Once on the heart transplant waiting list, the Michigan toddler’s heart now beats on its own.
5:00 AM
Author |

A normal pregnancy ended in a terrifying birth for Elizabeth and her husband, Brandon: as soon as new baby Sullivan's umbilical cord was cut, he started to turn blue.
Within an hour or two, Sullivan was airlifted from Beaumont Hospital, Royal Oak, to University of Michigan Health C.S. Mott Children's Hospital.
MORE FROM MICHIGAN: Sign up for our weekly newsletter
"Once we got to U of M, they were treating him to keep him alive," Elizabeth said. "The condition was undiagnosed—they just knew that his left ventricle was not functioning properly."
Sullivan, who was born on Feb. 22, 2019, was stabilized in the pediatric cardiothoracic intensive care unit at Mott. To this day, it's not entirely known what caused his condition.
"We think most likely he suffered a massive heart attack as a newborn," pediatric cardiothoracic surgeon Jennifer Romano, M.D., said, calling his condition "complex and rare."
This severely damaged his left ventricle to the point where it was not functioning. Once Sullivan was stabilized in the pediatric cardiac ICU, his care team and family decided on a best path forward: a hybrid palliation performed by Romano and interventional pediatric cardiologist Jeffrey Zampi, M.D., when Sullivan was 10 days old.
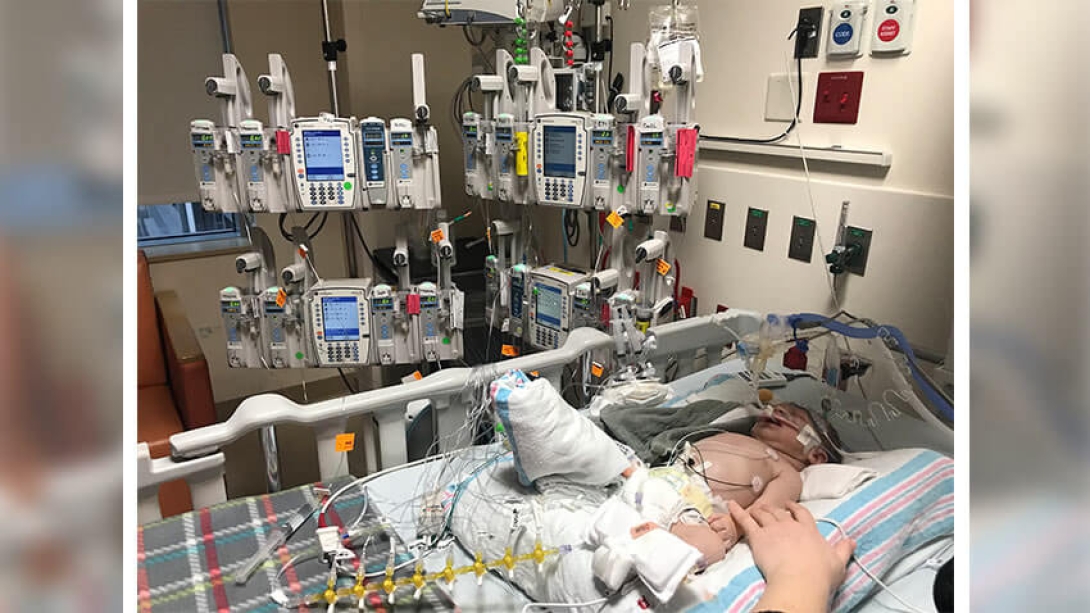
Undergoing a hybrid procedure
A hybrid procedure combines minimally invasive catheter techniques performed by Zampi with surgical techniques performed by Romano.
"When we talk about a hybrid procedure, what that means is any procedure where you combine surgical and catheter-based techniques at the same time," Zampi said. "Dr. Romano and I work really closely together—shared decision making and shared technical expertise—and by combining those different skill sets, you get the best of both: a procedure that's as minimally invasive as possible but also as effective as it can be."
Hybrid procedures can be used in a variety of high-risk patients ranging from those born with only a single pumping chamber or ventricle to those with complicated forms of congenital heart disease where the heart may have many abnormalities and require a complex repair down the road. The team within the Congenital Heart Center at Mott is one of only a handful in the country with extensive experience in the use of the hybrid procedure in both of these situations.
The Mott team was able to apply their experience to Sullivan's unique situation. The goal with Sullivan's hybrid procedure was to give him a stable circulation while allowing his left ventricle to recover, if possible, from whatever had impaired the function or, at the very least, to buy him time while waiting for a heart transplant.
"This approach is what we use for the highest-risk cases," Romano said. "It's a way to stabilize a sick newborn… to get a stable physiology, get them off a ventilator, and have them be able to go home and grow.
"When we look at any patient, we look at what's going to give them the best quantity and quality of life," she added.
During Sullivan's hybrid procedure, bands were placed on Sullivan's pulmonary arteries to restrict some of the blood flow while a stent was placed between the aortic and pulmonary artery to assure unobstructed blood flow to the body. He was added to the heart transplant list and began his recovery in the pediatric cardiac ICU.
A healing heart
After seven weeks in the hospital—living in Sullivan's room or at the nearby Ronald McDonald House—Elizabeth and Brandon got some amazing news.
"One day, one of the heart transplant doctors came in and told us that they had seen a slow progression of his left ventricle starting to repair itself and function more than it had," Elizabeth said. "So they said, 'If his heart is healing, we should give him time to see how it heals.'"
