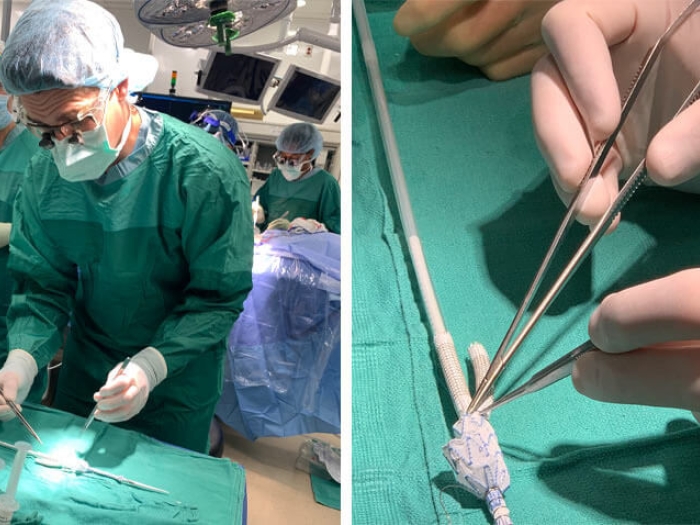
Also known as an aortic aneurysm, this condition can be deadly if left undiagnosed. Learn more about who is at risk for enlarged aorta.
7:00 AM
Author |
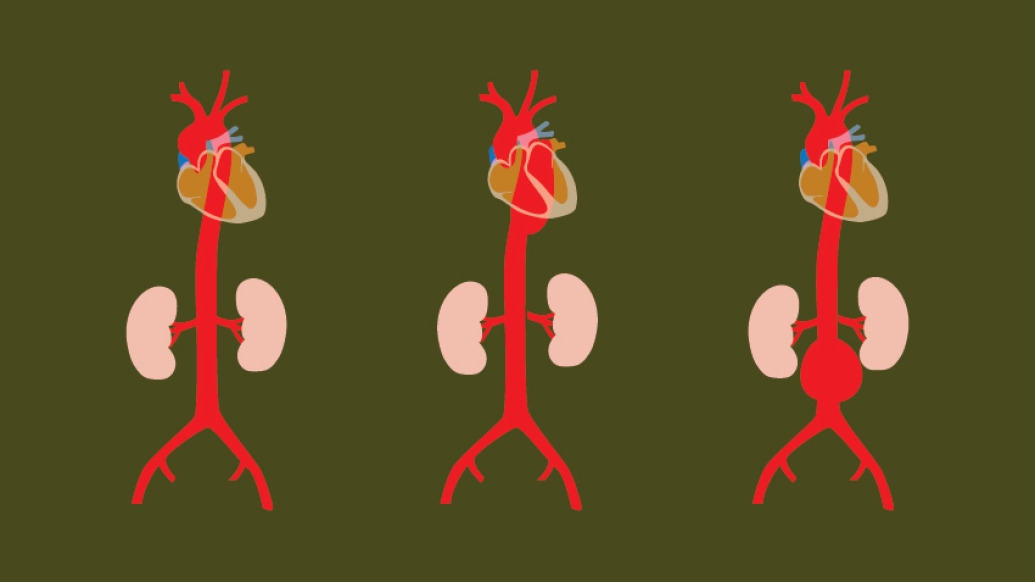
Each year in the United States, aortic aneurysms contribute to nearly 20,000 deaths. But with awareness, monitoring and proper care, aortic aneurysm treatment can be relatively simple — often with a minimally invasive procedure if surgery becomes necessary.
MORE FROM MICHIGAN: Subscribe to our weekly newsletter
To raise awareness of aortic aneurysms, also known as an enlarged aorta, Michigan Medicine vascular surgeon Jonathan Eliason, M.D., outlines the symptoms and risk factors.
What are enlarged aorta symptoms, and how is it diagnosed?
Eliason: An individual with an enlarged aorta typically experiences no symptoms until the aneurysm ruptures. In most cases, this means an aortic aneurysm wouldn't be discovered unless some type of screening was performed that allowed aortic measurements. Aortic aneurysm screenings are recommended for certain individuals, depending on their age, gender, family history and other risk factors.
Screening is typically done via an ultrasound scan, a painless test that uses sound waves to create images of organs and structures inside the body. If an aneurysm is detected, its size can also be measured by ultrasound.
What are enlarged aorta risk factors?
Eliason: Because the condition can be hereditary, screening is recommended for men or women over age 65 who have a person in their immediate family with an abdominal aortic aneurysm (AAA). Men over 65 who have smoked more than 100 cigarettes in their lifetime should also be screened. According to the U.S. Preventive Services Task Force, this group stands to benefit the most from early detection and surgical treatment due to a higher prevalence of larger AAAs compared to other patient groups. Routine screening is not recommended for women, who are at lower risk for AAAs.
Individuals with connective tissue disorders, such as Marfan or Loeys-Dietz syndromes, are more likely to experience an aortic aneurysm at a younger age and should be closely monitored.
The vast majority of patients with an AAA do not have a family history and instead have other risk factors. Smoking is by far the strongest risk factor for aortic aneurysm, even a remote history of smoking cigarettes or breathing secondhand smoke. Uncontrolled high blood pressure is also a risk factor, though far less than cigarette smoking. Hardening of the carotid or coronary arteries contributes as well. We often order testing in these areas if a patient has an AAA.
How much can an aorta stretch before it could burst?
Eliason: The average aorta is approximately 2 cm, or slightly smaller than one inch. An aneurysm means that the diameter is 1.5 times larger than normal, or 3 cm, in the abdominal aorta.
SEE ALSO: Observe or Operate? When an Enlarged Aorta Requires Action
The rupture rate really increases at 5.5 cm in men and 5 cm in women. That doesn't mean an aneurysm can't rupture at a smaller diameter or at a larger diameter, but these tend to be the sizes where surgery is actively considered. If a person has a connective tissue disorder, aneurysm repair may be considered at a smaller size.
What happens if an aneurysm ruptures? Is there any warning?
Eliason: During an abdominal aortic aneurysm rupture, an individual typically experiences severe abdominal or back pain. Sudden death can also occur. In some cases, patients might experience symptoms without a rupture. These patients may get a warning of abdominal pain or escalating back pain. If the aneurysm is in the chest only, the individual may experience chest or upper back pain.
Is an individual with an aortic aneurysm more likely to experience another aneurysm?
Eliason: Yes. One study reported that just over a quarter of individuals with an abdominal aortic aneurysm had a simultaneous thoracic aortic aneurysm. This suggests that thoracic aortic aneurysm screening is appropriate for patients with abdominal aortic aneurysms.
Is there anything else individuals should know about risks associated with an enlarged aorta?
Eliason: Yes, anyone diagnosed with an abdominal aortic aneurysm is more likely to have atherosclerosis (hardening or blockages) in other arteries. This may put them at an increased risk for other cardiovascular conditions such as heart attack or stroke. Screening for these conditions may be indicated.

Explore a variety of healthcare news & stories by visiting the Health Lab home page for more articles.

Department of Communication at Michigan Medicine
Want top health & research news weekly? Sign up for Health Lab’s newsletters today!