They were the first to answer the call in March 2020. Now, they reflect on COVID and how their lives have changed.
1:10 PM
Author |

Two years ago, Michigan reported its first case of COVID-19. Nearly two weeks later, Governor Gretchen Whitmer announced a stay-at-home order to "flatten the curve" of daily COVID cases and deaths.
The first of several vaccines against the novel coronavirus were made available in late 2020, saving scores of lives across the globe. However, the virus mutated, and large portions of the population were not vaccinated. Several waves later, over 950,000 Americans and 32,000 Michiganders have died of COVID-19.
Through everything, the health care workers – physicians, nurses, therapists and so many more – who answered the pandemic's initial alarm continue working to keep individuals and communities healthy.
That commitment comes with enduring waves of death and trauma, harmful misinformation and eroding public trust. Here, several University of Michigan Health faculty and staff members reflect on their personal and professional experiences during the pandemic, sharing hardships most may not have felt or seen outside of the hospital walls.

Tessa Adzemovic, M.D., M.S., internal medicine-pediatrics resident
The first eight months of Tessa Adzemovic's residency training were exciting, tiring and – with the benefit of hindsight – normal. Grief and suffering existed as always in the hospital, but the Toronto native was lifted by the myriad of profound patient interactions she experienced as a rookie physician starting in July of 2019.
Like everyone's, Adzemovic's world changed in March 2020. She remembers the specific moment: a hospitalist and mentor of hers ran into the ICU carrying the results of an arterial blood gas test for a patient whose blood oxygen levels had quickly dropped. "I think [they] may have COVID," the hospitalist told her. His clinical suspicion was right – it turned out to be one of the first critical cases the hospital would see.
"One of the most astonishing things about the beginning of the pandemic was that we were all learning together: the residents, the attendings, the respiratory therapists and the nurses - it was a shift of the traditional paradigm," Adzemovic said. "The hospital, and particularly the ICU, always has an element of unpredictability, but now we were treating a condition we didn't even know existed six months back. We saw complications in quantities we hadn't experienced before. We facetimed with families when prior we were able to hold their hands."
The guidelines came and changed furiously. Masks, gowns, visitor restrictions. For Adzemovic, the most challenging part of going through the early stages of residency in a pandemic was not being able to go home and see her family. At the same time, she recognized that the patients couldn't see theirs either. "Before I go into every patient room, I think, 'This is someone's parent or loved one,'" she said. "I may not be able to be with my family, but I will make sure to provide the most compassionate care to the patients I have the privilege of being with during this difficult time."
