Ophthalmologists take photos of a patient’s eyes to monitor good health and track progress of disease. Here are some common ways the images are taken.
7:00 AM
Author |
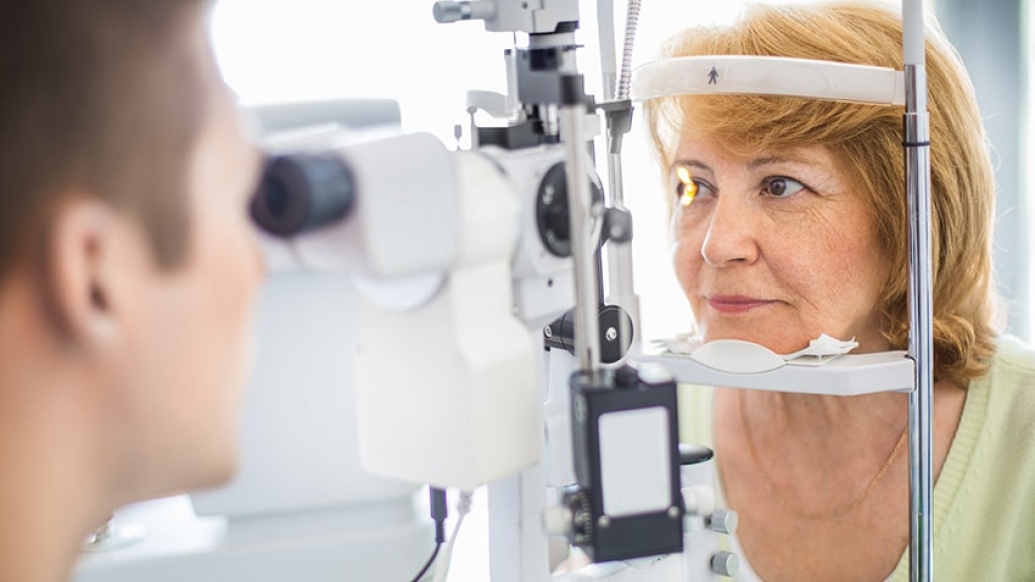
Ready for your close-up?
If you're going to the eye doctor, either for a routine exam or an existing issue, you should expect to have photos taken of your eyes.
MORE FROM MICHIGAN: Subscribe to our weekly newsletter
Those images, after all, are a key part of preventive care. They can help your ophthalmologist look for problems — and, if any are detected, to diagnose an issue and monitor it (or pursue treatment).
The tools offer valuable insight: "This technology can see things that we can't," says Timothy Steffens, director of imaging and information systems at the University of Michigan Kellogg Eye Center.
Some methods capture the surface and surrounding areas of the eyes; others go deeper to survey the inside and back of the eye.
Each type of ocular photography is quick and simple. None require special preparation or involve any pain for the recipient, Steffens notes. Patients, he adds, needn't be scared.
He spoke more about common ways that images of an eye are obtained:
How ophthalmologists take eye photos
Standard digital camera: A basic 35mm digital camera may be used to document patients diagnosed with an external condition or disorder. Among them: droopy eyelids, Graves' eye disease, proptosis (when an eyeball protrudes) and skin cancer in or around the eye. "We use standard protocols so the images are consistent from visit to visit," Steffens says.
Slit lamp biomicroscope: The same tool your ophthalmologist uses to examine your eye. It uses a narrow beam of light and magnifies the view of the front of the eye. Says Steffens: "We're recording corneal diseases, cataracts and ocular tumors."
SEE ALSO: Making Prosthetic Eyes That Look Like the Real Thing
Fundus photography: A digital camera attached to a low-powered microscope gives a close-up view of the retina, optic nerve and macula. "You're using conventional photo techniques here with the help of dilation and the special optics in the fundus camera," Steffens says. It can also help ophthalmologists monitor changes in a patient's retina over time — and spot warning signs such as leaky hemorrhages caused by diabetic retinopathy and macular degeneration.
Optical coherence tomography (OCT): This technology involves a low-powered laser that goes through the pupil (although "we don't even touch the eye," Steffens notes) to measure thickness in the back of the eye — crucial for determining progression of and treatment for a variety of disorders, including macular degeneration, optic neuritis and glaucoma. The method, he adds, "has become a standard of care."
Fluorescein angiography: Also using a fundus camera, this diagnostic test requires a patient receive an injection of fluorescein dye in his or her arm just like when blood is drawn. The dye travels through the body to the eye's blood vessels in about 15 seconds — and the resulting contrast allows doctors to more clearly notice signs of diabetic retinopathy, vein and artery occlusion, edema and tumors.

Explore a variety of healthcare news & stories by visiting the Health Lab home page for more articles.

Department of Communication at Michigan Medicine
Want top health & research news weekly? Sign up for Health Lab’s newsletters today!





