Before entering the pressurized oxygenated room or tube, here’s five things you can expect.
3:39 PM
Author |
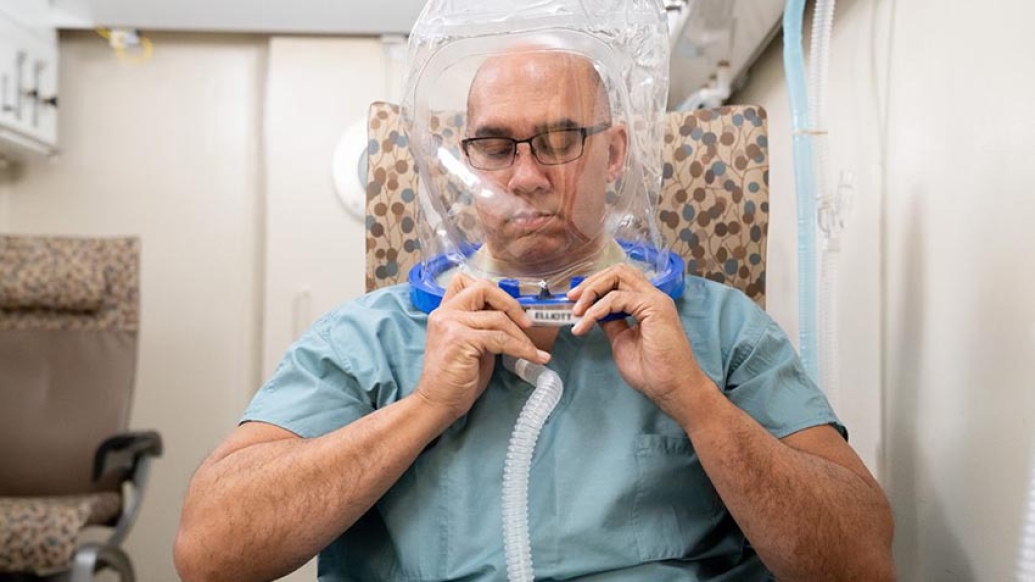
Kate McKenney says patients go for a deep dive at their clinic each day, but they're not going in a swimming pool or lake — or any body of water at all. Instead, they enter a hyperbaric oxygen chamber, which helps wounds heal faster and more effectively.
"We call our treatments 'dives' because our chamber is pressurized to 2.2 ATA (atmospheres absolute), which is the equivalent of scuba diving down 40 feet of seawater," says McKenney, the administrative manager for the Michigan Medicine Comprehensive Wound Care Clinic. "It's a unique treatment that not many people know about."
When body tissue is injured, it may require more oxygen to heal. Hyperbaric oxygen therapy involves breathing in oxygen at a high pressure to help fight infection and induce wound healing.
The pressurization and oxygen hoods are the most important aspects of the therapy. The hoods increase the oxygen that your lungs take in, and the pressurization increases the amount of oxygen your blood absorbs. This delivers more oxygen to parts of the body where it may be in short supply. The extra oxygen can assist with healing, fighting infection and has also been shown to stimulate the release of stem cells and growth factors.
"The increased atmospheric pressure, along with the patient receiving 100% oxygen through the hood, allows both your blood and blood plasma to carry oxygen more effectively," says Rob DeLeon, lead hyperbaric technician. "This saturates the body with oxygen and improves the body's effectiveness in healing wounds."
MORE FROM MICHIGAN: Sign up for our weekly newsletter
Some diagnoses by a doctor include including non-healing wounds from arterial disease, along with advanced diabetic foot ulcers, stubborn bone infections and problems due to prior radiation treatment, which can present as slow healing soft tissue wounds, avascular necrosis of the bone or radiation cystitis. "We treat patients with a variety of diagnoses in our chamber," says Steven Haase, M.D., the medical director of the clinic. "But each indication is backed up by scientific research and endorsed by experts in the field."
How it works
Hyperbaric medicine has been done for a long, long time, according to McKenney. "The first treatment was done in the 1930s by the U.S. Navy for decompression sickness. Treatments have been performed in healthcare settings since the 1950s or 1960s. Our safety protocols are still based on Navy research," she explains.
There are two types of chambers patients may come across. "A multiplace, which is like a room or a small airplane, like we have here, or there are also monoplace chambers, which are best described as 'tubes.' They are smaller and designed for one person to lay down while receiving treatment," McKenney says.
