The coronavirus felt like a distant threat, until an entire family experienced it firsthand.
5:00 AM
Author |
This article is part of a series marking one year since the COVID-19 pandemic began. Read more articles on the coronavirus from the Michigan Health and Michigan Health Lab blogs.
Fred Godfrey thought the COVID-19 pandemic was "hogwash", as he put it.
"I didn't think I needed the stupid mask and that I knew better than the experts. I wasn't worried about it; I wasn't really taking the precautions they say to take," he remembers.
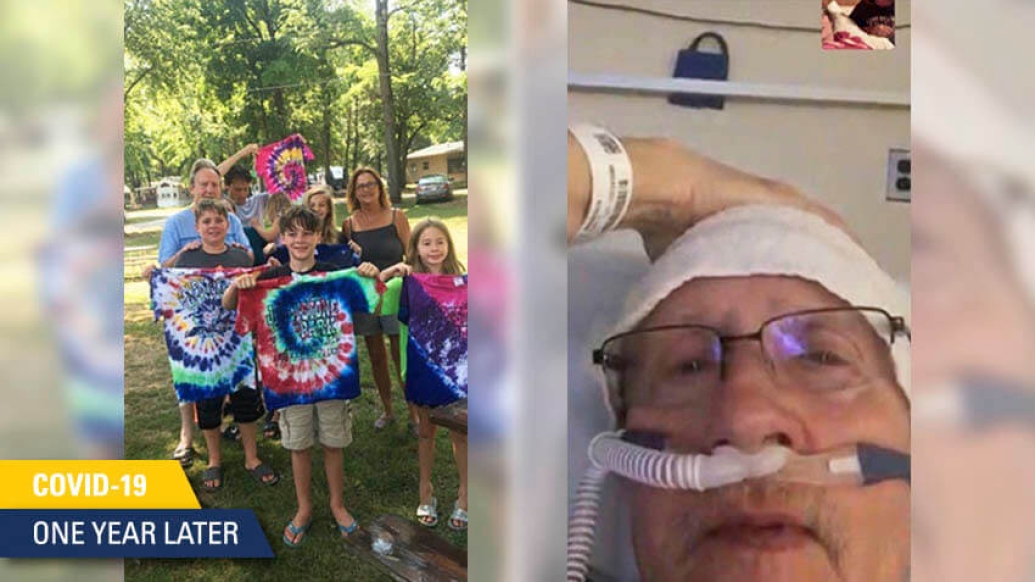
That was until he and his entire family – including his wife, two of his three kids, six grandchildren, and his son-in-law's aunt – fell ill with the virus.
How it began
On November 15, Godfrey, who is 69, and his grandson went to the local "buck pole", a gathering spot for hunters, for Michigan's opening hunting day. Godfrey recalls people from five to six counties being in attendance.
SEE ALSO: Keeping Our Patients Safe During COVID-19
"That's where I'm sure I got it," says Godfrey. "We didn't have masks on; I'm positive I picked it up there."
Over the next few days, Godfrey developed a "tickle" in his throat and a slight cough. He assumed it was allergies from his daughter's new dog, but as the days went on, Godfrey's coughing was incessant. He decided to get tested for COVID-19.
He was positive.
"I had it and I was taking everything that you read to take – drinking tonic water with quinine, taking zinc pills and quercetin supplements," he recalls.
Godfrey was sure he had everything under control, until the evening of December 3.
"Our water heater pilot light went out and I went to go light it. As I'm down on my hands and knees trying to light it, I started coughing so hard I couldn't get up. It hit that quick," recalls Godfrey. "I crawled out of the basement and up the cellar steps. I sat down in a rocking chair, and after about an hour I could start breathing a little, so I made it to my bed."
But when he got up the next morning, his oxygen level was at 83% on an oximeter the family owned – far lower than normal.
He and his wife, Betty, decided to head to their daughter's house, but on the way over, his oxygen levels dropped to 66%.
