One in 50 people carry the gene for the neuromuscular condition.
5:00 AM
Author |

Sitting in her hotel room, Christine Erickson got a call from the day care. Something seemed wrong with William, the staffer said.
Erickson wasn't surprised to hear this about her six-month-old son.
Not soon before, she noticed William never brought his knees to his chest. The pediatrician told her to see how William progressed. Soon, he lost nearly all his muscle strength.
The neurologist knew the diagnosis right away and later confirmed it: spinal muscular atrophy. Children with the condition lack the protein needed for the survival of motor neurons that cause the muscles to fire. They will look more "floppy" than traditional babies, not achieving typical developmental milestones.
SMA causes children to progressively lose function and strength, and, prior to available treatment, kids with the most common form of the disease would need a ventilator to breathe or die by the age of two, says Alecia Daunter, M.D., a pediatric physiatrist at University of Michigan Health C.S. Mott Children's Hospital.
"In 2016, there was a major change in the field with the introduction of a medication called nusinersen," Daunter said. "This was the first treatment for a previously untreatable, progressive condition. Another exciting change came a couple years later, when a therapy was approved which replaces the SMN1 gene that is missing in SMA. An oral medication called risdiplam came out later. Together, this totally changed the disease trajectory because this is now a treatable condition and there is so much reason for hope."
The gene therapy, called onasemnogene abeparvovec, is most effective when initiated early, as are the other treatments. William Erickson received it at 11 months – less than two months after the therapy was FDA approved – guided by Erin Neil Knierbein, D.O., a pediatric neurologist at Mott.
"William was getting significantly worse, and, to Dr. Neil, this therapy was the only choice," Christine Erickson said. "Once he was treated, we noticed small changes within days, just a bit more movement with his ankles. Gradually, he improved even more. A year after treatment, I could put him on his hands and knees, and he could hold it for 30 seconds."
Now four years old, William Erickson can lift small objects above his head and zoom around in his wheelchair. He still faces daily challenges: sitting, getting out of bed on his own and drinking out of a cup. Small stuff, to William's mother.

"I don't take anything for granted," Christine Erickson said. "We're together when we didn't think we would be here. William won't have a bad lifestyle; it will just be different. We are just so grateful that he was diagnosed."
Screening for SMA
Unlike Christine Erickson, who learned of her son's SMA at eight months, Darlisha Barnes got a call just days after her daughter, Harley, was born in 2020.
"She was part of newborn screening for SMA," Barnes said. "We were in disbelief when they told us our child needed to see the neurologist. It wasn't until around three or four weeks old that Harley started to show significant muscle weakness."
Barnes was terrified for her daughter to receive the genetic treatment. Even though it showed positive outcomes, the drug was so new that there was no long-term historical data for it. On top of that, she had not seen many other Black families go through the experience.
"If you put SMA on top of the fact that black women die at higher rates when giving birth, and you are then giving your child to the medical system at such a young age, it's a different experience than some other families may have," Barnes said. "I think there could be a gap in support and resources to some families who are more vulnerable in this system.