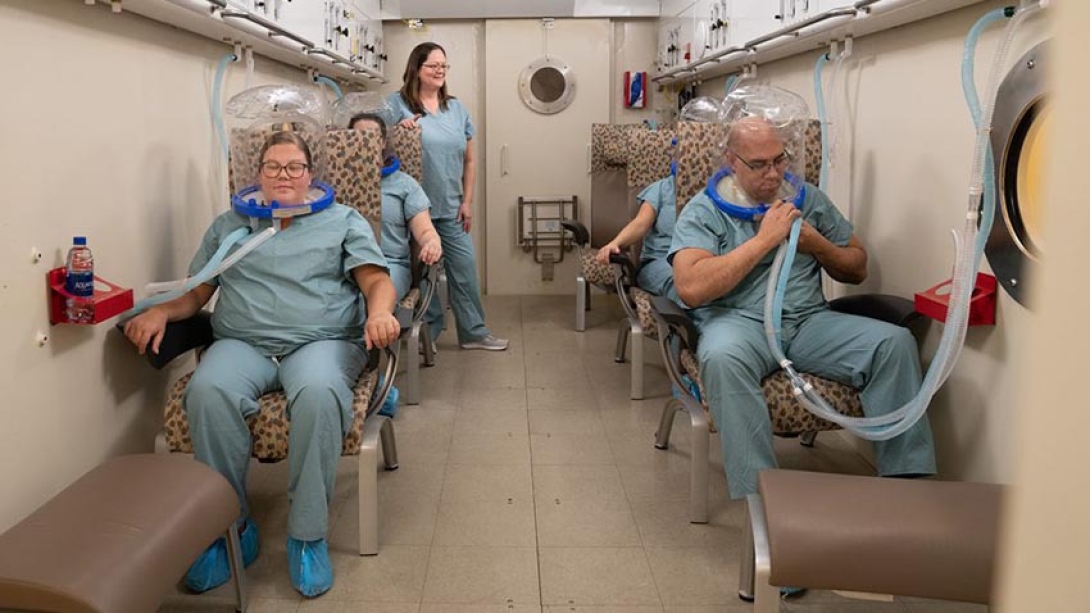
At U-M, the oxygen chamber is a room where up to 10 patients and two staff members spend two and a half hours at a time for treatment.
"When a patient comes in, the chamber is pressurized, and once at pressure, a hood is placed on the patient, which provides them with 100% oxygen," McKenney says.
The chamber at Michigan Medicine, situated at their Domino's Farms outpatient location, allows those inside to stand up and move around whenever they'd like.
"Think of it like an airplane cabin," McKenney said. "Patients sit together, there is a television and Netflix in there, and you get to know one another."
Patients wear the hood for 30 minutes at a time, then take it off for 10 minutes. The patients are continually monitored by staff members in the chamber. That cycle takes place three times before the daily treatment is complete.
Before starting therapy
Haase and DeLeon recommend knowing these five facts before entering a hyperbaric oxygen chamber for therapy:
1. Don't arrive sick to the appointments.
Your treatment might be delayed if you have a cold or other illness such as high blood pressure, fever, frequent loose stools or any flu-like symptoms. "If a patient has a cold, it could affect their ability to clear their ears, which could lead to inner ear injury," DeLeon says.
2. Certain medications should be avoided ahead of time.
Oxygen may change the effects of certain medications. While receiving therapy, there are a handful of medications that cannot be taken in combination with this treatment, such as some chemotherapies, a topical ointment used for wounds and a medicine that prevents alcohol intake in patients with a history of alcohol abuse.
Be sure to speak with your physician and health care providers in advance to discuss any drugs you're taking.
3. Expect to be there for a few hours.
Hyperbaric oxygen chamber therapy sessions last a little over two hours and are generally scheduled once a day, five days a week. Your doctor may prescribe 30 or more treatments before the therapy is complete. How many treatments you have is often dependent on how quickly your condition improves.
Like Podcasts? Add the Michigan Medicine News Break to your Alexa-enabled device or subscribe for daily updates on iTunes, Google Play and Stitcher.
"The actual treatment takes about 110 minutes; 90 minutes of oxygen with two 10-minute air breaks. The rest of the time is for the descent and ascent time," DeLeon says.
4. You may feel like you're on an airplane at first.
Some people say the start of this therapy feels similar to flying on an airplane. As the pressure builds in the chamber, so does the pressure within your ears, which may leave you with an ear-popping sensation.
"During out treatments we have protocols that help avoid putting a patient in a situation where they have fluid buildup or pain in their ears," DeLeon says.
5. Some potential side effects to be aware of.
Feeling tired after your treatment is normal, and so is pain in your ears or sinuses, or the feeling of fluid buildup in your ears.
If you're claustrophobic, being confined in the chamber could also make you anxious. Vision changes and finger numbness can occur, but both usually subside during the treatment. With the increased pressure and breathing in of 100% oxygen, you could also feel woozy, or even giddy.
In very rare cases, seizures or a collapsed lung can occur due to the treatment, and it can potentially increase the progression of cataracts.
"A collapsed lung would only occur if the patient had emphysema or another lung disease where air could get trapped in small blebs (a blister filled with fluid) and burst with the pressure changes. But this is extremely, extremely rare," Haase assures.
Although rare side effects can occur, McKenney notes that a trained and certified health care professional is always present on site during the entirety of your treatment, which is a nationwide rule.

Explore a variety of healthcare news & stories by visiting the Health Lab home page for more articles.

Department of Communication at Michigan Medicine
Want top health & research news weekly? Sign up for Health Lab’s newsletters today!





