These trained professionals work to prevent and treat injuries during practice and competition and can assist in a variety of other situations.
7:00 AM
Author |
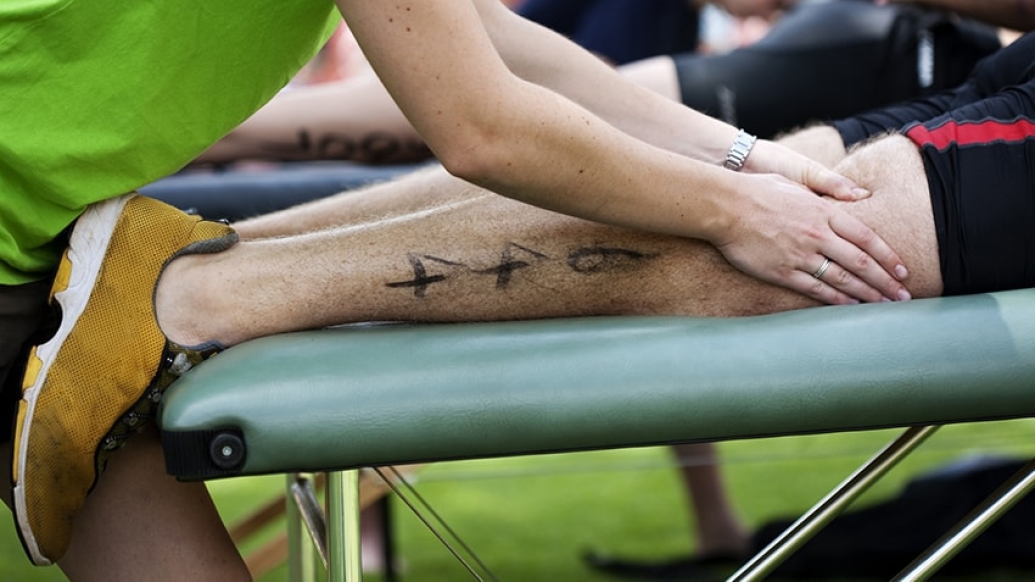
On and off the field, athletic trainers wear many hats.
Regardless of setting or situation, however, the intent is the same.
MORE FROM MICHIGAN: Sign up for our weekly newsletter
"The whole purpose is to protect our athletes from getting hurt in the first place — and if they do get hurt, to help them get back in the game," says Jere Freeman, A.T.C., a supervisor for clinical assistive personnel at Michigan NeuroSport, a Michigan Medicine program that specializes in neurologic care for athletes.
All athletic trainers, he adds, follow three key tenets: "prevention, protection and rehabilitation."
One means of doing so is psychological: build a rapport among clientele with frequent contact, sometimes on a daily basis. Over time, then, a positive relationship might better spur athletes — hypercompetitive ones in particular — to speak up when something isn't right.
"You want them to come to you when they have an injury," says Freeman. "Having their trust is really important."
The connection extends beyond team sports. Patients recovering from concussion and some surgeries also can benefit from regular contact with the same athletic trainer, he notes.
Freeman explained common scenarios where athletic trainers can help:
On the playing field or court: High school and collegiate sports teams keep athletic trainers on-site at practices and games — a legal requirement in most states. Typically, they help quickly address and treat minor injuries (such as a sprained ankle or dislocated shoulder) without a doctor visit. And they might field basic medical queries from players.
SEE ALSO: The Dangers of Untreated Concussions in Kids' Sports
Because athletic trainers also learn how to handle more serious outcomes such as traumatic neck or back injuries, they're crucial when one does occur. Says Freeman: "A big part of an athletic trainer's job is their training in emergency medicine and evaluating injuries … providing immediate care as well as guiding parents and families toward emergency services if needed."
After orthopedic surgery: People who undergo orthopedic surgery are also likely to get face time with an athletic trainer. Athletic trainers in a clinical setting, Freeman says, assist throughout the process by prepping a clinical schedule, managing the flow of patients, administering functional tests before a doctor's consultation and ultimately serving as liaisons between physical therapists and surgeons on behalf of the patient.
They also serve as partners during postsurgical rehabilitation. An athletic trainer will often work with patients who have exhausted their insurance benefits for physical therapy. Says Freeman: "We'll give them an exercise progression — strength and balance training, sports-specific drills … giving them activities curtailed to their special needs going forward."
When a concussion lingers: If an athlete shows signs of a concussion that aren't improving, he or she might meet with an athletic trainer as part of the care team. "The majority of people we meet are still symptomatic," says Freeman. An athletic trainer will step in to gauge patients' level of ability (and injury) through diagnostic exams as part of a Michigan NeuroSport appointment.
Athletic trainers put patients through physical tests that might include sprints or stationary biking — activities meant to exacerbate concussion symptoms, albeit briefly. The reason: "It's just a gradual, monitored progression to see what their limits are," Freeman says, "and to establish a guideline to where they should be while working out on their own." The tests repeat in future visits.

Explore a variety of healthcare news & stories by visiting the Health Lab home page for more articles.

Department of Communication at Michigan Medicine
Want top health & research news weekly? Sign up for Health Lab’s newsletters today!