That's when his wife and daughter quickly re-routed him to Michigan Medicine's emergency room.
Godfrey was initially brought up to the general COVID-19 care unit, but then as a precaution the team transferred him to the intensive care unit in case he needed to be intubated.
A few days into his hospital stay, though, Godfrey felt as if he was losing his will to fight.
"I felt like I was going to die; I had given up," he says. "I was just completely exhausted."
Around this time, Godfrey found out the virus had spread through his family's "pod", leaving 12 of his family members with COVID-19. Fortunately, no additional hospitalizations were needed.
New friends like old friends
Although he wasn't able to have any visitors, he says FaceTime video chat sessions with his family kept his spirits high. So did visits with his care team.
MORE FROM MICHIGAN: Sign up for our weekly newsletter
"The doctors, nurses, they were like old friends that you knew for a long time," he explains with emotion showing through in his voice.
His doctor, Vineet Chopra M.D., M.Sc., chief of hospital medicine at Michigan Medicine, kept using the analogy of "getting to shore."
Godfrey recalls, "He said 'I can keep you from drowning, but I can't get you to shore yet.' Or he'd say 'We're a little closer to shore now.'"
These words of encouragement continued to give Godfrey hope. He remembers feeling very safe and cared for.
"I looked forward to every morning having him peek into my bed, waking me up. That was a really great thing, hearing him call my name and seeing him there."
Chopra never hesitated to speak with anyone from Godfrey's family on FaceTime or by phone to update them on his care, which they greatly appreciated.
"All my needs were met, and they thought ahead and had answers for questions for me before I even thought of them," Godfrey reflects.
His story is a reminder of the importance of respecting this virus and public health guidance. In this case, the best story is no story.Vineet Inder Chopra MBBS
An emotional recovery
Twelve days later after arriving at the emergency room, Godfrey was discharged from Michigan Medicine.
It was a day full of emotion, recalls Godfrey.
Like Podcasts? Add the Michigan Medicine News Break on iTunes or anywhere you listen to podcasts.
"You're on oxygen, you're still kind of struggling for air. In one way you're scared to leave, and another you're so happy to get home."
For the next month he and his wife stayed at their daughter's house in Saline, Michigan, so they were close to Michigan Medicine in case his situation changed.
Chopra's own research has shown that many hospitalized COVID-19 patients suffer setbacks and continued health problems in the first months after they leave the hospital. The study, based on data from the first wave of patients treated in hospitals across Michigan in spring 2020, was published just days before Godfrey went home.
For his arrival back home, Godfrey's wife, who's also a nurse, got the place properly set up with an oxygen tank, a shower chair and a walker. She scheduled a visiting nurse and physical therapy visits.
"I have a lot of medical people in my family, but someone who didn't know nothing would be scared," Godfrey says.
Although Godfrey recovered well, he says the cold air now bothers his lungs and that his stamina isn't the same as before.
"I still run out of air and I need to recoup for a minute or two," he explains.
A new attitude towards COVID-19
Since Godfrey's hospitalization, and his entire family's experience with COVID-19, he says they all wear masks, wash their hands "100 times a day" and don't go out much since it all happened.
"I wish cases like Mr. Godfrey were uncommon. Sadly, they are not," explains Chopra. "We saw COVID rip through families time and time again. And while I'm grateful that he and his family did well in the end - his story is a reminder of the importance of respecting this virus and public health guidance. In this case, the best story is no story."
"It's made us much more respectful of it," says Godfrey.
For others, Godfrey cautions taking the diagnosis lightly and seeking help as quickly as possible.
"You could never imagine how fast it comes on," he says – nor how quickly it can spread to your loved ones.

Explore a variety of healthcare news & stories by visiting the Health Lab home page for more articles.

Department of Communication at Michigan Medicine
Want top health & research news weekly? Sign up for Health Lab’s newsletters today!