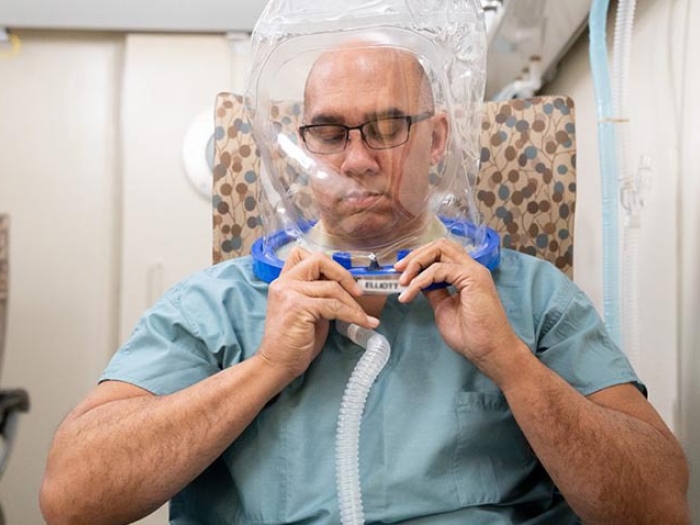
For patients with nonhealing wounds and other conditions, a boost in oxygen intake could be a way to accelerate recovery.
7:00 AM
Author |

Wounds need oxygen to heal.
In the case of serious wounds, then, a super-sized dose of oxygen can be the key to improvement for some patients.
MORE FROM MICHIGAN: Subscribe to our weekly newsletter
Known as hyperbaric oxygen therapy, such a boost "delivers oxygen to the tissues that don't have enough to be healthy," and may help, says Steven Haase, M.D., medical director of the Comprehensive Wound Care Clinic at the University of Michigan.
Hyperbaric oxygen therapy has been sought out by a growing number of patients and practitioners in recent years.
The U-M clinic, which offers the treatment five days a week, can simultaneously treat up to 10 individuals.
Haase, also a clinical associate professor of plastic surgery, answered some common questions about the outpatient procedure.
How does it work?
Contrary to what some people might assume, oxygen isn't blasted topically on the affected area. Instead, recipients breathe 100 percent oxygen via a transparent hood ("a bit like wearing a loosely fitting space helmet," Haase notes).
In some centers, a person lies on a table and is moved into a single-occupancy tube. At U-M, however, the oxygen is delivered in a group setting. Patients are seated upright in large recliner chairs or rest on a cot inside a pressurized room.
Why is it effective?
In two words, pressurization and oxygen. The chamber at the U-M clinic is pressurized — similar in practice to riding in an airplane — which, in turn, allows the body to carry more oxygen in the blood to stimulate healing.
SEE ALSO: 3 Tips for Seniors Visiting the Emergency Department
Those elements, Haase says, "are keys that drive the oxygen to dissolve in the blood and get it where it needs to go."
Who are candidates for this treatment?
Recipients typically include those with nonhealing wounds; bone or soft-tissue damage from radiation; and osteomyelitis. Certain diabetic wounds of the lower extremities are considered candidates for therapy.
Beyond a collapsed lung that hasn't been treated, there are few barriers that would exclude someone from participation. "People who are basically medically stable and healthy enough for moderate activity should do well in the chamber," Haase says.
How long might sessions last — and over how many visits?
Treatments are most often booked for a set number of visits, such as 20 to 30 total, and take place once per day, five days a week, Haase says. Each lasts 90 minutes and has several added rest breaks interspersed throughout.
A patient's progress is monitored during the course of the visits. That helps doctors determine whether to continue with further sessions or seek an alternate means of remedy.
What are the risks?
Due to pressure shifts, some recipients might experience vision changes — a temporary effect, Haase says. There also are concerns, he says, that the therapy could worsen cataracts, but studies so far aren't conclusive.
Higher oxygen levels can pose a fire hazard; patients must adhere to a lengthy safety list prohibiting certain items such as battery-powered devices, among other things, from the chamber.
But problems, Haase notes, are "very rare." Those with an existing air bubble in their sinuses or teeth might feel slight pain or have trouble clearing their ears; they can ask for a nasal decongestant to help.
To find out more, visit the Wound Care Clinic online, or call 734-936-9795 to make an appointment.

Explore a variety of healthcare news & stories by visiting the Health Lab home page for more articles.

Department of Communication at Michigan Medicine
Want top health & research news weekly? Sign up for Health Lab’s newsletters today!