He’s used to treating critically ill patients. But when he became infected with COVID-19, one critical care doctor found himself as a patient in an ICU.
1:15 PM
Author |
Editor's note: Information on the COVID-19 crisis is constantly changing. For the latest numbers and updates, keep checking the CDC's website. For the most up-to-date information from Michigan Medicine, visit the hospital's Coronavirus (COVID-19) webpage.
Interested in a COVID-19 clinical trial? Health research is critical to ending the COVID-19 pandemic. Our researchers are hard at work to find vaccines and other ways to potentially prevent and treat the disease and need your help. Sign up to be considered for a clinical trial at Michigan Medicine.
When the doctor becomes the patient in the hospital department where he trained, he knows better than anyone what he's up against.
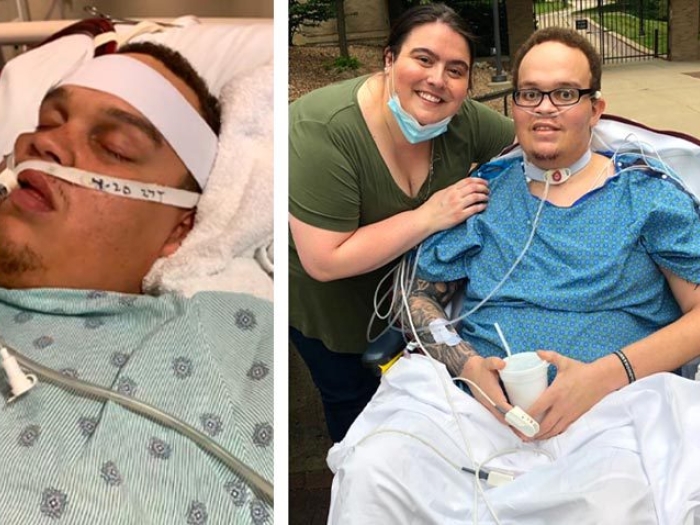
So for Eugene Vovchuk, M.D., the last month and a half have meant a bit of fear, many moments he doesn't remember while hospitalized, and the knowledge that after being on a ventilator for COVID-19, he's very lucky to be back at home with his family.
LISTEN UP: Add the new Michigan Medicine News Break to your Alexa-enabled device, or subscribe to our daily updates on iTunes, Google Play and Stitcher.
Vovchuk is an anesthesiologist and critical care physician in Detroit. His fellowship, part of his many years of medical training, was at Michigan Medicine.
"Being a critical care doctor myself I know that I faced a high mortality rate with what I had," he says.
Really sick, really fast
It all started on March 13 with a fever. Vovchuk stayed home from work and quarantined himself in the master bedroom, thinking it was probably influenza. But then the nausea hit, and he started having trouble breathing. He kept getting sicker.
He knew it was time to go to the hospital.
He was admitted at Michigan Medicine, intubated for 12 days, and then needed several more days to overcome delirium. His heart was also beating too quickly, and now he's dealing with high blood pressure, too.
SEE ALSO: Treating One of Their Own: COVID-19 Breaks Myth of Invincibility for Hospital Doctors
Connecting with family
For weeks, Vovchuk could only see his 1- and 3-year-old daughters and his wife via FaceTime. The visitor restrictions, necessary to stop the spread of the disease, can lead to loneliness for many COVID-19 patients, and increased anxiety for their loved ones at home.
What Vovchuk didn't know while he was intubated was his doctor was helping his family keep in touch with their dad and husband.
"I got to learn a lot about him from his wife," says hospitalist Julie Barrett, M.D. "I talked with his mother, too. I would turn the camera toward the window and his daughters would sing to him."
MORE FROM MICHIGAN: Sign up for our weekly newsletter
Vovchuk was one of Barrett's first patients in the RICU, the Regional Infectious Containment Unit, which is an isolation area opened just for COVID-19 patients. She also cared for him at the end of his hospital stay where she could see how much he was improving.
"He unmistakably had COVID-19," Barrett says. "I have never seen someone so young and so sick. You just don't see a 38-year-old that sick who was previously healthy."
Deciding the best treatment
Vovchuk was admitted to Michigan Medicine because he was so sick, doctors thought he may need ECMO. Short for extracorporeal membrane oxygenation, this intensive care therapy is thought to offer a last chance at life for the sickest COVID-19 patients. Not all hospitals are able to offer the treatment.
SEE ALSO: When Ventilators Don't Help COVID-19 Patients, This Might
The ventilator in the hands of skilled surgeons ended up ultimately being enough, says hospitalist Valerie Vaughn, M.D, MSc.
"It was the coolest thing to walk into his room and to finally be able to have a conversation with him after knowing his medical history so well. But yet, with all I knew about him, I had never seen the color of his eyes, or heard the sound of his voice," Vaughn remembers. "Then, one day, he looked up and said, 'Who are you?' That was a fun moment."
Vaughn happily wrote Vovchuck's discharge orders on April 15, when he was symptom-free and fever-free for three days, and his most recent COVID-19 test came back negative.
'A new take on life'
"I feel extremely fortunate to be alive, and I look at this as honestly a new take on life," Vovchuk says. "I'm going to definitely be changing some habits, like being more active and being healthier. I feel very fortunate."
Vovchuk's medical know-how may also be what's making him cautiously optimistic as he settles in at home.
"I still have months of rehab ahead of me, both cardiovascular and physical," he says.
And the long-term effects of a COVID-19 infection are not yet known.
But while he manages those concerns and keeps recovering, he is already able to do the one activity he'd been waiting weeks to do: hug his daughters and his Yorkie dog, Rocky.

Explore a variety of healthcare news & stories by visiting the Health Lab home page for more articles.

Department of Communication at Michigan Medicine
Want top health & research news weekly? Sign up for Health Lab’s newsletters today!