Adzemovic fears for the loneliness of a generation of young physicians. She knows residency training is difficult and isolating in general, but COVID-19 has exacerbated that into a new form of anguish. On top of that, she finds it difficult to see "people living as if nothing has happened when we have nearly 1 million dead and unprecedented global inequities." She's felt the effects of misinformation in the hospital – in patients asking for ivermectin before getting intubated, inquiring about bleach, and declining to wear masks.
But she's also seen people change. One young father who was stabilized during a long COVID-19 hospitalization told Adzemovic he would vaccinate his child when he got home. It's a unique privilege, she says, being able to impact future choices even if she can't impact the past.
Adzemovic remains tired but wouldn't change her experience for anything. "I've learned to live with a lot of grief, but I love what I do," she said. "The pandemic has unroofed a lot of inequities that have existed for generations, and it's inspired me to be a more vocal advocate for my patients both inside and outside of the hospital."
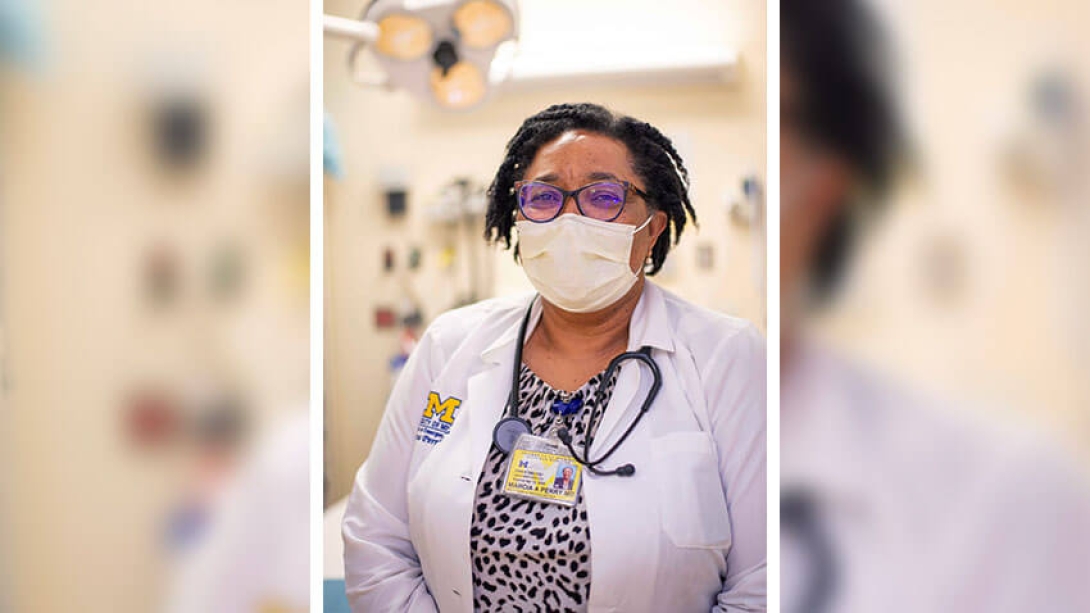
Marcia Perry, M.D., emergency physician
Back in November, Marcia Perry worked a "short shift" in the emergency department from 11 a.m. to 4 p.m. The ER was busy, so the shift manager asked Perry to work the triage area, sending patients to the appropriate places. There were 60 people in the waiting room.
She ran for all five hours, helping many patients who were able to leave without being admitted. "They kept coming and coming," Perry said. "At the end of my shift, there were 71 people waiting. I was exhausted and felt like I did nothing to help."
Normally, after a shift like this, Perry and her coworkers would blow off steam at a local restaurant. But the 25-year veteran physician who sees COVID patients every day worries about "slacking up her vigilance." Since the start of the pandemic, she hugs less and sees fewer friends. Perry has two teenage daughters, one with asthma. She didn't see her 86-year-old mother for nearly two years.
"I've had multiple thoughts about retirement; I'll be 60 this year," Perry said. "I've been so exhausted, but I would like to get my girls on their way before I do that. So, I keep pushing every day."
Over time, Perry noticed herself and her colleagues getting more easily frustrated. Patients had been coming to the emergency department forever for things that are not emergent, but she was now having to tackle a parallel deluge of misinformation and animosity. Some patients were triggered by simple questions about COVID-19 or the vaccine. "I had to check that frustration very quickly," she said. "It's difficult when you don't have the opportunity to educate patients. I now ask, 'What questions do you have about COVID or the vaccine?'"
Perry continues to "do everything" not to bring COVID to her workplace because, more than anything, she fears giving it to someone else. She hopes others will do what they can not to bring it to her.