Gaps in the health care system are exactly why universal newborn screening for SMA is so important, Neil says.
"We must ensure that everyone, regardless of race, insurance or socioeconomic status, is able to learn that their child will develop this condition and can have access to treatment," she said.
Once effective treatments became available, the largest barrier with SMA was the lack of early diagnosis. One in 50 people are carriers for SMA, and a child has a 25% chance of having the disease if both parents are carriers. But children like William Erickson were not yet being screened for it.
The ability to identify babies within 1 week of birth as genetically affected with SMA and quickly institute treatment, usually before they are 1 month old, has made an extraordinary impact in SMA care.Erin Neil Knierbein, D.O.
The federal government added it to the list of suggested conditions for uniform screening in 2018, and the state of Michigan started with preliminary screening in 2019, after William was born. As of 2022, 47 states screen for SMA and 97% of babies born in the U.S. are screened at birth, according to Cure SMA, a nonprofit organization that funds research and advocacy.
The ability to identify babies within 1 week of birth as genetically affected with SMA and quickly initiate treatment, usually before they are 1 month old, has made an extraordinary impact in SMA care, says Neil, who is also the medical director for the state's SMA newborn screening program.
"It has been a team effort to organize and mobilize all the key players at the state level and within U-M Health," she said. "Everyone understands the urgency for moving quickly with evaluations, insurance approval and administration of the medications." Additionally, U-M Health recently joined the Cure SMA Care Center Network, which Neil and Daunter say will help to ensure that patients receive optimal care at U-M and establish best practices nationally.
Within weeks after treatment, Harley Barnes made slow improvements. She worked consistently with Betsy Howell, P.T., her physical therapist at the U-M Health Pediatric Rehabilitation Center. Harley went from not being able to lift her arms and legs to being able to feed herself and operate a manual wheelchair.
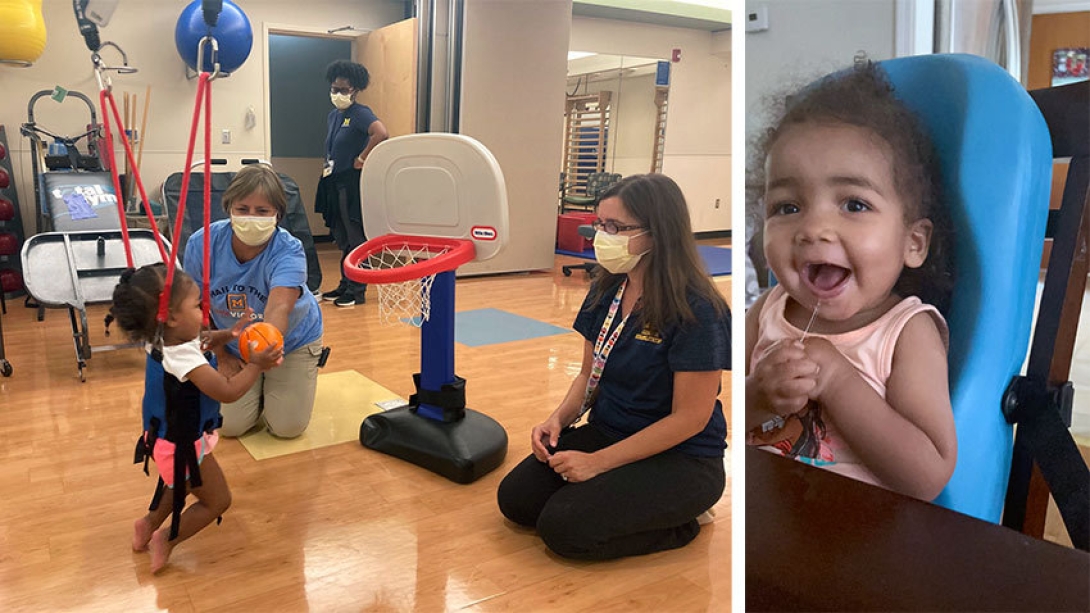
"Though the treatments are not a cure, they are gamechangers," Barnes said. "Harley is turning two in a couple of weeks, and instead of saying goodbye to her, like many families have had to before treatment, we get to plan birthday bash to celebrate. Harley is thriving; there is so much that she can do. She really wants to walk, and we pray she will be able to walk independently soon, but until then, she will be able to wheel into her second birthday party."
Learn more about the multidisciplinary SMA team at the C.S. Mott Children's Hospital. click this link.
Like Podcasts? Add the Michigan Medicine News Break on iTunes, Google Podcasts or anywhere you listen to podcasts.

Explore a variety of healthcare news & stories by visiting the Health Lab home page for more articles.

Department of Communication at Michigan Medicine
Want top health & research news weekly? Sign up for Health Lab’s newsletters today!





