An immunologist explains how the vaccine trains your immune system to fight the coronavirus.
7:55 PM
Author |
This article was updated on May 10, 2021.
The Pfizer and Moderna mRNA vaccines currently being rolled out to the public are considered an incredible scientific achievement. But, many might wonder, what exactly do they do?
Here to clear up that mystery, Beth Moore, Ph.D., the Interim Chair and Professor of Microbiology & Immunology at Michigan Medicine, breaks down what happens after the shot goes into your arm.
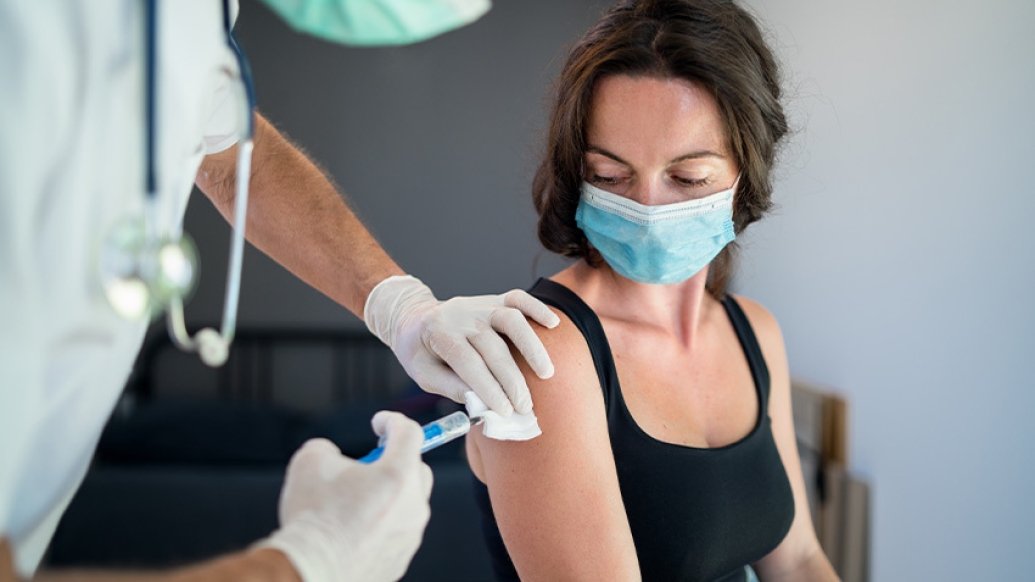
1 minute after COVID vaccination
Pick an arm and roll up your sleeve. After answering a few screening questions, the shot goes in.
Along with salt, sugar and a fat coating, the most important ingredient in the vaccine is the mRNA, a tiny instruction manual for your cells to use to make the infamous SARS-CoV-2 spike protein. Scientists figured out that the coronavirus uses its spike protein to attach to molecules called ACE2 receptors on the outside of your cells to get inside.
"Once inside the cell, the mRNA from the vaccine is taken up by your ribosomes and translated into many copies of the spike protein," says Moore. Then, the mRNA is broken down and the newly-formed spike protein is released from the cell.
MORE FROM MICHIGAN: Sign up for our weekly newsletter
15 minutes after
After their jab, most people will be asked to sit and wait a 15-minute observation period, to watch for rare allergic reactions. Those with a history of serious allergic reactions should prepare to wait up to 30 minutes. Reactions have ranged from hives to anaphylactic shock and are quickly treated with Benadryl for a mild reaction or epinephrine for anaphylaxis.
12 hours to 10 days later
Your arm might be a little sore or maybe you'll feel some fatigue after the first shot. What's happening?
Your immune system is gearing up, Moore explains. After your cells use the mRNA to develop the spike protein, immune messenger cells called dendritic cells come into play.
"Dendritic cells are patrolling and will come in contact with the antigen that they haven't seen before and raise the alarm, travel to a lymph node, find the right T and B cells and activate them," Moore says.
Fatigue and soreness, she explains, are the result of substances called cytokines and chemokines that help direct more immune cells to the infected site, causing inflammation. Some people report temporary swelling of the lymph nodes in their armpit after receiving the vaccine, as well.
