A Michigan Medicine pediatric specialist explains what tonsillectomy and adenoidectomy entails, from examination to recovery.
7:00 AM
Author |
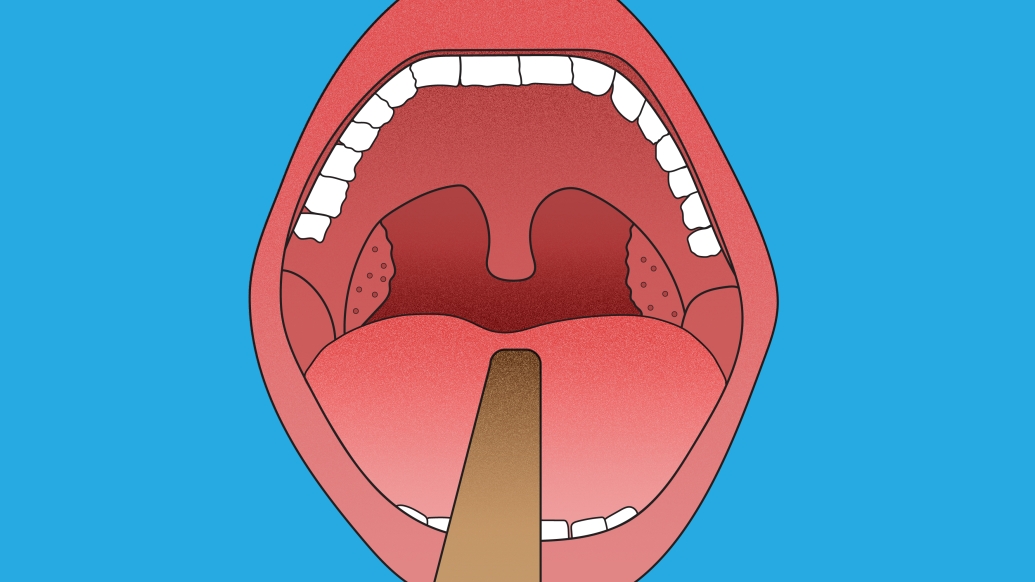
Tonsils are made up of lymphatic tissue in the throat that defend against viruses and bacteria that enter the mouth.
ASK ALEXA: Add the Michigan Medicine News Break to your Flash Briefing
The adenoids, a mass of lymphatic tissue in the back of the nose, play a similar role in the immune system.
But tonsils and adenoids may sometimes cause health issues in children and young adults.
When enlarged, the tissues can block the airway and cause sleep-disordered breathing, or sleep apnea. Both could also become a source of ongoing infection.
Because tonsils and adenoids may shrink over time, the troubles are temporary for some children. For others, surgery may be required to remove them.
It isn't recommended for every child, however.
"Removing them just because they're big is not a good idea — but when they're causing a problem with sleep or infections, the benefits outweigh the risks," says Aaron Thatcher, M.D., a pediatric otolaryngologist at University of Michigan C.S. Mott Children's Hospital. "Surgery doesn't cause significant immune system dysfunction."
Performed more than 530,000 times each year on patients 15 years old and younger in the United States, tonsil removal (tonsillectomy) is the second most common surgery for children.
When tonsils should be removed
Doctors utilize best-practice guidelines to determine if a young patient needs a tonsillectomy, Thatcher says.
When it comes to suspected sleep apnea, the warning signs can manifest as irritability, trouble focusing and poor school performance. The setbacks can impact "every element of a child's quality of life," Thatcher says.
There is strong evidence that tonsil and adenoid removal is effective in treating obstructive sleep apnea. Doctors may first order a sleep study (polysomnogram) to evaluate a child's sleep before going forward with surgery for sleep symptoms.
MORE FROM MICHIGAN: Sign up for our weekly newsletter
Sometimes, tonsils are removed because of chronic infection. The threshold: A child should have had seven recurrent tonsil infections within one year, five infections per year over a two-year span, or three infections annually over three years.
"Missing a lot of school can create problems with learning," Thatcher says. "It also creates a big strain on family who have to find care for child care during frequent infections."
Chronic ear or sinus infections or persistent nasal obstruction may warrant adenoid removal, also known as adenoidectomy, at the same time as or instead of a tonsillectomy.
What happens during tonsil and adenoid removal surgery
In most cases, doctors will remove a patient's tonsils and adenoids in the same procedure.
"We find that usually both are contributing to the obstruction of the airway," Thatcher says.
Performed under general anesthesia with a breathing tube in place, a tonsillectomy takes about 15 to 20 minutes. A doctor typically uses an electric cauterizing instrument to cut out the tonsils and seal off the blood vessels that feed them.
An adenoidectomy involves shaving or cauterizing the adenoid down to the base. A flexible catheter is used to hold the palate, and a dental mirror helps guide a surgeon's tool to the right spot.
Adenoidectomy without tonsillectomy is more common than a tonsillectomy alone, Thatcher says. An adenoidectomy usually occurs when a young patient needs a second set of ear tubes for recurrent ear infections or has chronic nasal obstruction.
A child's tonsils may be removed (and the adenoids left intact) if a child is having recurrent throat infections but isn't experiencing nasal obstruction.
Recovery from tonsillectomy and adenoidectomy
It takes patients longer to recover from having their tonsils taken out than from adenoid removal alone.
SEE ALSO: 10 Great Children's Books for Talking About Surgery, Sickness and Feelings
"Both will cause a sore throat, but the tonsillectomy pain is usually more severe and lasts longer," Thatcher says. Those patients may have discomfort for about a week; adenoidectomy pain lasts about three to four days.
Although most patients recover without incident, as many as 5 percent may experience complications such as bleeding, difficulty breathing and dehydration. Severe bleeding may require a second operation.
Complications are more likely in children with craniofacial anomalies, Down syndrome or bleeding disorders. Patients with sleep-disordered breathing who are 3 and younger also have an elevated risk. They're kept overnight for observation after surgery, Thatcher says.
Some patients may continue to experience viral infections (albeit less severe ones) or sleep problems.
Still, Thatcher says, the benefits are clear.
"It becomes much easier to live a normal life," he says. "I've had some children interested in athletics suddenly see a big improvement because they're sleeping better and able to breathe better. And teachers may see an improvement in a child's attention and focus."
C.S. Mott Children's Hospital pediatric otolaryngologists see patients at three clinics in Southeast Michigan. Learn more or call 734-936-5730 to make an appointment.

Explore a variety of healthcare news & stories by visiting the Health Lab home page for more articles.

Department of Communication at Michigan Medicine
Want top health & research news weekly? Sign up for Health Lab’s newsletters today!