After a near-death health scare, renewed strength and hope comes thanks to a U-M cardiovascular care team and a committed advocate.
7:00 AM
Author |

An avid golfer, sailor and professional photographer, Nora Fisher, pictured above with her sister, plans to resume her active lifestyle soon.
MORE FROM MICHIGAN: Subscribe to our weekly newsletter
For now, however, rest and recovery are on the agenda after a transcatheter aortic valve replacement (TAVR) procedure in September that the 70-year-old credits for saving her life.
Until a year and a half ago, the energetic Fisher was making the most of retirement after a 33-year career teaching high school.
But when an abdominal hernia began interfering with her activities, Fisher decided it was time to have it surgically repaired — a seemingly simple step. Instead, the procedure started a chain reaction of sickness she couldn't manage alone.
Unexpected trouble
Fisher, a resident of Flint, Michigan, didn't count on the series of events that followed her hernia repair surgery June 5, 2015.
She developed several infections that led to additional surgeries over the next year — as well as a severe bacterial infection known as infective endocarditis that would take her to the brink of death.
Infective endocarditis is an infection caused by bacteria that enter the bloodstream and settles in the heart lining or heart valve. In Fisher's case, the severity led to a damaged aortic valve that needed to be replaced.
Before that could happen, though, she would need to heal from her abdominal issues.
Extremely ill and unable to make medical decisions on her own, Fisher turned to her sister, Lynn Levin, for help.
Levin's first decision: to have her sister transferred to the University of Michigan Health System, where more abdominal surgery to repair Fisher's intestine was performed by U-M gastroenterologist John Byrn, M.D.
"I needed to get well enough to have my aortic valve repaired," Fisher recalls.
Choosing TAVR
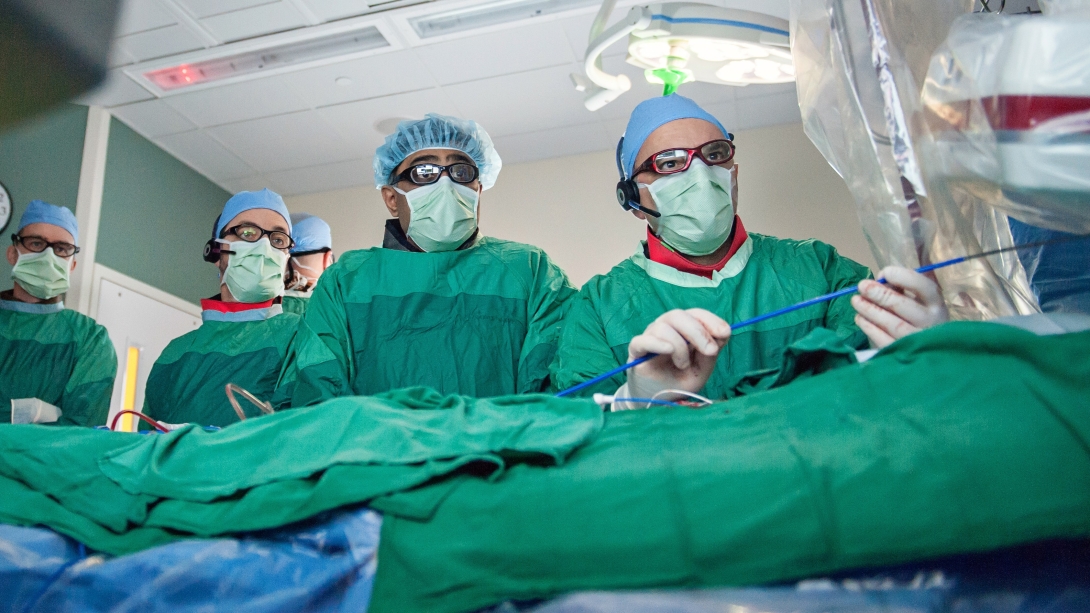
Once Fisher was stabilized, doctors at the U-M Frankel Cardiovascular Center performed several procedures, including a transesophageal echocardiogram, to identify the exact condition of the patient's aortic valve to establish a treatment plan.
Doctors determined that Fisher was too ill to tolerate and recover from traditional surgical aortic valve replacement (SAVR) but was a candidate for TAVR. The procedure, led by U-M cardiologists P. Michael Grossman, M.D., Stanley Chetcuti, M.D., and G. Michael Deeb, M.D., was performed in September 2016.
"When we met Ms. Fisher, she was extremely ill," says Grossman. "Her heart was failing due to the ravages of her aortic valve condition. After a thorough evaluation, the U-M Heart Valve Team felt that TAVR was the only valve replacement option for Ms. Fisher."
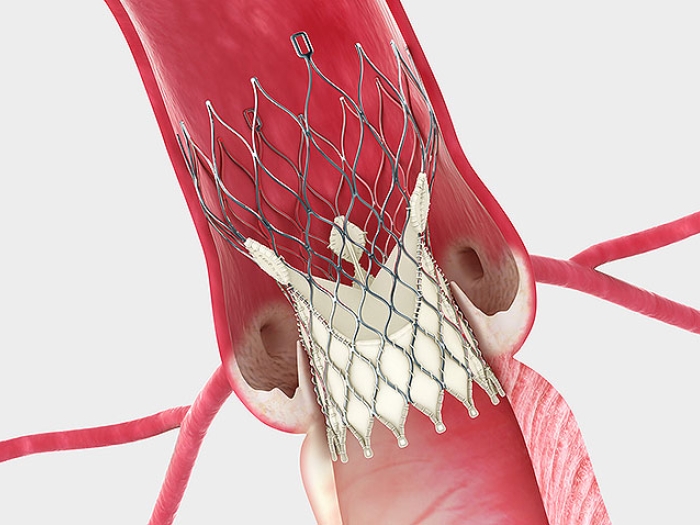
Unlike a SAVR procedure, which involves opening the chest to replace a patient's aortic valve, the minimally invasive TAVR can be done through small incisions that enable a new valve to be inserted by means of a catheter.
Which is why TAVR patients often experience a much quicker recovery than SAVR patients that allows most of them to begin cardiac rehabilitation within days or weeks, typically resulting in dramatic improvements in quality of life.
U-M has performed more than 780 TAVR procedures — the most of any health system in the state — and is one of the top programs in the country in terms of TAVR volume.
Advocacy and gratitude
For Fisher, the results of the procedure were evident almost immediately.
SEE ALSO: TAVR Procedure Performed on a Teen, a Rarity
"I could finally breathe without oxygen," she says.
Adds Grossman: "The minute we deployed the new valve, Ms. Fisher's blood pressure and heart-pumping function improved — and the smile on her face when we saw her the morning after the TAVR confirmed a wonderful result."
Currently in cardiac rehab, Fisher is grateful for the "fabulous care" she received at U-M.
She's also deeply grateful for the advocacy and commitment of her sister.
Levin, often faced with making difficult health care decisions on behalf of Fisher, remained by her side during 18 months of on-and-off hospitalizations and rehabilitation programs.
Given her experience as a dedicated patient advocate, Levin urges people in similar situations to do plenty of research on a loved one's medical condition and ask lots of questions.
At one point, the U-M Palliative Care team counseled her about life-and-death decisions she would likely face.
"But I believed in miracles," Levin says.

Explore a variety of healthcare news & stories by visiting the Health Lab home page for more articles.

Department of Communication at Michigan Medicine
Want top health & research news weekly? Sign up for Health Lab’s newsletters today!