Rachel Frederick, M.D., emergency medicine resident
"I have never been a doctor without COVID."
One week before she matched for her residency, everything shut down. Rachel Frederick was pulled from her clinical rotations; match day was cancelled, and graduation was virtual. "We didn't close that chapter in the way we expected to," she said.
The new chapter came rapidly, three months into the global pandemic. Frederick and her co-residents couldn't spend time together or engage in teambuilding activities. In a way, she says, they had to grieve the loss of that connection.
The full gown and personal protective equipment are all Frederick has known. "In the emergency department, we have a really short amount of time to connect with patients and learn how to treat them appropriately," she said. "It's how we build some semblance of trust and communicate that we have their best interests at heart. Doing all that in PPE is incredibly difficult."
For a lot of residents in Frederick's class, the first patients they intubated and later pronounced dead were lost due to COVID. During surges when the waiting room numbers hit new highs and staff had to run all night to find places for patients, Frederick assumed she was just getting accustomed to the job. She didn't know anything different. "But when your attending says, 'We got crushed tonight,' those moments are eye-opening," she said. "With this much acuity and volume and people who can't get timely care, this is not how things are supposed to operate."
Frederick has a pre-adolescent son, and she's grateful for the extra time she got to spend with him while they both attended school at home. But now in residency during a pandemic, much of her emotional energy is spent at work. On top of that, she's constantly thinking about what she might bring home.
"I've chosen this career path, and I know the risk when I go into the emergency department," Frederick said. "That's not something my family got to choose. Knowing my choice puts them at risk is hard to reconcile. It's been difficult, but it is such important work to me."

Jakob McSparron, M.D., pulmonary critical care physician
On a January night, he turned on an NBA game to see thousands of people and almost nobody wearing masks. The next morning, Jakob McSparron woke up at 5 a.m. and headed to the hospital where more than half of the patients in the ICU were on ventilators due to COVID-19.
"Many of them were really trying to do the right thing," he said. "Some of them are immunosuppressed and got unlucky because other people were not careful. I have this strange tension between normal events and going back to an overflowing hospital, and that's really painful."
During the first surge in 2020, spirits and adrenaline were high in the hospital's intensive care units. McSparron's team is trained to take care of people with lung disease and respiratory problems. In a sense, COVID was in their wheelhouse.
"That feeling carried us for what felt like a long time," said the ICU physician of 10 years. "I helped run the Regional Infectious Containment Unit, and it was truly all-hands-on-deck."
Once the RICU closed, most patients with COVID-19 were sent to McSparron's primary ICU, the Critical Care Medicine Unit. Quickly, around 70-80% of his patients were sick with the virus, leaving few beds for people with other critical illnesses. The work became even more challenging when they realized there was no end in sight.
MORE FROM MICHIGAN: Sign up for our weekly newsletter
His frustration occasionally feels closer to anger. McSparron hears more people saying getting infected with COVID is inevitable; meanwhile, the hospital has had to limit transfers, surgeries and admissions for many patients to cope with the COVID surges. His wife is pregnant with their third child, yet McSparron has taken care of more young, healthy pregnant women in the ICU in two years than in his entire career combined. All of them unvaccinated.
"I don't describe myself as burnt out, but compassion fatigue feels real," he said. "In those cases where everybody in the family is unvaccinated, and there is a pregnant woman on life support with a baby who has a very high chance of not living or being delivered very prematurely, I just don't always have it in me to have the conversation about vaccines again."
McSparron has a lot of friends who tell him they "have to keep living." And while he doesn't believe things should shut down again, McSparron doesn't want the vulnerable and immunosuppressed, as well as the children too young to be vaccinated, to be forgotten.
"I have never seen our teams as tired as they are these days," he said. "We all want to return to normal, but the virus is not gone. We can continue to protect each other with small changes in behavior."

Christine Reppke, R.N., emergency medicine nurse
During the pandemic, the emergency department waiting room set up a smaller, separate triage space for COVID-positive patients to limit spread among patients and staff. When omicron came, Christine Reppke felt the small waiting room would be better utilized by patients who didn't have the virus.
Previous outbreaks, like H1N1 in 2009, felt more distant to Reppke. Initially, she and some of her nurse colleagues thought the coronavirus would be "six weeks of torture" before dropping off. She thought something similar would happen when the vaccines were made available.
"Two years in, having not had COVID while working in the ER feels like walking in a minefield," Reppke said. "There are all the stressors of being busy making sure you're doing the best you can for your patients, but I'm also constantly worrying. 'Am I going to be OK? Is my family going to be OK because I went to work today?' The idea of us not being done is overwhelming."
Reppke wishes people stopped seeing her job as political. She doesn't want anyone to have to see the ER on a busy day, and she doesn't want people to suffer from COVID or lose someone because of it.
"When I say I'm watching people die from this every day, I wish people didn't believe that I'm exaggerating," she said. "I don't have a political agenda. I'm watching people suffer."
Reppke tries not to be judgmental when talking to patients' family members who argue with her about the virus as she works to keep their loved ones healthy. It can be disheartening and hard to show up every day. Several colleagues have left the emergency department for other areas of the hospital that may be deemed less risky or confrontational. Reppke has thought about it, too.
She would miss the emergency department, though. The environment suits her; Christine is drawn to it. "Even though it's frustrating, there's more rewarding parts of it than frustrating parts," she said.

