'Every day is a good day’: a meaningful doctor-patient relationship that changed everything.
11:37 AM
Author |
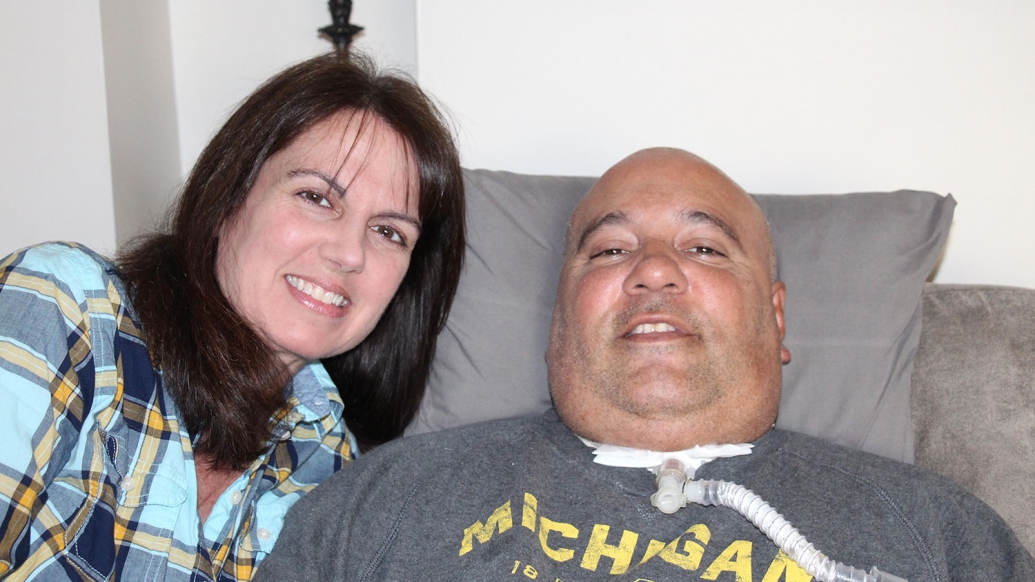
In June 2018, Matt Sirianni began losing some motor functions and found himself struggling to walk. It seemed odd for the otherwise healthy adult in his late 40s.
Yet a full year of neurological infusion treatments at Michigan Medicine turned out to be ineffective, and Matt was eventually referred to the organization's Pranger ALS Clinic.
ALS — which stands for amyotrophic lateral sclerosis and is also known as Lou Gehrig's Disease — is a progressive disease that weakens muscles and impacts physical function. It is typically terminal.
"Getting such a diagnosis can be frightening, but all I know is that when we got to the clinic, everyone was so supportive and spent so much time giving us information and making us feel comfortable," Matt said.
The clinic is where Matt met his pulmonologist, Philip Choi, M.D. It served as the beginning of a patient-physician relationship that changed Matt's life forever.
Quick deterioration
Choi's role at Michigan Medicine is to work with patients who need assistive breathing devices such as respirators and ventilators.
He helps lead the Assisted Ventilation Clinic, which was established in 2009 and now treats nearly 1,200 patients annually.
Like Podcasts? Add the Michigan Medicine News Break on iTunes, Google Podcast or anywhere you listen to podcasts.
While the clinic has gained increased visibility during the pandemic — as the use of ventilators became essential to aid the most seriously-ill COVID-19 patients — the Assisted Ventilation Clinic team has worked tirelessly over the years to help all types of patients, including those with ALS.
"Commonly, patients with ALS eventually need devices that can replace their respiratory muscles, which are deteriorating," Choi said. "That will often involve a tracheostomy, and so I had that discussion with Matt and both he and his family were adamant that a trach was not a path he ever wanted to go down."
Just months after meeting Choi, however, Matt found himself unable to breathe. He was diagnosed with pneumonia and transferred from his home hospital back to Michigan Medicine's intensive care unit, where Choi once again met with him.
"I really didn't think there was going to be much quality of life left if I went on a ventilator full time," Matt said. "And Dr. Choi listened to those concerns with empathy while I prepared for palliative care. But then he shared his own thoughts about what I could do with a trach — which included still being able to travel, see my kids and stay productive. He knew exactly what was important to me."
So Matt decided to get a tracheostomy, allowing his lungs to be hooked up to a ventilator, which mechanically helps him breathe.
The Trach Trail
Following his tracheostomy, a team from the ventilation clinic sprang into action. He and his family started down what the clinic calls "The Trach Trail."
"The trail is a set of steps that we have put in place to make sure our inpatients will be cared for safely once they return home," Choi said. "They will ensure you and family members know how to work the ventilator and trach, and be able to troubleshoot any problems that may arise."
Those who offer the training include doctors, nurses, nurse practitioners, respiratory therapists and more. Patients can also meet with social workers and nutritionists.
And once patients are discharged, they are never on their own.
"Things were definitely overwhelming when we got home," said Laura Sirianni, Matt's wife. Laura and Matt's sister, Sue, help with Matt's caregiving. "But the vent clinic checked in on us immediately and we knew that we could reach out 24 hours a day if we needed."
Indeed, that's one of the perks of the vent clinic — Julie Hanley, a nurse practitioner, and Armando Kurili, a respiratory therapist, have worked in the clinic for years and have specific expertise in home ventilation. They are both available throughout the week for patient calls to make sure patients get the care they need.
It's a service that's much appreciated by Matt's family.
"It's hard to believe the level of support and training we received from Michigan Medicine," Laura said. "We're able to provide ICU-level care to Matt while allowing him to live at home."
'I'm just so thankful'
For Matt, his experience with Choi and other Michigan Medicine team members has given him a renewed perspective on life.
"I know my time is limited, but as far as I'm concerned, every day is a good day," Matt said. "I'm hoping for at least five more quality years ahead. And that's because of a decision I was able to make and the assistance we've gotten from our doctors, nurses, respiratory therapists ... really everyone we've worked with at Michigan Medicine."
Matt saved his biggest thanks for Choi — and the personalized care he continues to provide.
"I'm just so thankful for the relationship Dr. Choi has forged with me," Matt said. "He took the time to understand me and I was able to really understand him. There's a level of trust between us, so I know that each health decision we make moving forward will be the right one."

Explore a variety of healthcare news & stories by visiting the Health Lab home page for more articles.

Department of Communication at Michigan Medicine
Want top health & research news weekly? Sign up for Health Lab’s newsletters today!





