A close encounter with death changed David Lossing’s life forever. Now, he and his family want to share a message of awareness.
7:00 AM
Author |

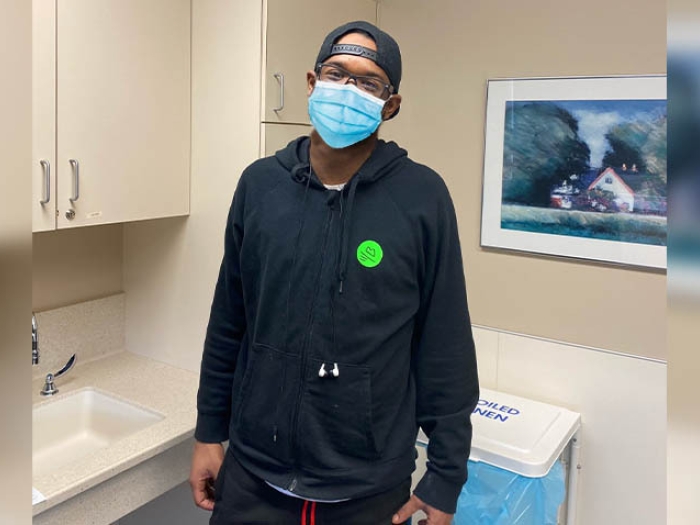
One day on the job, David Lossing was suddenly struck by a sore throat and tightness in the chest.
"I just didn't feel right," says Lossing, a restaurant manager from St. Clair County, Michigan. "I sat down and called my wife."
LISTEN UP: Add the new Michigan Medicine News Break to your Alexa-enabled device, or subscribe to our daily audio updates on iTunes, Google Play and Stitcher.
He didn't imagine those symptoms would prompt a helicopter flight to Ann Arbor for emergency surgery.
Lossing owes a debt of gratitude to his wife, Nancy, who urged her husband to call 911 immediately, even though he wasn't experiencing any sharp, shooting pain.
"If I had told him to wait until I could get to him or we second-guessed calling 911, that would've been it," says Nancy, who has unstable angina and knows the value of quick care.
When paramedics arrived, Lossing's blood pressure was 40/30 mmHg. That's extremely low: Normal blood pressure is considered 120/80.
His skin was losing color because blood wasn't circulating in his body and oxygen wasn't reaching his brain.
Survival Flight, the critical care transport program of Michigan Medicine, flew 100 miles northeast to pick up Lossing. He was rushed to the University of Michigan Frankel Cardiovascular Center, where cardiac surgeon Bo Yang, M.D., was waiting.
Because Survival Flight communicated with emergency department physicians on the ground, they had the greatest chance of saving his life after a diagnosis was made.
"David had an acute type A aortic dissection," Yang says.
In other words, the layers of Lossing's aorta were pulling apart, trapping blood between them and threatening his main artery's ability to supply his body with oxygenated blood.
"This type has a high risk of rupturing, and once it ruptures, it's difficult to save the patient," Yang adds. "He bled from his aorta, and that blood was compressing his heart. Even if you have a strong heart, if there's no blood circulating, that's not compatible for life."
Be aware of your family history as it relates to heart and aortic disease.Bo Yang, M.D.
Treatment for aortic tear
Without immediate intervention, Lossing probably would have died.
"We ran from the emergency department to the operating room," Yang says. "Everyone moved very quickly, and across specialties we worked simultaneously to prepare for surgery."
MORE FROM MICHIGAN: Subscribe to our weekly newsletter
Before Lossing's arrival, teams across disciplines worked to prepare the operating room and the heart-lung machine, which takes over the functions of those organs during surgery.
"Every second counted, and we needed to be immediate but precise in every move we made," Yang says. Blood was filling the space around Lossing's heart, adding pressure that had to be relieved.
After resuscitating Lossing, Yang and his team performed a sternotomy and relieved the compression of the heart. Then, they performed an aortic root repair, replacing the ascending aorta and aortic arch with complete resection of the tear.

Complications and recovery
Although the operation was a success, Lossing's blood wasn't clotting afterward.
Bryant Wu, M.D., an assistant professor of anesthesiology, worked with his team to get Lossing's blood to clot. New cardiothoracic surgery fellow Carlo Rosati, M.D., sat at Lossing's bedside all night to monitor his progress.
Before Lossing's 10-day stay at Michigan Medicine was through, Survival Flight staffers even made a surprise visit.
"These were the guys that helped keep me alive on the way to the hospital," Lossing says. "I know people like to say they're just part of the team, but a team is made up of individual people, and these people saved my life."
Causes of aortic dissection
Lossing's good health and lifestyle made the events all the more surprising.
"David didn't drink or smoke," Nancy says. "He walked every day. There was no indication of something like this ever happening."
SEE ALSO: For Cardiac Success Story, Survival Starts with Self-Awareness
The couple learned a traumatic event might have been responsible. Earlier that day, Lossing lifted a 200-pound sign that had fallen at their restaurant, which could have triggered the aortic dissection.
Another possibility that physicians generally see more often: genetics. Some mutations are known, and some are unknown.
"Be aware of your family history as it relates to heart and aortic disease," Yang says. "These are dangerous diseases. If someone has an aortic dissection, it's normally related to genetics and there's a gene variance that caused the walls of the aorta to be weaker. Family members should be screened."
Just weeks after returning home, Lossing — a father of two and grandfather of six — was able to get back in shape by walking multiple miles every day.
The family hopes their experience reminds others to be vigilant.
"We feel God brought David through this for a reason," Nancy says. "We want to share this story. It could save someone's life. Don't ever hesitate calling 911."

Explore a variety of healthcare news & stories by visiting the Health Lab home page for more articles.

Department of Communication at Michigan Medicine
Want top health & research news weekly? Sign up for Health Lab’s newsletters today!