A diving accident took away much of Kanon McVicker’s independence, but complex nerve and tendon transfer procedures are helping him meet important milestones.
5:00 AM
Author |
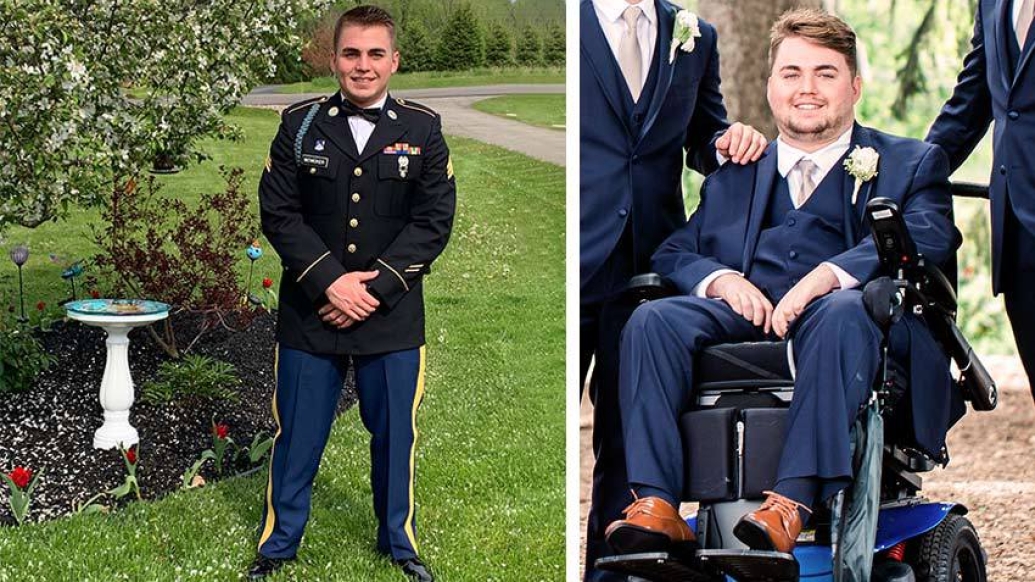
Kanon McVicker is thankful for small things in life, like brushing his teeth or holding a cup — even scratching an itch.
It's been a long, hard road for the 28-year-old whose life was drastically changed in 2019 when a diving accident resulted in a break in his cervical vertebrae, paralyzing him from the neck down.
Although doctors initially said he would not recover the use of his legs or arms, he's never given up hope that somehow he would prove them wrong.
And he's is doing just that, slowly but surely, thanks to innovative nerve and tendon transfer reconstruction expertise at University of Michigan Health.
"Following spinal surgery, my doctors told me basically I'd be paralyzed from the neck down and that would just be it," said McVicker.
But after a two-month stay at a rehabilitation hospital in Grand Rapids, Michigan, the young man began to feel slight movement in his arms.
It was the motivation the Eaton Rapids, Michigan, resident needed to pursue physical and occupational therapy, where he continued to see ever so small improvements in his arms and hands.
A promising discovery
It was also the motivation McVicker needed to begin researching possible treatment options for his condition. Months after his accident, he came across information about a spinal cord injury study headed by Wilson Z. Ray, M.D., and the promising possibilities it offered. An added bonus was that University of Michigan Health was involved in the study, with neurologist Lynda Yang, M.D., Ph.D., a foremost expert in spinal cord injuries, serving as one of its co-investigators.
Yang, director of the U-M Health Department of Neurosurgery's Brachial Plexus and Peripheral Nerve Program, met with the team of specialists, including Kevin Chung, M.D., director of the Comprehensive Hand Center, and Gianna Rodriguez, M.D., director of the U-M Health Spinal Cord Rehabilitation Program. Together, they evaluated McVicker in October 2020 to determine if he might be a candidate for tendon and/or nerve transfer procedures to improve the function of his hands and arms.
For patients with spinal cord injuries who want to improve hand and arm function, tendon and nerve transfers are the most promising surgical options, says Yang.
Tendon transfer is a procedure intended to restore function by transferring muscles/tendons that still work to augment muscles that are nonfunctional due to paralysis. Functional results are expected within weeks to months of the procedure.
Nerve transfer is intended to reactivate the muscle. During the procedure a branch or portion of a nerve in the arm above the level of the spinal cord injury is transferred to a nonfunctioning nerve from an area below the injury. By transferring the nerve, the recipient nerve can then receive the messages/signals from the brain to fire the muscles in the arms, hands and fingers. Functional results of a nerve transfer are expected within one to three years of the procedure.
The advantages of each technique differ, says Yang, noting that tendon transfer restores function earlier with likely more power, while nerve transfer results in function after a longer period, but likely restores more natural movement and finer motor control in the hand.
U-M Health is the only center in the U.S to offer both tendon and nerve transfer procedures, working with physical medicine & rehabilitation and physical/occupational therapy via a single interdisciplinary clinic through the Brachial Plexus and Peripheral Nerve Program. The program's collaborative team includes experienced physical and occupational therapists, physical medicine & rehabilitation spinal cord injury specialists, hand surgeons, neurologists and neurosurgeons working together.
"Each of our specialists evaluates the patient simultaneously in one clinic visit, then recommends nerve and/or tendon reconstruction, as appropriate," said Yang. "Together, our team discusses a customized plan, with patients benefitting from our interdisciplinary approach.
