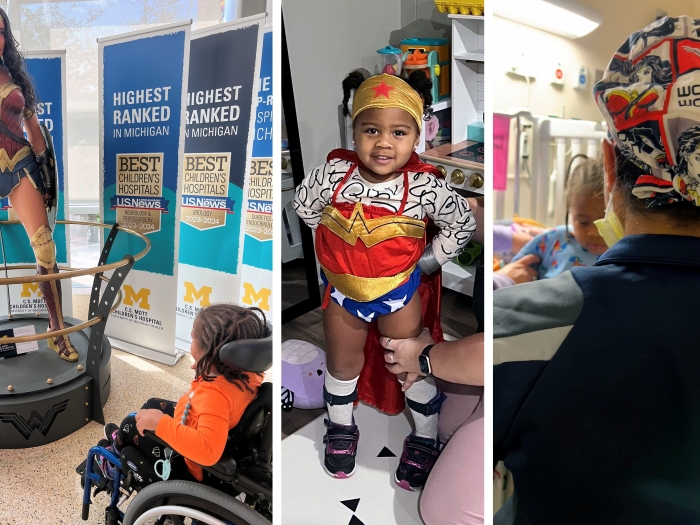
Rob Coleman had to sacrifice a lot while dealing with seizures, but after a successful laser ablation, the computer programmer is done planning around his epilepsy.
10:11 AM
Author |

