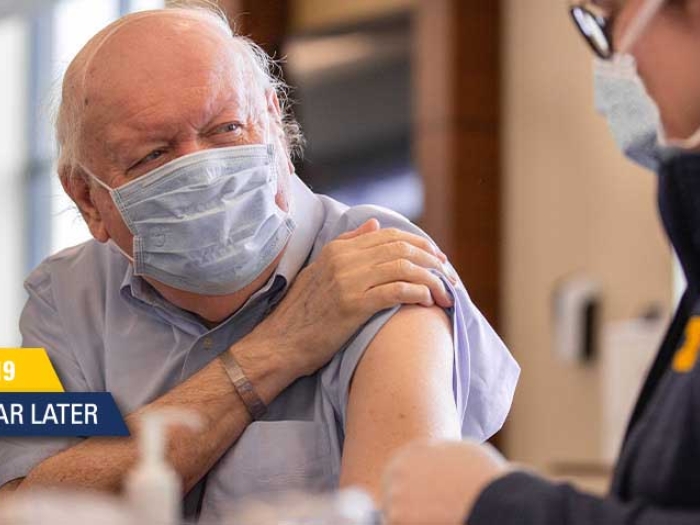
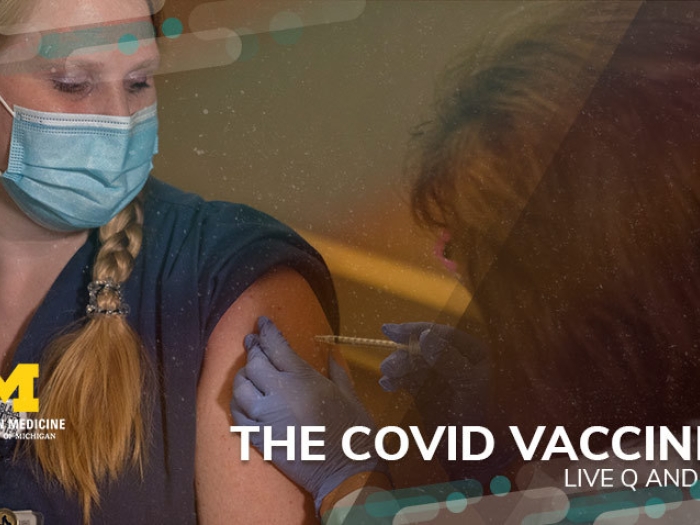
Why a false controversy about vaccine privacy and “passports” threatens to prolong the pandemic.
2:56 PM
Author |

