While 22 weeks pregnant, Fiona Linn learned her unborn daughter had a heart defect, requiring surgery. Here, she tells her family’s story.
7:00 AM
Author |
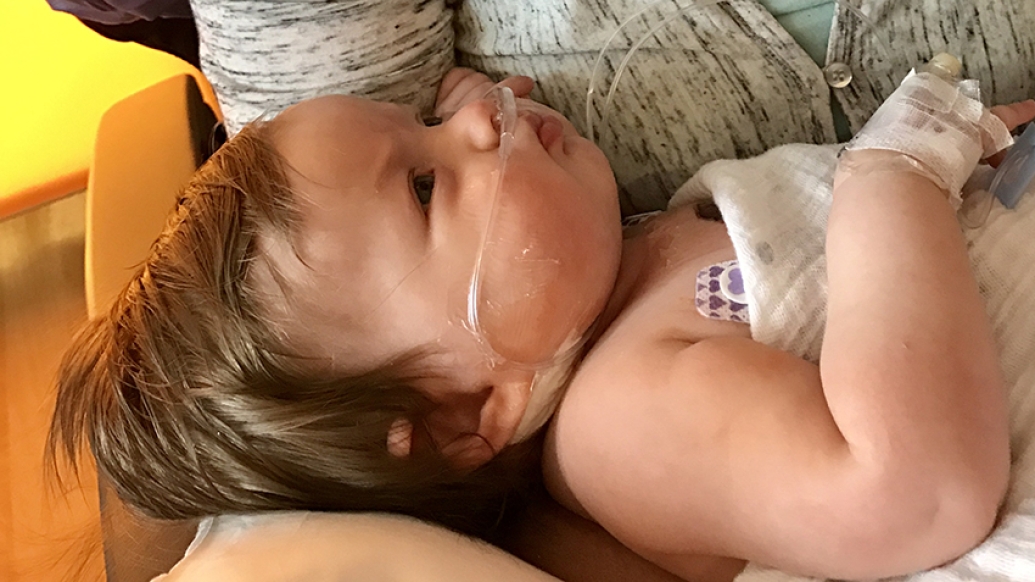
When Fiona Linn came to Michigan Medicine for a prenatal ultrasound last year, she expected everything to be routine. The news she received that day, however, was anything but.
"The technician noted an abnormality and immediately sent us for a heart scan," Linn says.
MORE FROM MICHIGAN: Sign up for our weekly newsletter
The test identified a common congenital heart defect in Linn's daughter, Nina, called tetralogy of Fallot. The condition features four problems, with the most severe being a hole in the heart and an obstruction of the opening between the heart and lungs. There is also an overly thickened muscle over the lower right chamber, and the aorta lies over the hole in the lower chambers.
"If left untreated, tetralogy could eventually be fatal to a young child," says Richard Ohye, M.D., Nina's surgeon in the Congenital Heart Center, part of the University of Michigan C.S. Mott Children's Hospital. That's why the most critical issues are repaired surgically early in a patient's life.
"Just 22 weeks into my pregnancy, we knew my daughter would need open-heart surgery by the time she was 4 months old," Linn says. "That's pretty jarring."
Medical advancements have led to lofty survival rates among children with congenital heart defects — upward of 97 percent. But, according to Ohye, "any open-heart surgery for a child is a traumatic event and can lead to complications. Nothing can be taken for granted in those situations."
Any open-heart surgery for a child is a traumatic event and can lead to complications. Nothing can be taken for granted in those situations.Richard Ohye, M.D.
'Nina was in good hands'
Linn is intimately familiar with Michigan Medicine, working for the past five years as a project manager in University Hospital and Frankel Cardiovascular Center operations.
"Because I work at the hospital, I know firsthand how wonderful our teams are, including those in the Congenital Heart Center," Linn says. "And while it took a little longer for my husband to get comfortable, we could certainly see that Nina was in good hands from the moment she was diagnosed."
The couple met with physicians, nurses and technicians throughout Linn's pregnancy, ensuring no further issues were found.
Linn gave birth Aug. 18, and the cardiac team was on hand immediately after delivery to better understand the severity of Nina's defect and determine the best treatment plan.
"Once she was born, cardiologists had the opportunity to see things a bit more clearly," Linn says.

Small actions, big impact
Nina's surgery occurred successfully on Dec. 20, which meant the family would be spending the holidays in the hospital.
SEE ALSO: Twin Sisters Survive Lethal Bond, Then Laser Surgery, in the Womb
"For the first two nights after her procedure, she was in the cardiothoracic ICU," Linn says. "The nurses and practitioners made sure she was comfortable at all times and, even though I wasn't able to hold her, they allowed me to get as close to Nina as possible to comfort her — and have her comfort me. They never took away our chance to bond."
By the third day after surgery, Nina's health was improving and she was moved to a room in the inpatient portion of the Congenital Heart Center.
The family spent the rest of their stay in the unit, but team members ensured that everyone was taken care of, even Nina's big sister, Zoe, who is 3½. Child life specialists made sure she had games to play and books to read while visiting her little sister.
"It was the holidays, and staff members brought around donated toys for us to give to our children as gifts," Linn says. "It was a really nice touch that gave our family — and the families around us — a chance to take our minds off our baby's health for a few minutes."
Nina was released one week after her surgery and has received positive health reports since. While her procedure is considered "one and done," Linn says her daughter — like most children born with a congenital heart defect — will undergo an annual checkup.
"We will keep an eye on her throughout her lifetime," Ohye says. "We'll make sure no complications pop up, so she can have the same quality of life as anyone else."

Explore a variety of healthcare news & stories by visiting the Health Lab home page for more articles.

Department of Communication at Michigan Medicine
Want top health & research news weekly? Sign up for Health Lab’s newsletters today!