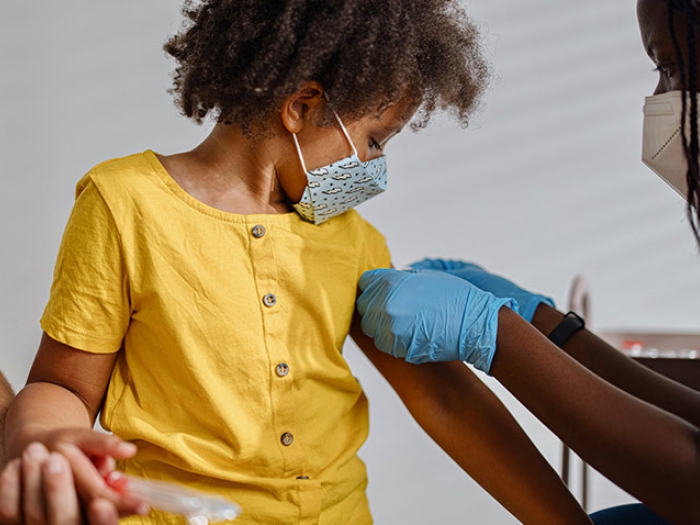
Physicians share advice on how parents and coaches can best handle, and avoid, any curveballs thrown their kid or athlete’s way.
6:00 AM
Author |

When it comes to keeping children safe during school or community athletics, most parents and coaches are diligent in covering their bases. But while many know that emergencies can happen, few feel comfortable handling them, especially when lesser-known about, but extremely critical, situations arise, such as a heat stroke or sudden cardiac arrest.
Here, pediatric cardiologist Monica Goble, M.D., pediatric sports medicine physician Ingrid Ichesco, M.D., and internal medicine, pediatric and sports medicine doctor Rebecca Northway, M.D., from C.S. Mott Children's Hospital share safety tips that every parent and coach should know, and ways to handle some of the most common, to the most serious, problems you might face on the field, in the rink, or on the court.
Concussion awareness
A concussion, or mild traumatic brain injury, occurs when force is transmitted to the brain.
"A concussion isn't an injury you want to play through," Ichesco says. "If an athlete has a concussion and sustains another hit to the head, it can be very dangerous and will most likely make symptoms worse."
LISTEN UP: Add the new Michigan Medicine News Break to your Alexa-enabled device, or subscribe to our daily updates on iTunes, Google Play and Stitcher.
To prepare for the possibility of a concussion, Ichesco advises:
-
Wearing appropriately fitting head protection. Although helmets and mouth guards don't prevent concussions, they could protect from skull fractures and dental damage.
-
Having kids be aware and notifying an adult immediately if they experience any vomiting, headaches, or neck pain.
-
Reminding your child to play respectfully and follow the rules of the game.
If you're concerned a concussion has occurred, Ichesco suggests:
-
The rule "when in doubt, sit them out."
-
Recognizing red flags, such as vomiting, complaints of a severe headache, concern about a serious neck injury or prolonged loss of consciousness (greater than one minute) and seeking urgent evaluation if any are present.
-
Obtaining medical clearance from a health care provider before returning to activities.
-
Gradual return-to-play progression, directed by a medical professional, once symptoms have resolved.
SEE ALSO: The Dangers of Untreated Concussions in Kids' Sports

Emotional trauma
Although emotional abuse issues have finally surfaced in recent years, the problem still remains a serious one across all sports.
Athletes and teams strive for wins and perfection, which puts pressure on athletes and coaches. Various actions and words may be perceived as helpful in building physical and mental toughness, but they border a fine line before they're considered abusive.
"It's important to increase awareness of emotional abuse, which can be more difficult to pinpoint than physical or sexual abuse," Ichesco says. "Sports should be fun, safe and promote lifelong fitness."
Here's what parents and coaches can do to help:
-
Educate athletes about emotional abuse and trauma, and empower them to tell an adult.
-
Ensure children are not left alone with one supervisor; there should be at least two present, with one ideally not a parent, in order to protect all parties involved.
-
Promote a culture where all levels (coaches, parents, children, administrators) are aware of emotional abuse and bring awareness to appropriate ways to report concerns. SafeSport, a nonprofit organization, is a resource that provides educational information on emotional abuse and reporting misconduct.

Heat safety
Heat illnesses are often thought to occur in hot weather, but it can happen even in cooler temperatures, says Northway. Signs of overheating include muscle cramps, passing out, a brief loss of consciousness, heat exhaustion and most dangerous of all — heat stroke.
A heat stroke is associated with neurological changes, such as confusion, agitation or seizures. Heat stroke can occur when heat production and environmental heat exceed the body's thermoregulatory capacity.
If a player is overheated, cool them quickly by icing the groin, armpits and misting them with cool water. The treatment for heat stroke requires a full body cooling within 30 minutes, Northway states.
MORE FROM MICHIGAN: Sign up for our weekly newsletter
"Make sure to avoid vigorous exercise if possible when temperatures, humidity and the heat index are high," Northway says. "These are some basic pieces of advice everyone can implement to stay as healthy as possible while being active."
Along with tips for handling them, Northway says recognizing these signs of heat illnesses are crucial:
-
For heat cramps -- which occur in the stomach, arms or legs -- require athletes to stop activities and rest. Consuming cold fluids, particularly those containing sodium and carbohydrates, as well as icing, are recommended.
-
If a child has briefly fainted, move them to a shaded, cool area to rest and elevate their legs while helping them rehydrate.
-
If heat exhaustion or a stroke is suspected, call 911 immediately.