After 12 years, Rob Coleman is breaking up with his neurologist. The Michigan Medicine patient from southeast Michigan is also back to being his own chauffer, letting his teenage eldest son off the hook.
LISTEN UP: Add the new Michigan Medicine News Break to your Alexa-enabled device, or subscribe to our daily audio updates on iTunes, Google Play and Stitcher.
Coleman, 44, hasn't had a known seizure in more than a year, since his July 2017 laser ablation for temporal lobe epilepsy. And as he tapers off his final seizure medication this winter, it's back to a full life that had been interrupted for more than a decade.
12 years of accommodations
Back in 2006, Coleman's wife, a nurse, realized something might be a little off. "She noticed when I was talking, all of a sudden I didn't know what to say or didn't understand an easy question," Coleman remembers. Three to four times a month, he was slipping into a state of confusion, which lasted around 30 seconds to a minute. It felt like he couldn't understand what was happening, even though he could tell someone was talking to him. "Then I'd come back, and say, 'wait a minute….'" he says.
Our goal with any surgery for epilepsy is the best chance of stopping the seizures without a patient noticing a difference in how their brain works.Emily Levin, M.D.
Coleman started seeing a neurologist and tried a couple of different medications. He was told not to drive until he could count six months without a seizure, which never came. So his eldest son, a newly-licensed driver at the time, became the second driver in the family. And Coleman's longtime employer agreed to let him start working from home. He remembers: "At first it was a little disheartening, thinking, 'I have to do all this, I have to live with this, and I'll be taking medications forever…."
MORE FROM MICHIGAN: Sign up for our weekly newsletter
Open brain surgery for epilepsy didn't appeal to him, so the Colemans settled into this adjusted lifestyle until they learned about a newer, less invasive treatment option that's performed in an MRI suite. Called laser interstitial thermal therapy, LITT for short, it uses a beam of targeted heat to attack — and destroy — the portion of a patient's brain causing the seizures. His Michigan Medicine neurologist, Nusha Mihaylova, M.D., Ph.D., told him laser ablation allows the surgeon to remove a seizure focus with pinpoint accuracy. Preserving his memory, IQ and other brain functions so Coleman would still be able to work was essential.
"The cognitive outcomes after laser ablation are better compared to what we see with open brain surgery, because it's restricted to the surgical site," explains Mihaylova, an assistant professor of neurology at Michigan Medicine. LITT also requires less recovery time than a craniotomy, but may offer a slightly lower chance of stopping seizures completely. A traditional temporal lobectomy is still possible later if LITT isn't curative, which keeps patients' options open.
"Our goal with any surgery for epilepsy is the best chance of stopping the seizures without a patient noticing a difference in how their brain works," explains Coleman's Michigan Medicine neurosurgeon, Emily Levin, M.D.
A chance to stop the seizures
It had been a while since Coleman could drive, and he was still working from home. So Coleman and his wife decided to go for it, and see if LITT would stop his epilepsy and get him back to his lifestyle from before the seizures began.
"I thought, if the worst that could happen is the seizures are still there, I at least tried," Coleman says. "If it works, everything's great, if not, I haven't really lost anything."
Levin, an assistant professor of neurological surgery at Michigan Medicine, started planning his LITT procedure. Because all brains are different, so are all brain surgeries.
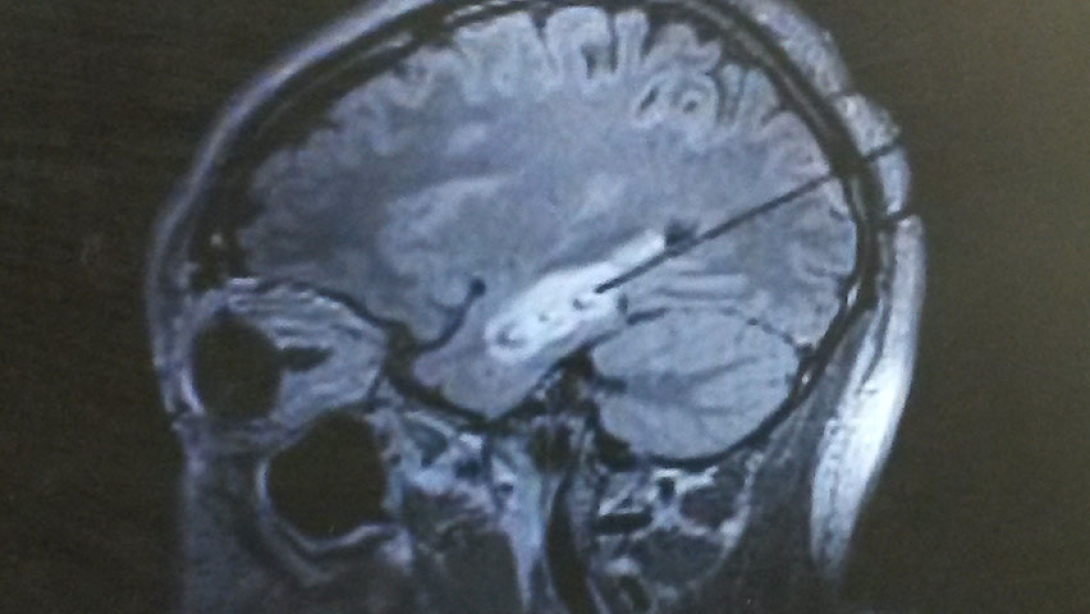
"Rob's seizures were coming from the left temporal lobe," Levin explains. "We also had to figure out where his speech and memory functions happen." She plotted a route to the source of the seizures that wouldn't damage those normal areas of Coleman's brain.
Coleman was asleep, getting MRIs throughout the day, while Levin operated on his brain for about an hour, only making an incision smaller than a quarter-inch. He was home the next day, resting for a couple of weeks, and back to work in his home office the next month.
Year One without a seizure
The epilepsy team tests patients after surgery to determine their risk for future seizures.
"The tests didn't indicate Rob was at risk for seizures anymore," Mihaylova says, "so we gradually started reducing his medications. We were able to stop one, and we are now tapering the second." Along with a lack of seizures, Mihaylova says Coleman's doing great in terms of cognitive function: concentration, paying attention, problem solving and other key tasks for a successful professional, and a husband and parent, in the prime of his life.
Coleman is also excited about another experience epilepsy stole from him: rush hour. Although he's enjoyed having a one-flight-of-stairs commute, Coleman's already driving again and says he's eager to get back to his company office for more face time with his colleagues of 23 years. His last neurology appointment is in February.

Explore a variety of healthcare news & stories by visiting the Health Lab home page for more articles.

Department of Communication at Michigan Medicine
Want top health & research news weekly? Sign up for Health Lab’s newsletters today!