Cecile Hollinshead, PA-C, emergency medicine physician assistant
Before coming to Michigan Medicine, she was a physician assistant in Norfolk Virginia, a hub for multiple military bases. In the aftermath of September 11, 2001, that was the first time Cecile Hollinshead felt truly unsettled working in health care.
"We were afraid the military bases would be hit," she said. "If they really wanted to instill terror, they could have hit the ERs in the area. It was the first time I experienced something that was unknown."
Two years ago, she felt a new kind of uncertainty. Hollinshead and her husband, Patrick, are both physician assistants in the emergency department. They have two pre-adolescent kids and no extended family to help take care of them.
"Our kids understand that every day that we go into work is a chance that we come home sick," she said. "We both felt that it is our job to be at the ER to help others, so we show up when we're scheduled. But it's always in our minds when we go to work."
Burnout shows up in different ways for Hollinshead. She feels it when advocating for really sick COVID-positive patients who want to leave hospital and don't know the ramifications that could have. She feels it when family members refuse to believe what she is saying about their loved ones in serious condition.
Hollinshead has also seen several colleagues, both physician assistants and nurses, leave the field. She understands. They see patients at their worst – medically, emotionally, psychologically. But it doesn't make it easier. "The people in the ER are my second family," she said.
For Hollinshead, the ER is where she should be. She likes the full spectrum of cases they see, the challenge of it all. But in the future, she hopes everyone will show more empathy and respect to her and her team.

Vikas Parekh, M.D., hospitalist and associate chief medical officer, capacity and operations
Over two years, Vikas Parekh has gotten really good at modeling COVID-19 trends. He's correctly forecast the last five surges, helping the hospital prepare for the worst.
And he'd really like to stop doing it.
"People sometimes try to make it seem like everything is OK, and that's just not the case," he said. "There's just this general sense of frustration from health care providers who have been out on the front line while other people have moved on and forgot what's happening in health care systems every day."
It's been continued déjà vu for Parekh. He sees a new variant of COVID "explode" somewhere else in the world, and then he and his colleagues are hit hard in the hospital.
"There's a lot of burnout and fatigue," Parekh said. "There is some degree of disillusionment, especially with omicron and a lot of messaging in the press that it is mild. Conceptually, on a grand scale, it is milder. But when you're in the trenches at the hospital, it doesn't mean anything. We were taking care of patients who had severe COVID, and the hospital was full again to the point where we were cancelling procedures and surgery."
Parekh comes from a medical family. His wife is a physician as well. His whole family is vaccinated, and several of them had COVID already, but they've mostly avoided gatherings and taken precautions that many people now forgo.
Keeping a positive outlook is not always easy. Parekh just tries do what he can to assist the health care system.
"Taking care of patients in front of me is really grounding," he said. "I focus on supporting my team of residents and students on the inpatient floors, as they navigate these challenges – grounding us in core principles of compassion and why all of us are here in the first place – to care for patients who need us."
Like Podcasts? Add the Michigan Medicine News Break on iTunes, Google Podcasts or anywhere you listen to podcasts.

Explore a variety of healthcare news & stories by visiting the Health Lab home page for more articles.

Department of Communication at Michigan Medicine
Want top health & research news weekly? Sign up for Health Lab’s newsletters today!





