Young organ donors offer a key lifeline to other sick children in need. But misconception and fear can cloud the idea of donation, a poll found.
7:00 AM
Author |

This article was updated on April 7, 2022.
Many adults know the lifesaving value of organ donation. Millions of American adults have committed to help others in the event of their deaths.
But what about children?
MORE FROM MICHIGAN: Sign up for our weekly newsletter
Families must consent to donate those organs, says John Magee, M.D., section head of transplant surgery and surgical director of Pediatric Liver & Kidney Transplantation. But parents, even if registered as donors themselves, often find the decision tough after a devastating loss.
"It can be a difficult conversation, but organ donation should be a norm for everyone," says Magee. "It's often the only good thing that comes from an inconceivable tragedy."
That mindset, however, isn't reflected in a C.S. Mott Children's Hospital National Poll on Children's Health. The nationwide survey of 2,005 parents found that only 17% of those with children ages 14 and younger have interest in learning more about pediatric organ donation.
Of parents with teens, just 1 in 4 poll respondents said their new drivers had registered to be organ donors when receiving their driver's license.
There's good reason to narrow those gaps: More than 2,000 children in the United States are on an organ transplant waiting list. Although pediatric donors exceed recipients, many minors still wait longer than adults for a transplant because they may need an organ of a certain size.
SEE ALSO: The Faces of Transplant: How Organ Donation Saved Their Lives
Children may join organ donor registries in some states, Magee says, but this is not widely known — and parents must still offer consent for donation to proceed. Additionally, a child's primary care doctor often doesn't approach the family with the topic of donation.
Which is why the conversation should continue in order to shift attitudes and reduce misconceptions about organ donation, no matter an individual's age.
"This survey really highlights the need for more education," says Magee. "Nearly all children live a long and healthy life, but getting the word out early is still a good thing."
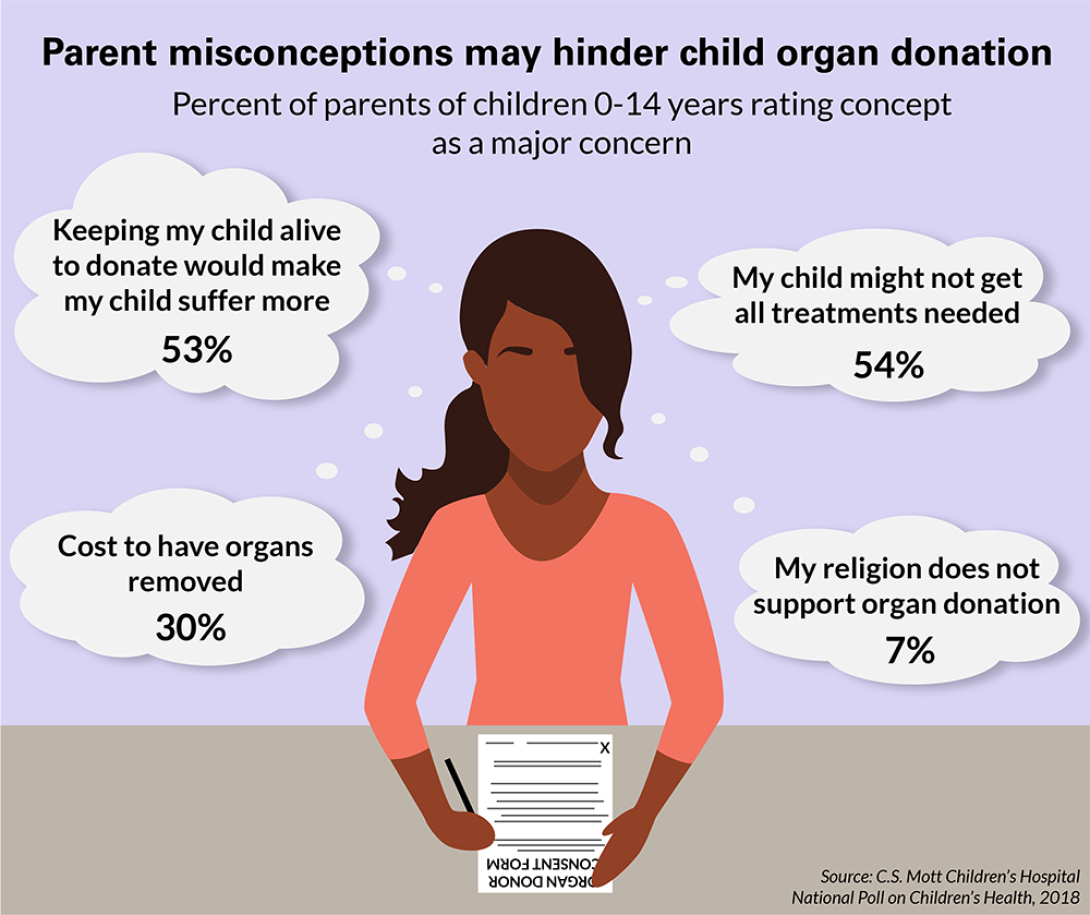
What to know about pediatric organ donation
It doesn't affect the care a living child receives: "When somebody's in the hospital, every effort is made to save their life," says Magee, who notes that transplant teams play no role in treatment before death. A resulting donation, if approved by a child's guardian, will not take place until a patient has been declared dead and has no potential to feel any pain.
Young donors are often best for other kids: Some organs, such as livers and kidneys, can be used from adult donors. But other organs must be a specific size to be suitable for a child recipient. Among them: hearts and lungs. "The need, particularly for a size-matched compatible person, is enormous," says Magee.
There's no pressure to donate: At the end of a young patient's life, a family will be approached about the option of donation. "The discussion is held in a very respectful way that recognizes the grief as well as the potential of helping somebody else," says Magee. Parents are also notified that the transplant, if carried out, would take place at no cost to them.
A minor can't make the decision alone: Older children may understand the value of being a donor, but their word isn't enough to give consent. Still, if appropriate, that conversation can lessen a family's reluctance should the unthinkable occur. Says Magee: "I've definitely seen cases where a child has told their parents: 'This is exactly what I would want to do.'"
Organ donation has physical — and emotional — power: A key point of comfort for many bereaved parents is that their child's organs can give another young person a new chance at life. "I know many families who look back on the act and consider it something that brought about a positive from an otherwise horrible situation," Magee says.

Explore a variety of healthcare news & stories by visiting the Health Lab home page for more articles.

Department of Communication at Michigan Medicine
Want top health & research news weekly? Sign up for Health Lab’s newsletters today!





