A common childhood illness peaks in the warmer months. A Michigan Medicine pediatrician explains what parents should know.
7:27 AM
Author |
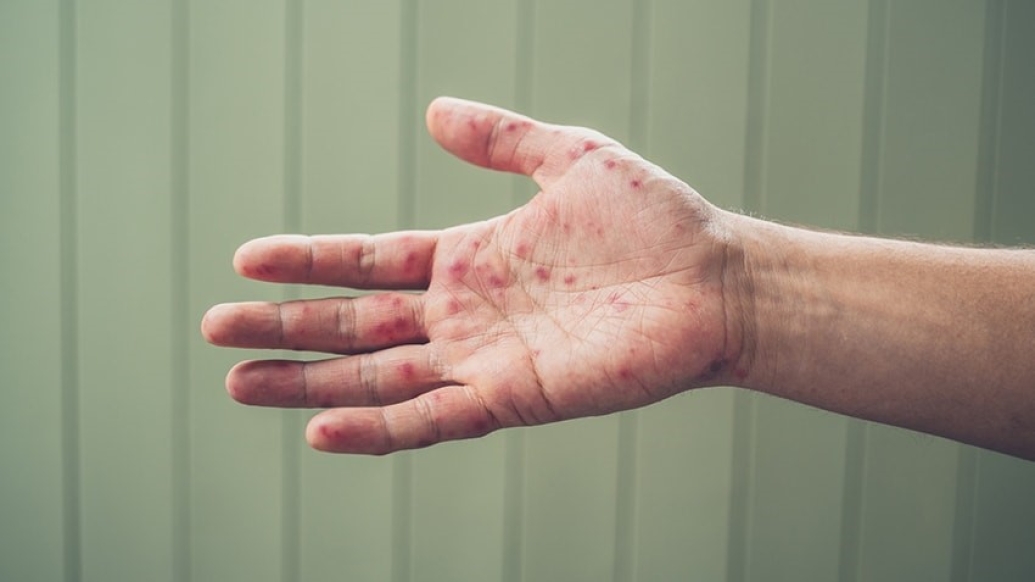
A highly contagious viral infection, hand, foot and mouth disease can surface on the body parts that make up its name.
"You often see tiny blisters in the mouth or a rash that can appear in other locations but commonly appears in the mouth, on the fingers, palms, buttocks and on feet," says Ashleigh El Sakr, M.D., a Michigan Medicine C.S. Mott Children's Hospital pediatrician.
Cases typically spike in summer and early fall. It is most commonly seen among infants and children younger than 7 years old, though it can be seen in older children, adolescents and adults.
In fact, two Major League Baseball players grabbed headlines this summer after contracting the disease. New York Mets starting pitcher Noah Syndergaard ended up on the disabled list, followed by New York Yankees hurler J.A. Happ whose case was mild enough that he wasn't expected to miss a game.
Signs and symptoms
A key sign of hand, foot and mouth disease is the appearance of sores, which vary by patient in size and location.
"The rash can include flat or raised bumps, or they can be more blister-like," El Sakr says. "Often, those blisters rupture pretty easily."
LISTEN UP: Add the new Michigan Medicine News Break to your Alexa-enabled device, or subscribe to our daily audio updates on iTunes, Google Play and Stitcher.
Common side effects include fever and mouth pain. Nonverbal children unable to express their discomfort may refuse to eat or have increased drooling.
Bumps and blisters usually are not itchy or painful, and the fever is temporary.
Dealing with the disease
"Though hand, foot and mouth can be a mild illness, children with symptoms are at risk for dehydration and should be monitored closely," El Sakr says.
Most times, however, families can handle a child's infection without an in-office visit.
There is no prescription treatment for hand, foot and mouth disease. The virus must run its course, with patients typically starting to improve within seven to 10 days.
To ease mouth pain and fever, El Sakr recommends acetaminophen (Tylenol) or ibuprofen (Motrin).
"We don't routinely suggest topical oral therapy in children as there is limited evidence of benefit of lidocaine or Benadryl in kids," El Sakr says.
Dehydration due to fever and sore mouth is a known risk; parents should make sure their child stays well hydrated during recovery. Keep track of the number of wet diapers your child has, as well as fluid intake.
Says El Sakr: "If the child is acting normally, tolerating fluids with normal urination frequency and no excessive drooling, the patient can often be cared for at home without a clinic visit."
MORE FROM MICHIGAN: Sign up for our weekly newsletter
Once the fever is gone and a child is able to drink and eat, he or she can return to school despite the fact they're still likely carrying the virus.
In some cases, parents may notice some peeling or shedding of a child's fingernails months after symptoms subside. Rarely, neurologic or pulmonary complications may arise.
Prevention
Hand, foot and mouth disease is another reason to practice proper hand-washing and cough etiquette at all times.
Daycare facilities also should take note when a child is affected, making sure other students follow good hygiene etiquette and that classroom facilities are sanitized.
That's because the infection is most often caused by a coxsackievirus or an enterovirus and may spread by way of respiratory secretions – sneezes, coughs or even talking at close range – for up to three weeks after symptoms.
Hand, foot and mouth disease also can be transmitted from fluid in a ruptured blister, as well as through stool for up to 10 weeks after a child's symptoms resolve – an increased risk for kids who are toilet training or in diapers.
Because there is more than one strain of the virus that causes this illness, it is possible to have hand, foot and mouth more than once. Families should remain vigilant about cleaning hands and surfaces to minimize spread of infection.

Explore a variety of healthcare news & stories by visiting the Health Lab home page for more articles.

Department of Communication at Michigan Medicine
Want top health & research news weekly? Sign up for Health Lab’s newsletters today!