Your immune system can't tell the difference between just a spike protein and the actual virus. "Feeling a bit run down is just a sign your immune system is working," Moore says. But if you don't feel tired or sore, don't worry. Not everyone feels these effects.
In April 2021, use of the Janssen/J&J COVID-19 vaccine was paused after six women—out of 6.8 million who received the one-shot vaccine--developed a rare clotting disorder. The condition is similar to a reaction some people have to an anti-clotting medication called heparin.
However, the CDC lifted the pause ten days later after meeting to discuss guidance for patients and healthcare providers.
"The bottom line is this is a very rare complication, but not clear yet what causes it. The benefits still outweigh risks, especially for people with no history of clotting disorders," says Moore. People who are concerned can consider opting for one of the mRNA vaccines, which are not linked to this clotting disorder.
3 to 4 weeks later
Both of the mRNA vaccines require two shots: three weeks later for the Pfizer vaccine and four weeks for Moderna. During that waiting period, "hopefully, your B cells are generating good plasma cells and making neutralizing antibodies," says Moore. Neutralizing antibodies block the coronavirus from entering your cells and making you sick. But these can be relatively short-lived. Hence the need for the second dose which can help generate longer-lived immune cells that can respond to the spike protein. Many people report a much stronger reaction to the second dose, including fever, fatigue and muscle aches.
"Because you already have antibodies on-board from the first dose, you're going to get a little bit more robust immune response the second time," Moore says. "At the same time, you are boosting the immune response to be bigger, better and faster and really locking in the memory of it."
Don't be tempted to avoid the second shot to avoid potentially feeling sick. The danger of not getting the second dose is you'd have short term protective antibodies from plasma cells, but no long term memory cells, explains Moore.
SEE ALSO: Seeking Medical Care During COVID-19
Meaning within time (and how time much has yet to be determined), you could have no protection.
In addition, these side effects are temporary—compared to the far more serious, and potentially deadly—effects of COVID-19.
6 weeks later
Remarkably, the current COVID-19 mRNA vaccines were 95% effective at preventing COVID-19 in clinical trials two weeks after the second dose. Moore believes that may be due in part to how targeted the vaccines are.
"With natural infection with the virus, the body may generate an immune response to multiple proteins on the outside and inside of the virus—but ones that aren't doing any good because they don't block the spike protein from ACE2." The mRNA vaccines only code for the correct protein. "That's one of the reasons why people who have already been infected with COVID-19 should get the vaccine. Even if you've survived the infection, you don't know if you have good neutralizing antibodies or a lot of irrelevant antibodies."
The future after receiving a COVID-19 vaccine
More vaccines are coming soon, using different technologies. The AstraZeneca and Janssen vaccines, both studied at Michigan Medicine, each use inactivated adenoviruses to deliver the gene for the spike protein to your cells. Says Moore, "Immunologically, they may have an advantage in that the more foreign material you give your body to respond, the bigger more robust response you get."
As the vaccines are rolled out to more and more people, studies are ongoing to see how long immunity will last, if people who are vaccinated can still spread the virus and whether the virus will mutate to the point where the vaccines are no longer effective.
To the last point, "all viruses mutate," says Moore. "The good news is the vaccine is still effective because the mutations haven't changed the basic structure of the spike protein so much that the neutralizing antibodies are not effective," she adds. But scientists will continue to monitor these variants to see if eventually the vaccines will need to be modified.
Like Podcasts? Add the Michigan Medicine News Break on iTunes, Google Podcast or anywhere you listen to podcasts.
As far as when we can take off our masks and gather together again, the verdict is still out.
"We know that if you make a neutralizing antibody against the spike protein, that means the virus can't attach to the ACE2 receptor on the cells in your body easily," Moore explains. "With a good neutralizing antibody response, the vaccinated person is unlikely to have a clinically significant (or even noticeable) infection, but it may still be possible for that person to breathe out the infectious live virus."
Until data come in from studies of vaccinated people, it's too big a risk to stop taking precautions.

Explore a variety of healthcare news & stories by visiting the Health Lab home page for more articles.

Department of Communication at Michigan Medicine
Want top health & research news weekly? Sign up for Health Lab’s newsletters today!