His heart was healing so well, in fact, Sullivan was moved to inactive status on the heart transplant list, meaning his care team thought he wouldn't need a transplant after all.
"After being told how unlikely it was that his heart would recover, we were shocked to find out that it was beginning to heal itself," Elizabeth said. "His incredible strength alongside the amazing medical care he received in those first weeks of life is truly, in our eyes, a miracle."
With Sullivan getting stronger, the family was finally able to go home to Canton, Michigan, in April 2019 when he was 8 weeks old.
"There were a lot of ups and downs when we were in the hospital for those weeks. He went into cardiac arrest twice; it was really touch-and-go. For us to come home was a really big deal," Elizabeth said.
It was always known that a second surgery would be needed—whether a heart transplant or another option. But thanks to the initial hybrid procedure, he was able to go home and live a relatively normal babyhood until the second surgery was needed.
Back at Mott
In December 2019 when Sullivan was just shy of 10 months old, he returned to Mott for a second surgery. His care team had decided it was time to see if his heart could function on its own. This surgery essentially undid what was done during the hybrid procedure with the goal of having Sullivan's heart function normally on its own.
"Sullivan had two ventricles and a structurally normal heart, he just had this heart attack," Romano said of why he was a good candidate for this procedure.
The hybrid surgery had allowed his heart to rest and heal for almost 10 months. That meant he was bigger and stronger—a very good thing because he did have several post-operative complications.
A few days after the surgery, Sullivan had to be put on ECMO, a form of life support, for three days as his heart and lungs recovered. All told, he was in the hospital for three weeks.
"He progressively got better, day by day," Elizabeth said.
Sullivan today
Since coming home, Sullivan has been flourishing.
'He's been healing and growing, and his heart is functioning solely on its own," Elizabeth said. "He's on two blood pressure medicines, and his left ventricle is technically mildly depressed still, but his body doesn't know any different so it's just been growing and accommodating that."
At almost three years old, Sullivan is "very feisty," said Elizabeth. "He has lots of personality. He's very funny. He's very loving—he's got a perma-smile on his face."
Zampi sees him every 6 to 12 months in his clinic and expects no future surgeries for Sullivan.

"Even when he was sick or when he came to the clinic after his surgery, he was always the happiest baby. His parents are the nicest people—you can tell he comes from a place of love," Zampi said, the affection apparent in his voice.
Both Romano and Zampi credit his devoted parents with how well he's doing. It's the teamwork between Romano, Zampi, the rest of the Congenital Heart Center staff at Mott, and patient families that make these complex procedures a success.
"When we have a patient like Sullivan born with really complex problems, we get together and discuss in a large group what's the best path forward—all of us taking all of our expertise and years of experience and different vantage points together," said Romano.
"Heart center-wide, we all put our heads together to make decisions that are right for families and incorporate families in the decision-making process so they have a voice," added Zampi. "We try to guide people along the pathway and also listen to their needs and wants, and I think that's pretty unique to our Heart Center."
Like Podcasts? Add the Michigan Medicine News Break on iTunes or anywhere you listen to podcasts.

Explore a variety of healthcare news & stories by visiting the Health Lab home page for more articles.

Department of Communication at Michigan Medicine
Want top health & research news weekly? Sign up for Health Lab’s newsletters today!