An outbreak of a pox virus, not typically found in Europe and North America, has many on alert.
8:34 AM
Author |
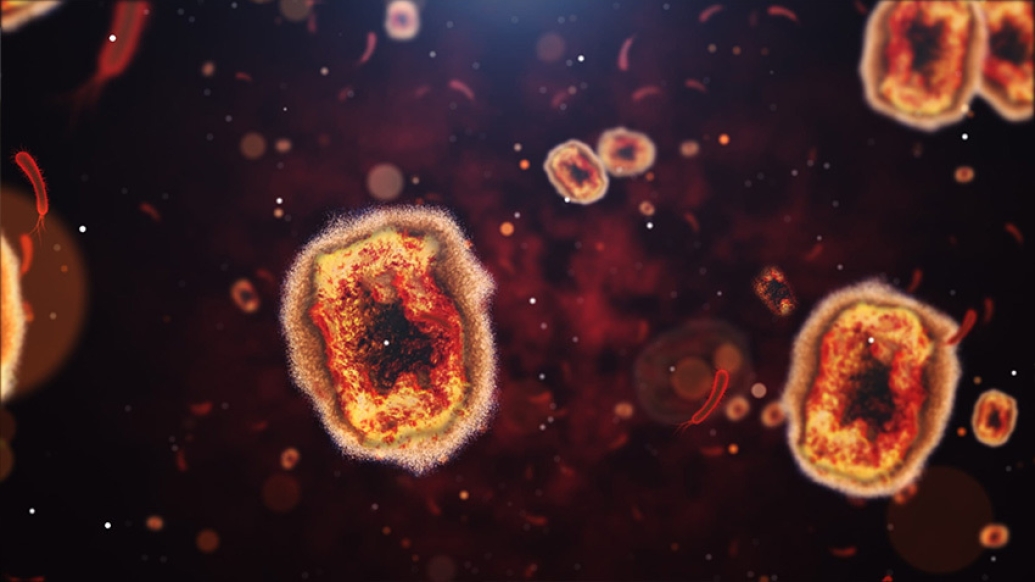
Infectious disease and public health specialists have raised an alarm as cases of monkeypox have spread throughout Europe and the United States. Monkeypox is a member of the orthopox family of viruses, related to smallpox virus, which was eradicated through vaccination in 1980.
Here, infectious disease specialist Sandro Cinti, M.D. answers some basic questions about monkeypox and how to protect yourself.
How does monkeypox spread?
Cinti: Monkeypox does not spread like flu or COVID, it spreads via close personal contact, including during sexual encounters. At the moment, it's been spreading mostly among men who have sex with men, but it can also be transmitted among family members who are in close contact, though not very efficiently.
This is not an extremely transmissible disease; nowhere near the level of COVID or influenza. Contact usually requires more than three hours of exposure within six feet and usually direct contact with lesions rather than respiratory droplets. It can also spread via contaminated linen and clothing.
The World Health Organization is currently saying this does not constitute a global public health emergency and has not widely spread within the community. If there begin to be more cases spreading in a way that is different, including droplet transmission, I think the WHO might revisit it as an emergency.
How would you recognize if you had monkeypox?
Cinti: The lesions are not subtle and are bigger than chickenpox (see link to Centers for Disease Control and Prevention for images). They can be on the face, hands and the trunk (abdomen). For the first time, we are seeing them sexually transmitted and so lesions can be on the genital or peri-anal area also. People who have these lesions should avoid sexual contact.
People can also experience fevers, chills and lymph node swelling. Sometimes that occurs before the rash appears. However, in this outbreak, those symptoms have been less frequent.
Like Podcasts? Add the Michigan Medicine News Break on Spotify, Apple Podcasts or anywhere you listen to podcasts.
Some clinicians may not recognize the lesions, which can sometimes look like a pimple, skin ulcer or papule, sometimes with a divot in the center. Any unusual skin lesions should be investigated.
How widespread is this current outbreak?
Cinti: This outbreak is so far relatively small at more than 7,594 cases worldwide and more than 700 cases in the U.S. It is notable because it is transmitting outside of West Africa where it is endemic and is spreading among people in other countries in people with no contact with West Africa.
What is the best way to protect yourself from monkeypox?
Cinti: Have protected sexual contact and avoid touching someone with skin lesions. If someone has been infected, they should contact their public health department to determine how to reduce the risk of transmission.
A person with a monkeypox infection should wear a mask and avoid close contact with others until the skin lesions are completely healed, which can take up to two weeks. It is a long course for people who get infected. I do want to stress that the risk to the public is very low. Most of the cases have been transmitted through sexual contact.
If you have been exposed to monkeypox (a close family member or sexual partner) please contact your physician or public health.
Are there any treatments for monkeypox?
Cinti: There are antiviral therapies for people with severe cases. Monkeypox will resolve without any treatment. Very few people have been hospitalized and no one has died, which is good news, and there is a vaccine available, but most people won't qualify for it.
However, if someone has had a significant exposure there is a possibility of receiving the vaccine to prevent illness. Having said that, the general population does not need vaccination.
Live your healthiest life: Get tips from top experts weekly. Subscribe to the Michigan Health blog newsletter
Headlines from the frontlines: The power of scientific discovery harnessed and delivered to your inbox every week. Subscribe to the Michigan Health Lab blog newsletter

Explore a variety of healthcare news & stories by visiting the Health Lab home page for more articles.

Department of Communication at Michigan Medicine
Want top health & research news weekly? Sign up for Health Lab’s newsletters today!