The fear of catching COVID-19 delayed a patient from seeking emergency treatment for a broken ankle. But thanks to a newly opened specialty care clinic, he’ll be riding the trails again soon.
2:45 PM
Author |
Editor's note: Information on the COVID-19 crisis is constantly changing. For the latest numbers and updates, keep checking the CDC's website. For the most up-to-date information from Michigan Medicine, visit the hospital's Coronavirus (COVID-19) webpage.
Interested in a COVID-19 clinical trial? Health research is critical to ending the COVID-19 pandemic. Our researchers are hard at work to find vaccines and other ways to potentially prevent and treat the disease and need your help. Sign up to be considered for a clinical trial at Michigan Medicine.
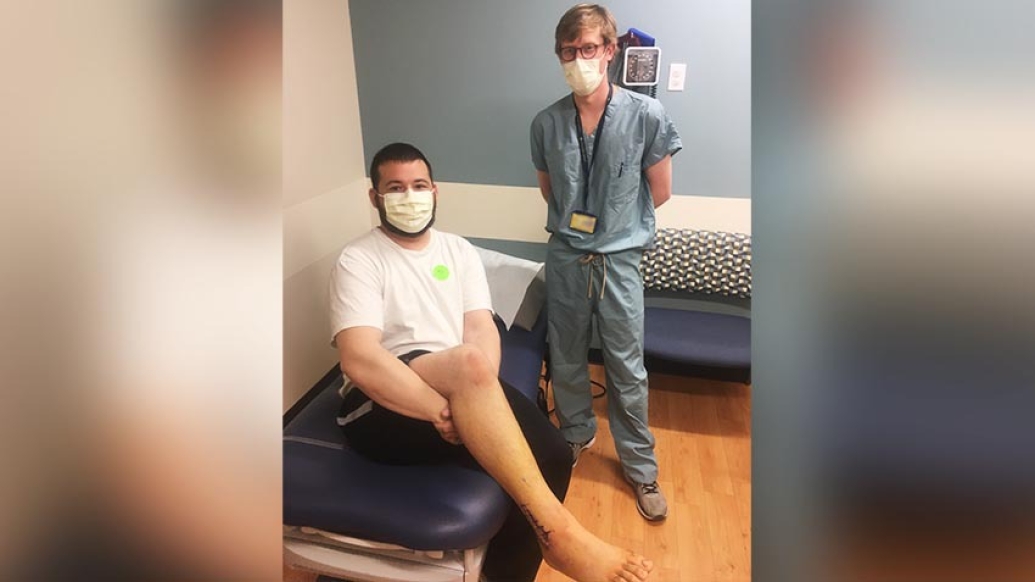
Evan Anderson was more afraid of being infected with the COVID-19 virus than he was of the broken ankle that he had hobbled around on for nine days.
The 32-year-old Plymouth, Michigan resident purposely avoided any emergency department after his right foot slipped off the peg and went under the moving back tire while riding an all-terrain vehicle (ATV) March 22 at Bundy Hill Offroad Recreation in Jerome, Michigan.
"Everything turned, popped and cracked, but I thought maybe it was just a bad ankle sprain," says Anderson, a married father of two children who owns Anderson Refrigeration LLC, a commercial refrigeration business.
Although it was Anderson's first ATV injury, such accidents keep emergency departments busy. In 2018, there were an estimated 81,800 ATV-related emergency department-treated injuries in the United States, according to a February 2020 report by the Consumer Product Safety Commission.
Anderson was able to push his ATV up a hill and drive home using that right foot thanks to supportive riding boots. For a week, he iced and elevated his ankle, using Motrin for the pain. When it didn't get any better after six days, Anderson found an urgent care in Livonia which wasn't seeing any COVID-19 patients, so he felt safe enough to go in for an X-ray.
"As soon as they saw the break, they wouldn't touch it and told me I needed an orthopaedic surgeon right away," he says.
Coming to Anderson's rescue
Getting help quickly was critical at this point, Anderson would later learn from orthopaedic surgeon James Holmes, M.D., an associate chief clinical officer at Michigan Medicine and a developer of the University of Michigan Comprehensive Musculoskeletal Center. Some broken bones that are not treated within a few weeks may not heal properly.
When Anderson called Michigan Medicine's Northville Health Center, they referred him to its new Bone and Joint Acute Injury Clinic at the Brighton Center for Specialty Care, where he met Holmes.
MORE FROM MICHIGAN: Sign up for our weekly newsletter
The bone and joint clinic opened March 30 as a way for patients with musculoskeletal injuries to limit their exposure to contagious patients at emergency departments during the pandemic, but still receive the full care they need. The clinic accepts patients with:
- Acute injuries of the foot, ankle, hand, wrist, knee, shoulder and elbow
- Closed simple fractures of the arm, elbow, hand, wrist, leg, foot or ankle
- Sprains and strains to the ligaments, muscles and tendons
- Acute back and neck pain
"We saw a need to see patients who would benefit from our care and whose care we could deliver fairly succinctly, accurately and expeditiously that didn't need to go into the hospital," Holmes explains. After deciding to open the clinic, it took three days and a team from nearly every department to launch it.
I wouldn't have normally put off getting treatment for so long but COVID changed all that. It's been an adventure.Evan Anderson
Comprehensive care during a pandemic
Anderson got one of the first appointments. He was screened for COVID-19 symptoms on the way into the building, giving him a sense of comfort about his initial fears of seeking care.
At the Bone and Joint Acute Injury Clinic, he had access to the same personnel he would have seen in the Michigan Medicine emergency department. The clinic is staffed by orthopaedic surgeons, physicians, musculoskeletal nursing and physician assistants, physical medicine and rehabilitation specialists, anesthesiologists and radiology specialists, with access to an outpatient surgery center and musculoskeletal imaging.
Holmes immediately bonded with him.
"Mr. Anderson understandably and appropriately waited nine days hoping he could walk his ankle fracture off rather than go to a hospital, and I'm sure I would have done the same thing," during the COVID-19 crisis, Holmes says.
Holmes operated on Anderson's distal fibula, repairing the ankle injury with a plate and screws. The outpatient procedure lasted just over an hour, Holmes reports.
Anderson, who is now in a cast, was happy with his care and his prognosis is excellent.
"I actually thought it was a really good experience," he says. "I feel like everything went pretty smooth. They were pretty quick to get me out of there." He arrived at 6 a.m. and was home by 11 a.m. He reports it was his best experience with anesthesia that he's ever had.
"I wouldn't have normally put off getting treatment for so long, but COVID-19 changed all that," Anderson says. "It's been an adventure."

Explore a variety of healthcare news & stories by visiting the Health Lab home page for more articles.

Department of Communication at Michigan Medicine
Want top health & research news weekly? Sign up for Health Lab’s newsletters today!





