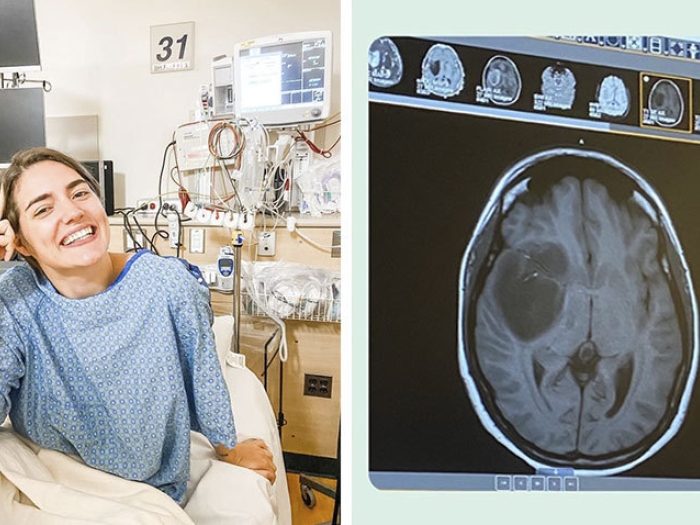
With the deadly brain tumor in the news, an expert outlines the basics of the disease and its treatment options.
3:20 PM
Author |
An aggressive brain tumor, a glioblastoma is considered a rare cancer with a poor prognosis.
SEE ALSO: The Story of Dad's Brain Tumor, Told Through an 11-Year-Old's Eyes
As the cancer receives a swell of attention on the heels of Arizona Sen. John McCain's diagnosis, Michigan Medicine neurosurgeon Daniel Orringer, M.D., who regularly treats glioblastoma patients, explains the condition and the present state of glioblastoma care.
Why is glioblastoma such a devastating diagnosis?
Orringer: Glioblastoma is one of the most dreaded diagnoses that we can give a patient because the treatments that we have are typically not curative and the disease marches at a very fast pace. Even with the best available treatments, patients don't live very long after diagnosis. Median survival of patients with glioblastoma is on the order of 14 to 16 months. However, some patients live a bit longer, and we're starting to understand the genetic basis of why some patients respond better to radiation and chemotherapy than others.
Our goal is to prolong the patient's quality time when they're faced with a very serious diagnosis.
What makes glioblastoma difficult to treat?
Orringer: Glioblastoma has a very infiltrative pattern of growth, almost spreading out like a cloud of cells in the brain. There isn't a very discrete margin as there is with some tumors, such as meningioma. It's very difficult for the surgeon to differentiate where the tumor ends and the normal brain begins because there's a gradient of cells going out into the normal brain.
Why isn't surgery curative for glioblastoma, and how does that affect treatment?
Orringer: Historically, the feeling has been that even in situations where a tumor is isolated to one part of the brain, we can find cells from the tumor in a very distant part of the brain. The thinking is glioblastoma cells can spread out in the brain over the course of several centimeters. It's not possible to remove all of the brain tissue containing those abnormal cells.
Because surgery is almost never curative for a diagnosis like glioblastoma, we follow that surgery up with radiation and chemotherapy that address a larger volume of the brain that's affected by the disease.
It's important that the patient is empowered with the knowledge that there are experimental treatments out there, too. One of the most important things that will help us make headway in glioblastoma is enrolling patients in clinical trials. It's through those clinical trials that we'll make advances in the treatment of what's a very difficult disorder to treat.
For the vast majority of patients who end up with glioblastoma, there's no clear underlying cause. Some patients are just more predisposed based on their genetic makeup.Daniel Orringer, M.D.
What causes glioblastoma?
Orringer: We commonly are asked the question, "How did I get this?" or "What did I do wrong?" There haven't been, with the exception of exposure to ionizing radiation, any clear risk factors identified. There are some genetic syndromes that are associated with the formation of glioblastoma, but those are very rare cases. For the vast majority of patients who end up with glioblastoma, there's no clear underlying cause. Some patients are just more predisposed based on their genetic makeup.
SEE ALSO: Surviving Brain Cancer Inspires Incoming Freshman to Pursue Medicine
We also know from recent evidence that most tumors in the human body occur sort of at random, and it's a matter of chance.
What are the symptoms?
Orringer: The common presenting symptoms can be headache, seizure, difficulty with language, difficulty with movement and coordination, and sometimes cognitive changes can occur. When a patient has a certain set of red flags, that is a signal to their physician that something out of the ordinary may be occurring. For example, if a patient goes through 70 years of life and very infrequently has headaches and then suddenly starts getting headaches on a regular basis, especially in the morning, that's a red flag that the patient should have further imaging. A patient can work with their physician to determine whether further imaging is required, which is a key part of determining whether a tumor is present.
What's the state of glioblastoma research?
Orringer: There's a lot that we still don't know about glioblastoma. We've studied it extensively for a long time but we're still learning about the process of development of a glioblastoma, and that makes it difficult for us to develop effective treatments.
We're also learning about the way the immune system attacks a glioblastoma, or doesn't and allows a tumor to form. One of the exciting areas of research in the brain tumor field is immunotherapy, in which the immune response is trained against the tumor. Much in the way that vaccination would work, we're trying to elicit an immune response against certain proteins that are expressed by the tumor. There are a number of exciting clinical trials that have shown some early promise with respect to immunotherapy and that, I would say, is one of the frontiers in glioblastoma research and one of the areas of hope for patients with glioblastoma and those who are treating them.

Explore a variety of healthcare news & stories by visiting the Health Lab home page for more articles.

Department of Communication at Michigan Medicine
Want top health & research news weekly? Sign up for Health Lab’s newsletters today!