Springtime brings allergy symptoms for many. A Michigan Medicine specialist explains how best to help a child get through a season of sniffles.
7:00 AM
Author |

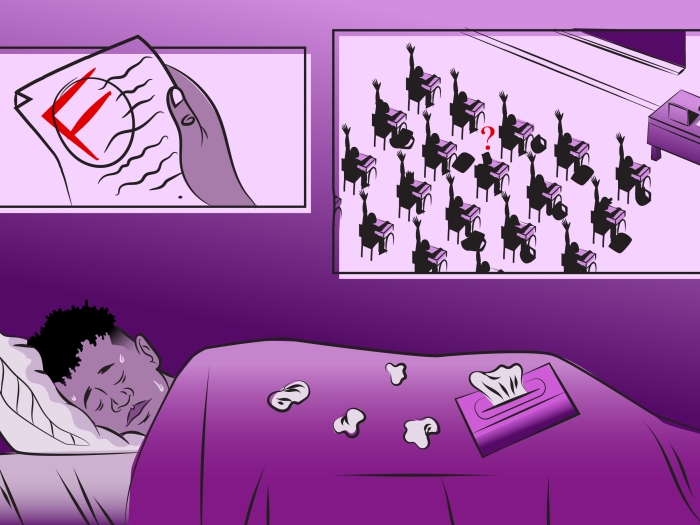
For some kids, the return of spring means more than warm weather and a break from school: Plenty will also experience sneezes, runny noses and watery eyes.
MORE FROM MICHIGAN: Sign up for our weekly newsletter
"When a child has uncontrollable seasonal allergies, it can significantly affect their entire life," says Georgiana Sanders, M.D., a pediatric allergist at University of Michigan C.S. Mott Children's Hospital.
Parents might turn to over-the-counter allergy medications to help.
More than half of families — 55 percent — did so within the past year, according to a new University of Michigan C.S. Mott Children's Hospital National Poll that examined how households with children ages 6 to 12 handle allergy season.
Just like adults, young people with allergies may face consequences without proper treatment.
"They don't sleep well; they don't perform well at school during the day," Sanders says. "I've seen it affect their sporting activities because they're miserable outside."
But treating a child with antihistamines — which work to block histamines that the body makes during an allergic reaction — often comes with questions.
Sanders spoke about the recent survey and gave some advice to families:
Tips for giving allergy medication to kids
Survey your environment first: Parents might try to reduce outdoor triggers before giving medication. One method: timing. "We obviously can't avoid trees and grass, but we know they produce more pollen in the morning and around dusk — so limit your time outside during those hours," Sanders says. She also advises a shower before bedtime to wash any pollen from the skin and hair. And consider a neti pot or sinus rinse bottle, devices that Sanders dubs "a shower for your nose."
Consult an expert if needed: Nearly two-thirds of parents asked a doctor about their child's seasonal allergies, the Mott poll found. Others sought advice from their pharmacist or a friend or family member. Sanders encourages parents to talk to their doctor about allergies and to pay close attention to labels when seeking allergy medication on their own. Eye drops that claim to treat "red" eyes, for instance, aren't effective for allergies.
SEE ALSO: Your Pediatrician vs. Urgent Care: What to Do When Your Child Is Sick
Children's medication is rarely different: Only 1 in 7 poll respondents reported giving a child adult allergy medication, but there is no variation between most antihistamines marketed to children and those for adults. The former is typically produced in liquid or chewable form, so it usually comes down to ease of consumption. "It all depends what's best for the child while maintaining the proper dose and controlling the symptoms," Sanders says.
Know when to medicate: Deciding when to administer allergy medicine might depend on the circumstances. Because antihistamines work relatively fast, "you can take them when you start having symptoms," Sanders says. "But if you're having symptoms three or four days a week, you'll be much better taking them preventively." Nasal steroid sprays, on the other hand, take time to kick in and are best started a week or two before pollen season begins, Sanders says.
Monitor a child's reaction: In a perfect scenario, the allergy medication will do its job without incident. But watch for any side effects, most notably sleepiness — which is less common with nonsedating antihistamines. "Sometimes you'll see mood changes or bad dreams, headache or stomachache," says Sanders, noting these occur rarely. She discourages regular use of decongestants, however, as they can disrupt sleep and increase heart rate.
Check the expiration date: About 1 in 5 parents have given a child expired allergy medication, the poll found. Although unlikely to be dangerous, outdated meds may lose their potency — a scenario that isn't ideal for youngsters made miserable by their symptoms. "There are always concerns with an expired medication," Sanders says, adding that parents also should check a liquid medicine to see if it looks different or cloudy.
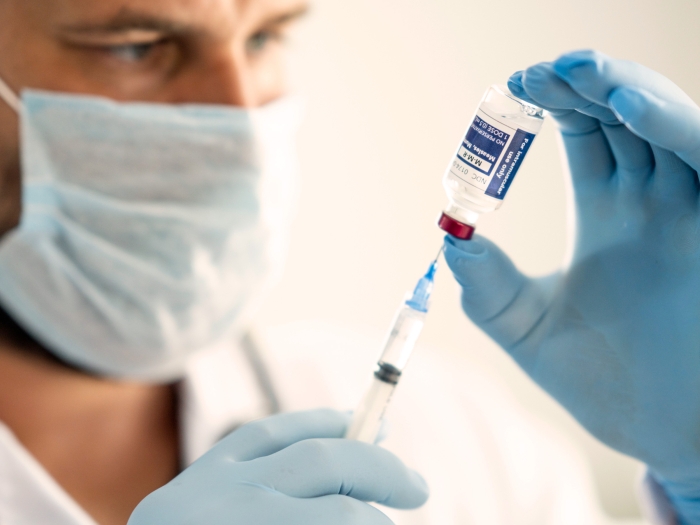
Consider further action when necessary: If avoiding outdoor triggers and trying over-the-counter antihistamines prove ineffective — or if a child is unable to follow either regimen —allergy shots may be an option. Also known as immunotherapy, the shots act to stop the reaction, not treat symptoms. And they work for about 85 percent of recipients. "Many people can significantly reduce medication use while still getting good relief," Sanders says.

Explore a variety of healthcare news & stories by visiting the Health Lab home page for more articles.

Department of Communication at Michigan Medicine
Want top health & research news weekly? Sign up for Health Lab’s newsletters today!