Proper hydration
Hydration is important for muscle function, blood pressure, circulation, cardiac function and temperature control. It reduces the risk of heat illnesses and enhances recovery. Signs of dehydration include thirst, fatigue, headache, dizziness, nausea, vomiting and muscle cramps.
"Make sure your child is drinking enough water throughout their activities," explains Northway. "It's an easy, steadfast rule that all parents and coaches can follow to keep children happy, healthy and safe."
Northway says these tips can help prevent any athlete from drying out:
-
Make fluids easily accessible and available at all times.
-
Be familiar with signs of dehydration prior to and while activities are happening, which includes weight loss, complaints of darker colored urine (lemonade colored or darker) and/or low urine output.
-
Athletes should pre-hydrate a few hours in advance to allow for adequate body absorption. Consuming beverages or foods with sodium and salt can help stimulate thirst and the retention of fluids.
-
During exercise, fluids should be consumed frequently, especially if the activity lasts more than one hour. A simple rule to follow? "Drink 5-10 ounces every 15-20 minutes during vigorous exercise," says Northway.

Sudden cardiac arrest
During a sudden cardiac arrest, the heart's rhythm suddenly becomes abnormal. For no apparent reason, a person suddenly drops due to ineffective blood supply to the body.
Quick action is essential to survival and neurological recovery, as minutes matter during these unexpected episodes. An abnormal heartbeat, untreated, may deteriorate rapidly to no pulse.
"This occurs in all age groups and in both athletes and non-athletes," Goble says. "If a person is experiencing a sudden cardiac arrest, act quickly. Your timely response may be the difference between life and death."
An automatic external defibrillator (AED) is crucial in a suspected cardiac arrest case. An AED, a computerized medical device that analyzes a person's heart rhythm, will recognize a shockable rhythm and advise the operator whether the person should be shocked.
Goble says signs of a sudden cardiac arrest include:
-
Abnormal breathing, air gasping, or absent breathing.
-
The person may appear limp or to be having a seizure.
During the urgent situation, Goble stresses the following:
-
Call 911 immediately and begin CPR to help circulate the blood.
-
Quickly apply an AED, ideally within three minutes of the collapse.
-
Once the AED is applied, the machine will analyze the heartbeat and decide if a shock is necessary to reset the heart's electrical system to help it return to normal. The sooner the AED is applied, the better the chances are for a full recovery.
-
Continue CPR until emergency medical services have arrived.
For school-based activities, some facilities in Michigan have been designated as a MI HEARTSafe School, meaning the school has been prepped for a cardiac emergency. Mott also works to educate schools in Michigan through their Project Adam Michigan initiative.

Weather preparedness
Keeping an eye on the weather before a game or event can be crucial to an athlete's safety. Many sports are played outdoors and unexpected storms can occur. Lightning strikes can cause permanent disability, or even death. Tornados are relatively common in certain areas, and some sporting events have little protective coverage.
"What to do in case of a storm should be part of an official 'Emergency Action Plan'," says Ichesco. "Having a set of instructions to follow and keep in mind can make serious situations more manageable."
Ichesco suggests the following for staying safe during severe weather situations:
-
Have a designated person watching the weather. Parents, coaches, organization leaders or school administrators should also check the local forecast before any game.
-
Be aware of storm warnings or watches in the area.
-
Recognize impending storm signs, like darkening clouds and increased winds, and remember it doesn't have to be raining for lightning to strike.
-
Be aware of shelters and safe places to head to.
-
Avoid standing in an open field or in standing water.
-
Wait at least 30 minutes after the last lightning strike to resume play.
SEE ALSO: Hurricanes, Fires, Floods: It's Best to Be Prepared
In addition to the scenarios above, all three experts recommend organizations develop an Emergency Action Plan (EAP), which is an established and practiced safety document that outlines steps to take in case of a medical emergency. For sporting events, this should include an action plan for inclement weather, injuries, a downed athlete, coach or spectator, that staff should be aware of.
"We often think of emergency preparedness as a topic for large sporting events, but every sporting team, from football to tennis, should have an emergency action plan in place," Northway says.
Parents should ensure coaches are aware of their organization's EAP document and that they're prepared for any medical emergencies. And coaches should consider standardizing a pre-event "Safety Time-Out" to review a simplified EAP checklist that includes athletic directors, trainers, team physicians, stadium managers, security officers, school administrators and local EMS providers.
"It is well-documented that having emergency action plans lead to both lives saved and reduced injury rates," says Northway.

Explore a variety of healthcare news & stories by visiting the Health Lab home page for more articles.

Department of Communication at Michigan Medicine
Want top health & research news weekly? Sign up for Health Lab’s newsletters today!