Michigan Medicine specialists are combining new techniques to improve how they diagnose prostate cancer and deliver treatment to the right target.
7:00 AM
Author |
The goal is not to find every prostate cancer — it's to find aggressive prostate cancer that may affect a man's survival.
MORE FROM MICHIGAN: Sign up for our weekly newsletter
A convergence of more sophisticated imaging techniques and a better understanding of what makes prostate cancer aggressive is helping to better identify those cancers that are more likely to grow quickly and spread to other parts of the body.
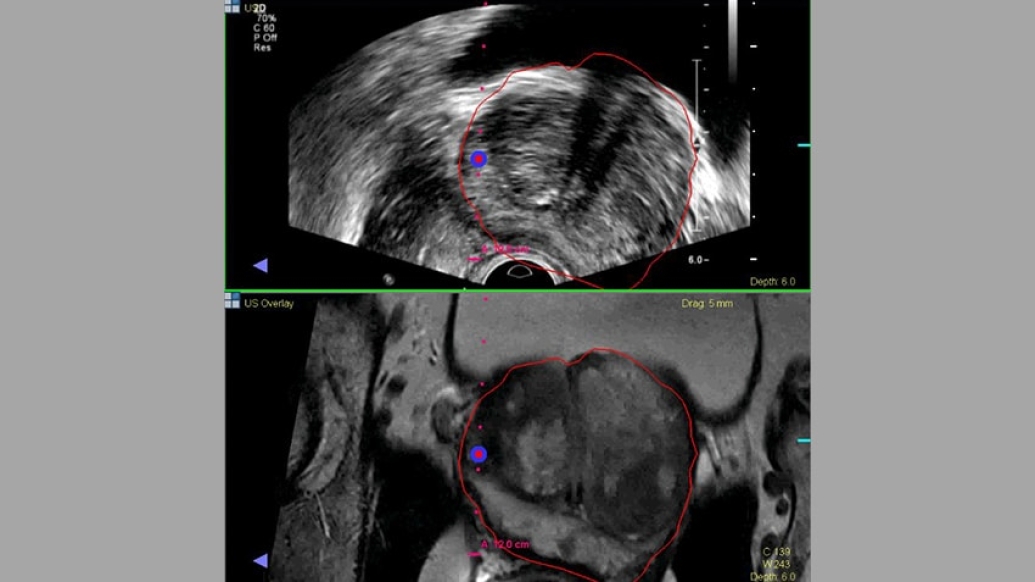
Michigan Medicine was first in the region to offer men a new technology called UroNav, which combines MRI and real-time ultrasound to help guide a biopsy needle, ensuring that tissue from all suspicious areas is captured. Since introducing UroNav in 2014, the prostate cancer team has done nearly 1,000 of these biopsies.
"Standard prostate biopsies are random. We systematically obtain random samplings from the prostate, but there's no guarantee that a biopsy will hit the cancer," says Ganesh Palapattu, M.D., professor of urology and chief of urologic oncology at the University of Michigan Comprehensive Cancer Center.
Palapattu compares it to shooting fish in a barrel with your eyes blindfolded. UroNav is like taking off the blindfold. (For example, the photo above shows an ultrasound image and then the fusion MRI/ultrasound image, which appears more clear and precise.)
The technology allows urologists to know where a suspicious lesion is so a biopsy needle can be targeted more precisely. In addition, the system can store the trajectory of needles so repeated biopsies can sample the same area. Michigan Medicine specialists used a similar system for research studies since 2012.
The technology is most useful for:
-
Men with a concerning prostate MRI
-
Men considering or who are under active surveillance for prostate cancer
-
Men with an elevated PSA or another concern for prostate cancer
MRI is primarily used to identify potential sites of prostate cancer when the standard workup does not identify disease — for example, a negative biopsy but a rising PSA.
"MRI has only become useful in prostate cancer diagnosis over the last several years. Advanced MRI technique, which we use extensively at Michigan Medicine, allows us to identify and target clinically significant prostate cancers. One of the nice side effects is that modern MRI tends to minimize the appearance of nonaggressive prostate cancers. So it really refines our ability to find the kind of cancer we want to find," says Matthew Davenport, M.D., associate professor of radiology at the U-M Medical School.
"MRI is key to this technique," says Jeffrey Montgomery, M.D., associate professor of urology at the U-M Medical School. "We have seen countless instances where fusion biopsy finally diagnoses men with prostate cancer after years of random biopsies missing the mark. It is making a huge difference in how we manage prostate cancer."
Beyond PSA
In addition to using MRI to help visualize the prostate, U-M urologists can use newer markers combined with the traditional PSA test to better gauge the risk of aggressive prostate cancer. A test developed at U-M called Mi-Prostate Score combines PSA along with a marker called PCA3 and a genetic anomaly discovered in U-M labs that's present in half of all prostate cancers.
SEE ALSO: What Men Should Know About BRCA Variant Testing
The combined test score gives a more accurate assessment of whether a man has aggressive prostate cancer.
"PSA has been criticized as a poor marker for prostate cancer. We're developing advances in prostate cancer diagnosis that go beyond just an elevated PSA. A PSA test may be part of the picture, but it's no longer all we have available," Montgomery says.
Some 161,000 American men are diagnosed with prostate cancer each year. Most men will die with prostate cancer, not from it, because their disease is slow-growing. But a subset of patients will develop fast-growing cancers that require immediate and aggressive treatment.
The challenge is reliably identifying which type of cancer a patient has.
"While prostate cancer may look the same from one patient to the next under a microscope, it may behave quite differently. This kind of behavior is driven largely by the genetics, the DNA sequencing of the cancer. The more information we can learn about a tumor — through better biopsies and better diagnostic tests — the more we will be able to tailor therapy for a patient," Palapattu says. "Our goal is to offer individualized treatment plans focused on each patient."
For more information about prostate MRI, UroNav, Mi-Prostate Score or prostate cancer care, call the Cancer AnswerLine nurses at 800-865-1125.

Explore a variety of healthcare news & stories by visiting the Health Lab home page for more articles.

Department of Communication at Michigan Medicine
Want top health & research news weekly? Sign up for Health Lab’s newsletters today!