Editor's note: Information on the COVID-19 crisis is constantly changing. For the latest numbers and updates, keep checking the CDC's website. For the most up-to-date information from Michigan Medicine, visit the hospital's Coronavirus (COVID-19) webpage.
What do kindergarteners, people taking exotic vacations, health care workers and Ellis Island immigrants have in common?
Most of them had to prove, in one form or another, that they wouldn't spread deadly infectious diseases to others.
Without that proof, they couldn't start school, get on a plane, work in a hospital or start a new life in America.
They're just a few examples of the long-established right for public institutions such as schools, employers, governments and businesses to protect the health of others by requiring individuals to provide proof of vaccination or of a past infection, or seek a medical or religious exception.
So why has COVID-19 vaccination become a lightning rod for controversy over "vaccine passports" and claims of violations of medical privacy or individual rights?
It's actually a tempest in a teapot, say two University of Michigan Medical School experts.
Rights vs. reality
Medical historian Howard Markel, M.D., Ph.D., has written two popular books on the history of infectious diseases and efforts to stop them over the centuries.
"Ways of proving vaccination or past disease have long existed in different forms, and for different diseases, even before we understood what actually caused infections or had vaccines against them," says Markel, who directs the University of Michigan's Center for the History of Medicine.
"They don't take your freedom away," he explains. "In fact, they increase your freedom because they allow you to travel where you want to go and do what you want to do. It's a non-issue and those who say otherwise are making controversy where none should exist."
SEE ALSO: Overcoming COVID-19 Vaccine Hesitancy
Health law and medical ethics researcher Kayte Spector-Bagdady, J.D., M.Be., meanwhile, notes that, "Institutions rarely have the right to require that you actually get vaccinated, but if you want to work somewhere in particular, or want others to provide you services (such as schools, or businesses, or travel), they might have the right to ask you to provide proof of vaccination first."
She adds, "Not only might they have the legal right, but they might also have the legal obligation to protect others." Spector-Bagdady is associate director of U-M's Center for Bioethics and Social Sciences in Medicine. She and Markel are both members of the U-M Institute for Healthcare Policy and Innovation.
The legacy of smallpox
The 1918 influenza pandemic has gotten a lot of attention for its similarity to the COVID-19 pandemic and the power of masking and reduced public gatherings to "flatten the curve" of cases. That's a phrase that Markel co-invented after studying the impact of preventive efforts in 1918 and 1919.
But for vaccination privacy, the history of smallpox is a better comparison, he says. That disease plagued humankind for thousands of years and killed one in three people who caught it, before worldwide vaccination eradicated it in the late 1970s.
No one is saying all Americans must get vaccinated against COVID-19, unlike the mandatory smallpox vaccination requirements of the early 20th century that made it possible for the entire United States to become free of outbreaks by the late 1940s.
The Supreme Court affirmed the right of health departments to require smallpox vaccination way back in 1905.
Other examples of "requiring proof" of vaccination
That ruling, and other judicial and legislative actions since then regarding the right to require proof of vaccination in certain circumstances, will all inform what governments, businesses, universities, school districts and others will do regarding COVID-19.
"You are free to make choices about vaccination, but all of our choices have consequences," he explains. "It simply means you won't be able to go places or do things that will require you to show you've been vaccinated. If you think that's freedom, have at it."
That's why parents carefully guard the small folded pieces of paper on which a doctor or nurse had written down the date and type of their young children's vaccinations, to show during school registration.
It's why vacationers, journalists, missionaries and nonprofit organization workers bound for many African countries have to carry a special certificate proving they've been vaccinated against yellow fever.
It's why many health care workers have to prove they've had multiple shots and get tuberculosis tests so they can avoid infecting their patients.
You are free to make choices about vaccination, but all of our choices have consequences. It simply means you won't be able to go places or do things that will require you to show you've been vaccinated. If you think that's freedom, have at it.Howard Markel, M.D., Ph.D.
And it's why the ancestors of today's Americans of European descent could be turned back if they didn't have a scar on their upper arm from a smallpox vaccination, or pockmarks showing they'd survived the disease. Even if they made it within sight of the Statue of Liberty, they could get sent home if they had symptoms of other diseases.
More recently, from the late 1980s until 2010, people with HIV/AIDS could not travel or immigrate into the United States – a ban based in both politics and public health concern.
Markel, who recently wrote about the history of the polio vaccine for the New Yorker magazine, remembers going to get his dose of vaccine as a child, at a mass-vaccination site that was a rite of passage for Baby Boomers and an important milestone to be allowed into school.
Exceptions to vaccine requirements
Entities that require proof of vaccination can also choose to allow unvaccinated people to do something in lieu of getting a vaccine.
For instance, health care workers who opt out of flu vaccination requirements might have to request a medical or religious exemption to do so, and wear a mask at work when influenza cases in the community are high.
And states can set conditions – such as mandatory education of parents about the dangers of disease and the safety of vaccines, or certification that they have a religious objection – before allowing unvaccinated children to attend school.
Markel notes that allowances for philosophical objections to vaccination, often fueled by false claims and fake science, have been on the rise since anti-vaccination activists began seeking legislative action in the 1980s.
SEE ALSO: Flattening the Curve for COVID-19: What Does It Mean and How Can You Help?
Spector-Bagdady says that one of the big questions still unresolved is whether the COVID-19 vaccine will be treated more like the annual flu vaccine or the measles vaccine. The flu shot is strongly encouraged for everyone by medical professionals, but only required in limited circumstances such as hospital workers. But the measles vaccine is required in many more situations, including enrollment into many public schools.
The federal government is expected to issue guidance for the use of COVID-19 vaccine status soon, but seems unlikely to set a standard for a national document beyond the white cards issued to vaccinated people. Other countries are creating their own standards and passes.
The misuse of HIPAA
One of the things that has been mentioned in both the vaccine controversy and in resistance to mask mandates is HIPAA. That's the acronym for a 1996 federal law that includes a medical privacy provision that went into effect in 2003.
HIPAA is one of the most misunderstood health laws in the country, says Spector-Bagdady, who has studied medical privacy extensively.
"Very few people actually understand what it means. They think it provides comprehensive privacy protections for health information in all circumstances, which it simply does not," she explains. "HIPAA only governs certain kinds of entities – your clinician, hospital, or others in the health care sphere. It does not apply to the average person or to a business outside health care. It doesn't give someone personal protection against ever having to disclose their health information."
So for example, if your friend shares on social media that she just got vaccinated against COVID-19, and you tell someone else that you had seen that post, you are not in violation of HIPAA because you're not covered by it in the first place. Your friend might like you less, but you're not breaking the law.
But if the nurse who gave your friend her shot took a picture of her and posted it on his own social media account without getting your friend's signed consent, that would be a HIPAA violation. However, nurses are trained in how to abide by the law, and they and their employers are subject to fines and public reporting if they violate HIPAA.
Another example Spector-Bagdady gives is hospitals that require patients get tested for COVID-19 before getting further services. If the patient doesn't have COVID-19 they can proceed. But if they do, and the treatment they're seeking isn't urgent, doctors might decide to postpone. If a patient refuses to get tested in the first place, they will likely be assumed to have it.
"We are allowed to put boundaries on access to non-urgent medical treatments in order to protect our team members, other patients, as well as the patient themselves who might suffer additional COVID-19 related complications," says Spector-Bagdady.
But HIPAA largely doesn't apply in the mask debate, she says. An individual cannot simply say that they have a HIPAA "right" to access a business or indoor space without wearing a mask.
"I have a visceral reaction when I read that in the news media," she adds. "That's really not a thing."
If there's a public health order in place in that state, county or city requiring mask use indoors, businesses not only have the right to require masks, they have a legal obligation, and could be fined for not doing so.
The bottom line, she says, is that, "unlike in clinical care – where adults with capacity almost always have the right to decline a medical intervention – under a public health framework we aren't allowed to put other people's lives at risk just because we think protecting other people is annoying. Just as with a criminal law prohibiting you from physically attacking another person; Oliver Wendell Holmes famously said 'The right to swing my fist ends where the other man's nose begins.'"
Moving forward
The past year has seen a pandemic turned into a political event in the U.S. and some other countries, Markel says.
The vaccine means the chance to turn the corner and get it behind us, but false controversy over it could slow that process and allow more contagious variants of the virus to evolve as it passes from person to person.
"Politics should end with the microbe," he says.

Explore a variety of healthcare news & stories by visiting the Health Lab home page for more articles.

Department of Communication at Michigan Medicine
Want top health & research news weekly? Sign up for Health Lab’s newsletters today!