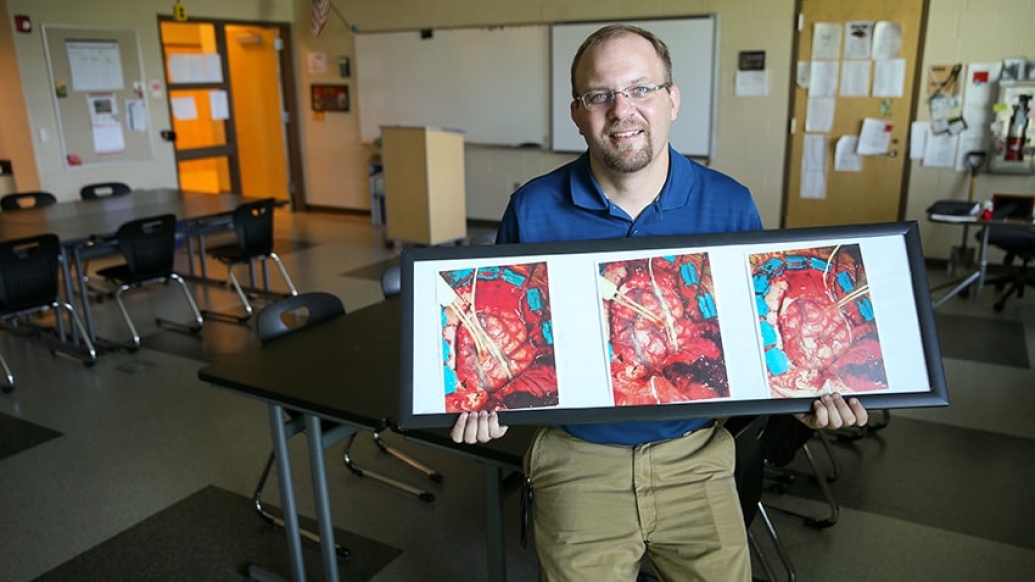
It's 2006. Keith Piccard wakes up every day, not knowing whether, or when, he'll have a seizure. He experiences auras, or the hallmark sensory signs of seizure, a few times a day, and a grand mal seizure a couple of times each month. Piccard diligently keeps a seizure diary and relies on his new wife and his co-workers to step in and call for help when a seizure begins.
SEE ALSO: Alzheimer's: Not Just a Disease for Older Adults
In 2016, Piccard wakes up, has breakfast with his wife and two young daughters and prepares to teach his Allendale Middle School science students, followed by his evening as a Grand Valley State University biology professor or a middle school wrestling coach. That depends on the day for this award-winning educator.
The difference?
Successful awake brain surgery for temporal lobe epilepsy.
"It was a huge blessing," Piccard says.
"Keith is eloquent and accomplished," adds his neurosurgeon, Oren Sagher, M.D. "Celebrating 10 years of high performance after surgery is a great milestone for him."
'Like warm honey'
Piccard had a febrile seizure, which is a high fever with a seizure, as an infant. It doesn't happen often, but some children will continue to have seizures after the first one. By 4 years old, he grew out of them, but the seizures returned again in his late teens.
He hasn't experienced an aura in more than nine years, but Piccard still remembers them vividly.
It would start with a rush down his brain, "like warm honey," that worked its way down to the rest of his body. When he noticed a metallic taste in his mouth, he knew it was going to be a little worse. Then a sound like a moth fluttering in his ear meant it was time to alert someone or call 911.
Once his eyes started flashing, his body would flex, and he couldn't do anything about it.
"They're scary in that I could feel my body flexing and shaking, but it's uncontrollable," Piccard says. "To be cognitively aware that you can't control your body is very weird."
His neurologist, Simon Glynn, M.D., says it's important to consider surgery for epilepsy patients like Piccard who are not responding to their medications, all in a timely manner.
"Losing 10 or 15 or 20 years of your life to a disabling condition is upsetting," he says. "The time these young people are losing is the time they're getting an education, establishing a career and starting a family."

'We want to unburden patients with epilepsy'
"I was on high doses of a lot of medication, and the seizures progressively became worse and worse," Piccard says of the time before his surgery.
SEE ALSO: Former Boxer Gives Brain Tumor a Counterpunch
Eventually, he was referred to the University of Michigan Comprehensive Epilepsy Program where the team determined he was a good candidate for surgery.
"When you don't know when your next seizure is going to be, you can't drive or use machinery, and even cooking can be risky," Sagher says. "It's incredibly infantilizing, and we want to unburden patients with epilepsy."
Sagher removed the portion of Piccard's temporal lobe that was causing the seizures.
"We had a plan in place that allowed us to maximize the chances that Keith would end up seizure-free, and minimize the chances he would have a disability later," Sagher says.
Anesthesiologists kept Piccard comfortable, but awake, because the team operated on his language dominant side. Speech and language pathologist Karen Kluin tested him before, during and after surgery to be sure his language ability was still intact.
"They took something out of my head and made me smarter," Piccard says. His cognitive scores actually increased once the damaged part of his temporal lobe was removed.
"I'm in contact with 1,000 students every year, and it simply wouldn't be possible if I was still struggling with seizures," he adds.
He may not have to think about epilepsy every day anymore, but Piccard keeps a photo of his brain taken during surgery in his classroom, hoping to inspire his students to study science and create the next medical advance.
For Glynn's part, he says Piccard represents the aim of neurologists working with epilepsy patients.
"It's rare for neurologists that you get to undo a condition someone has, and that's the goal of our epilepsy center," Glynn says. "Keith is an excellent example, because he is living a normal life and now only comes to see me once a year, and then only to review any questions he might have and be sure there are no difficulties with his medicine. I could not be happier for him."

Explore a variety of healthcare news & stories by visiting the Health Lab home page for more articles.

Department of Communication at Michigan Medicine
Want top health & research news weekly? Sign up for Health Lab’s newsletters today!