Headache and migraines commonly affect pregnant women, often during the first trimester. An expert shares treatments to try and when to call your doctor.
7:00 AM
Author |

Pregnancy is a crucial time of life — a time when the expectant mother wants to make sure that she is taking care of herself and that everything is going well.
SEE ALSO: 3 Reasons Women Are More Likely to Have Insomnia
Unfortunately, frequent or severe headaches can waylay these plans for many mothers-to-be. Here, neurologist and headache specialist Lauren A. Aymen, D.O., shares the medications, supplements, treatments and symptomatic red flags pregnant women should watch for.
Is it common for pregnant women to have headaches or migraines during pregnancy?
Aymen: Yes. Migraines are usually worse in the first trimester but can improve during the second and third trimester. Unfortunately, in 4 to 8 percent of women, migraines can worsen. Headache frequency typically returns back to the patient's pre-pregnancy baseline after delivery.
What's the reason for this?
Aymen: Pregnancy usually brings with it hormonal changes, stress, disrupted sleep, nausea and dehydration. And all of these conditions may worsen migraine in pregnancy.
What can be done for pregnant women who have migraines?
Aymen: You can't use most of the over-the-counter (OTC) medications during pregnancy — with the exception of Tylenol (acetaminophen). Magnesium and riboflavin are OTC supplements that are safe and can be effective as well.
Unfortunately, there are few prescription headache medications that are safe to use during pregnancy.
However, there are certain procedures that are safe during pregnancy that can aid in preventing and stopping migraines. For instance, we commonly use nerve blocks to reduce the frequency and severity of headaches. One example is an occipital nerve block, which is very effective at reducing the burden of pain during pregnancy.
SEE ALSO: The Best OTC Meds and Supplements to Treat Headache
There is also a new procedure called a sphenopalatine ganglion nerve block, which involves placing a small rubber tube approximately 4 centimeters (about 1 1/2 inches) into each nostril and delivering medication to the sphenopalatine ganglion, a branch of the facial nerve. This is very effective for patients with frontal or retro-orbital head pain and certain facial pain syndromes. One advantage to this procedure is there are no needles involved, so it's minimally invasive. In addition, the medication we use in both procedures acts locally and does not have systemic side effects.
If effective, these procedures can be repeated during pregnancy without any known risk to the baby.
Can a headache be a sign of something more serious?
Aymen: Yes. A headache with any of the following symptoms — if you're pregnant or not — could suggest something more serious.
The red flags include:
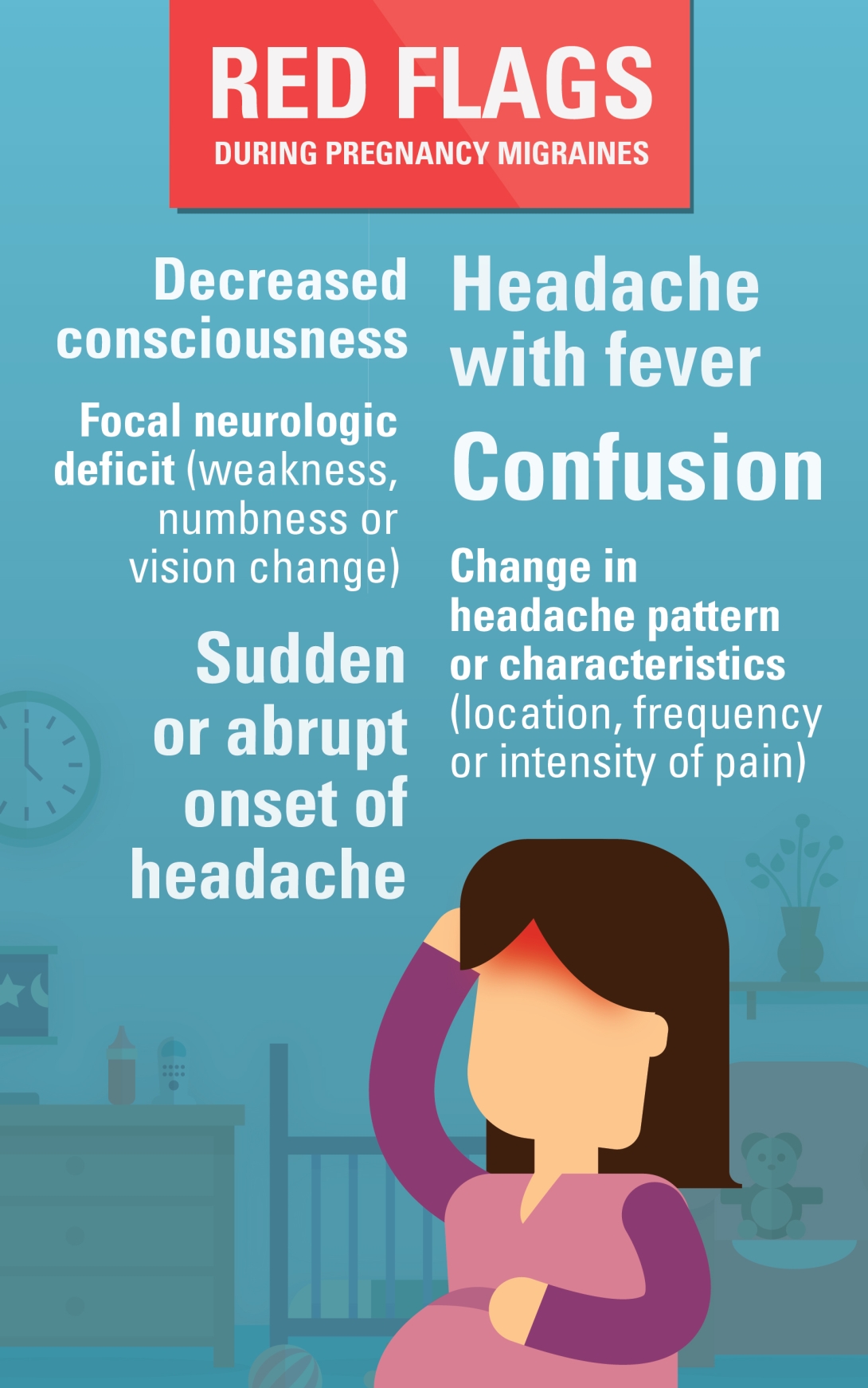
In addition, new headaches in people older than 50 could be a sign of a more concerning condition.
When should you contact your health care provider?
Aymen: If any of these red flags are present or if headaches are not responding to OTC medications or supplements, you should see a medical professional.

Explore a variety of healthcare news & stories by visiting the Health Lab home page for more articles.

Department of Communication at Michigan Medicine
Want top health & research news weekly? Sign up for Health Lab’s newsletters today!





