After a lifetime with cystic fibrosis, rare transplant operation lets hockey coach, new dad breathe freely
10:11 AM
Author |
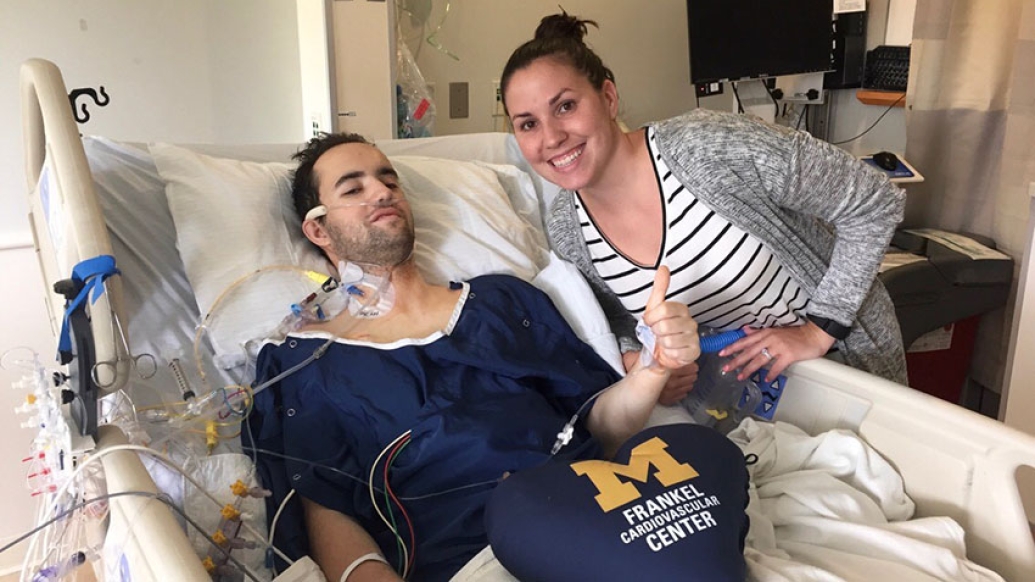
Christopher Newton found his second wind in August 2016.
After a lifetime of cystic fibrosis (CF), the 29-year-old Grand Rapids, Michigan, resident could barely complete a chore like washing dishes without becoming winded to the point of exhaustion. CF is a genetic condition marked by a buildup of thick mucus that damages the body's organs including the lungs and pancreas.
"I was on six liters of oxygen at the time, too," Newton says. "I'd get so tired just trying to breathe."
Because of his worsening lungs, he'd already stepped away from his livelihood as a high school hockey coach, so he and his caregivers had a life-changing conversation.
It was time.
He needed a lung transplant, a possibility that had followed him since childhood. Still, it surprised him. At the time, he was only 27 and a life-long hockey and lacrosse player. His breathing troubles didn't begin until 2014 when his medicinal treatment stopped helping his worsening lungs. Until then, he'd felt invincible.
Next step: transplantation
Newton was directed to the University of Michigan Transplant Center in Ann Arbor to have a double lung transplant. CF patients require a double transplant rather than a single lung because CF lungs contain bacteria that spread to the new lung if only one is implanted.
Lung transplantation is rare. U-M does 20-40 such cases a year of the nearly 2,000 completed in the United States annually. By comparison, nearly 18,000 kidney transplants occur in the United States annually.
Newton underwent a battery of tests to evaluate if he was healthy enough to endure the surgery but sick enough to need new lungs. They include blood work, an esophagram, EKG, bone density scan, a dental consultation and more.
Another prerequisite? He and his life partner, Jessie Matthews, whom he's known since high school, also were required to attend a lung transplant education class.

"The U-M team wants you to know everything," he says. "Your family is going through it all as much as you are."
Newton was paired with thoracic surgeon Philip W. Carrott, Jr., M.D. and pulmonologist Kevin M. Chan, M.D., the medical director of Lung Transplantation and Fellowship Training Program Director for Michigan Medicine's Division of Pulmonary and Critical Care Medicine. The duo gave him confidence because they always have a plan in place if complications arise during the transplant and the recovery, Newton says.
"Some of the statistics can look a little unfriendly," he says, referring to the survival rate. The one-year survival rate after a lung transplant is 87 percent while a five-year survival rate is 60 percent.
"I took the stance that there was no other option and all was going to be fine," he says. "The doctors seem like they had everything covered."
Getting the call while saying goodbye
Newton was on the organ donor list for two months. The typical wait is six months to a year.
When he received the call about available lungs, he was at his parent's house in Farmington Hills. He was there saying goodbye. His father, with whom he coached championship high school hockey, was upstairs dying from colon cancer.
"It was all pretty surreal," he says. "I was able to go upstairs, tell him I was getting new lungs and he acknowledged it and that was comforting."
Bill Newton, 55, died the day after his son's 14-hour transplantation, when his son was getting his second chance at life.
"I know he was looking over the whole situation," Christopher Newton says. "I know my dad would be so happy."
Recovery journey
Newton's been happy with his recovery. Two years post-surgery and his recovery has been without complications, with his lungs at normal capacity.
For six months, he stayed away from germ-carrying crowds and when he did go out to follow-up doctor's appointments, he wore a surgical mask and brought hand sanitizer. He didn't want to risk this gift of breath he received from a deceased prisoner; someone he could relate to as he was tethered to oxygen tubes for several months with no energy to go out.
"These lungs were considered high risk because of his lifestyle, and I know he was younger than me," he says.

Thus far, they've been an ideal match, thanks to the 20 or so anti-rejection medicines Newton takes, down from the 50 or so he had immediately following surgery.
"I remember the first breath I took in the hospital," he says. "It was the next morning after the drugs wore off and I had to ask Jess how far my lungs went down because I had never taken a breath so deep. I got a great set of lungs."
He relied heavily on the MyUofMHealth.org patient portal to keep up with his appointments and follow-up tests to make sure there are no signs of rejection, as well as correspond with his healthcare team, when he had a concern.
Getting his life back
The lung transplant restored Newton's life. He is working again, coaching hockey at East Grand Rapids High School, traveling, boating and doing dishes at home without getting winded.
"I have so much energy," he says.
Perhaps the biggest change is he and Matthews became parents. Because of his CF, the couple had to use in vitro fertilization (IVF) after the transplant because the disease makes conceiving troublesome.
Their first round of IVF worked. Liam was born October 30, 2018.
"My transplant improved my life in every way possible," Newton says.
To make an evaluation appointment with the Transplant Center, call a patient care representative at 1-800-333-9013.

Explore a variety of healthcare news & stories by visiting the Health Lab home page for more articles.

Department of Communication at Michigan Medicine
Want top health & research news weekly? Sign up for Health Lab’s newsletters today!