"Dr. Chung's expertise is complementary to my neurosurgery expertise and absolutely necessary for determination of every customized treatment plan," said Yang. "Without our distinct areas of expertise, we would not have the complete menu of options to offer patients deemed appropriate for surgical reconstruction, in coordination with Dr. Rodriguez and the rest of our team."
Meeting the qualifications
Despite the program's success, Yang points out that tendon transfer surgery and nerve transfer surgery are not cures.
"For this reason, first and foremost, we assess each patient's expectations. Some patients come to us wanting us to fix their hand, but this is not a fix or a cure. In Kanon's case, we felt his expectations could be met. He wanted to be independent in his wheelchair and to be able to feed himself."
I feel like I could teach others how to manage their expectations – and still give them hope.Kanon McVicker
Patients who qualify also need to have recovered as much function as possible from the spinal cord injury, says Yang.
And, finally, "Because there are no guarantees, there needs to be complete trust in the patient/physician relationship," Yang added.
McVicker was deemed a candidate for both procedures – and never hesitated to proceed with surgery.
"With Dr. Yang and Dr. Chung, it was my first experience with someone looking at my situation and being pretty optimistic about it," said McVicker. "They did limit my expectations and gave me the worst case scenario, which was that I might not get any better. There wasn't a lot of downward risk – only an upside.
"I was all on board. The doctors were passionate and super knowledgeable about what they were doing and so we went ahead with the first surgery in December 2020," McVicker said.
"Kanon underwent a coordinated nerve transfer and musculoskeletal (tendon) procedure in December 2020 to improve the function of his left arm," said Yang.
So far so good, says McVicker.
"After recovering from the surgery, it's like I've never had a month where I've plateaued. I've been getting incrementally stronger and more mobile. I've had Increases in strength and range of motion in my arm and hand – and in my independence for sure. I've had a definite improvement in my quality of life."
His mother and primary caregiver, Amy, agrees. "Before the surgery he could barely lift his arm and now he can lift his left arm over his head, and even reach out and hit us when we walk by. It's like night and day – and beyond what I expected."
A second time around
When asked if McVicker would be interested in having surgery on his right arm more than a year later, again, he didn't hesitate.
"I said absolutely."
"Kanon underwent a similarly coordinated nerve transfer and tendon procedure in April 2022 to improve the function of his right arm," said Yang. "Now, we're waiting to see how he responds to the second surgery."
McVicker says his right arm is definitely getting stronger.
"Before the April surgery my right arm had no tricep strength, but after the cast came off, I've noticed a little bit of strength and it's just continuing to get stronger."
Rehab's critical role
Critical to McVicker's progress is his ongoing rehabilitation and quality of care, says Yang, who noted: "The surgery is just a start."
Currently attending a rehab facility close to his home, McVicker's physical and occupational therapy plan is directed by U-M Health rehabilitation specialists who work hand in hand with the facility.
"We direct the plan and Recovery Project executes it," said Rodriguez. "We collaborate and share our knowledge with the team to ensure the highest quality of care. We want to make it convenient for patients without sacrificing quality.
"We see good outcomes with patients who are motivated and enthusiastic," continued Rodriguez. "Patients also have to want to self-manage, based on the education and direction we provide. At the end of the day they are ultimately responsible for themselves."
Kanon is one of those patients.
"He is very compliant and motivated – that's what keeps him progressing," said Rodriguez. "He and his family also realized he would likely not be able to move further without the surgeries. Now, with ongoing rehab, there's no telling how far he can go."
McVicker says his rehab team is noticing the improvements he's making with physical and occupational therapy twice a week.
"They do evaluations once a month to see my progress. There's never been an evaluation where I haven't improved just a little bit."
Looking toward the future
A criminal justice and psychology graduate, McVicker had just been promoted to Sergeant with the Army National Guard when his accident happened. Undeterred, he's now planning to pursue his master's degree in psychology in the spring.
"I feel like I want to specialize in helping people with similar injuries," he said. "I feel like I could teach others how to manage their expectations – and still give them hope. It's incremental work – you don't always have to stay positive. I have bad days but overall I try to be positive about my situation.
"If anything helps just a little bit, that's infinitely better than nothing. Just me being able to move one arm a little better than before enabled me to move my chair on my own and be independent. I can brush my teeth now with some adaptive equipment. That not only helps me as far as my well-being but it also helps the people taking care of me."
His mother couldn't agree more.
"Every small improvement is still an improvement. It's progress and we're happy with that even though it might be a little bit at a time."
McVicker is equally realistic.
"I wasn't expecting to wake up from the surgery and be doing pushups, but it's been incremental. It definitely takes a lot of dedication and positive mindset. If you don't' see results right away, don't get discouraged. It might take years to get to the maximum improvement — and I don't even know what the maximum is yet because it's getting better and better incrementally.
"I've definitely been more encouraged since the surgeries," McVicker said. "And things are getting more and more advanced, so maybe one day we'll have a complete cure for spinal cord injuries – but you have to start somewhere."
Live your healthiest life: Get tips from top experts weekly. Subscribe to the Michigan Health blog newsletter
Headlines from the frontlines: The power of scientific discovery harnessed and delivered to your inbox every week. Subscribe to the Michigan Health Lab blog newsletter
Like Podcasts? Add the Michigan Medicine News Break on Spotify, Apple Podcasts or anywhere you listen to podcasts.

Explore a variety of healthcare news & stories by visiting the Health Lab home page for more articles.

Department of Communication at Michigan Medicine
Want top health & research news weekly? Sign up for Health Lab’s newsletters today!





