Suddenly in the spotlight, this common lung infection has a lot of causes but can also be prevented in many cases. Learn more to protect yourself.
1:00 PM
Author |
It doesn't usually get a lot of attention. But all of a sudden, pneumonia has captured attention thanks to Hillary Clinton's case. Two experts offer some key information to help you and your loved ones avoid it — or get the best treatment if needed.
Facts about pneumonia
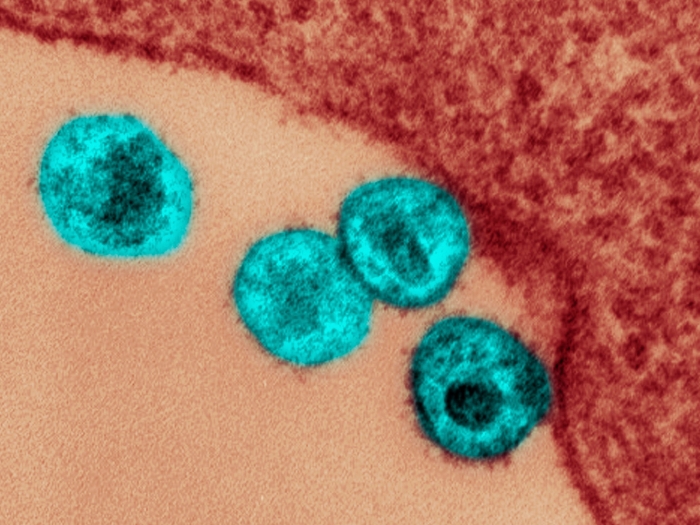
It has dozens of causes. A wide range of bacteria and viruses can cause pneumonia, from garden-variety flu viruses to nasty, antibiotic-resistant bacteria.
SEE ALSO: Bad News About the FluMist Nasal Spray
Infection-causing microbes want to escape the body's immune system defenses, and get from the mouth and nose into the lungs. Once there, the little nooks and crannies can be a great place to settle in to reproduce.
Then, patients cough up the phlegm that infected lungs produce, meaning the microbes' offspring can spread to their next human home.
Getting it makes you one in a million. About a million Americans end up in a hospital bed because of pneumonia every year, another 4 million or so deal with it at home, and 50,000 people die from it.
That puts pneumonia (together with other flu-related deaths) as the eighth most common cause of death in the U.S., with an annual cost of care of about $8.4 billion.
Stateside, it mostly affects older adults (though kids and younger adults can get it). But in developing countries, where kids aren't protected by as many vaccines, a million children under the age of 5 die from it every year.
Identifying a case's cause has gotten easier and faster. In just the past few years, says Michael Bachman, M.D., Ph.D., the time it takes a properly equipped testing lab to identify which virus or bacterium is making someone sick has gone from more than a day to just hours.
The rapid pace of identification, via modern genetic tests performed by specially trained staff like those Bachman oversees at the University of Michigan Health System's clinical microbiology lab, means doctors can get more precise information to help pick the right treatment for each patient.
Currently, this testing is mainly for hospitalized patients, but in the future it may guide the care of less severe cases.
You can protect yourself and your loved ones. Vaccines can prevent many of the infections that can lead to pneumonia. They're not a guarantee, says U-M infectious disease specialist Laraine Washer, M.D., but they're the best defense we have.
Other ways to prevent pneumonia include:
-
Wash your hands and cover your cough.
-
After 6 months of age, get your flu shot every year. It reduces your risk of the flu, which can lead to pneumonia.
-
If you're over 65, get your pneumonia shots. One called PCV13 (Prevnar) protects against 13 bacteria, and ideally you should get it first. Then, a year later, get the PPSV23 (Pneumovax) vaccine that protects against another 23 bacteria.
-
If you have a baby or toddler, make sure he or she gets all vaccines on schedule. This can protect against infections that can lead to pneumonia and other problems.
-
If you or your child have other health issues, talk to your doctor about the right vaccines for you. This includes people of any age who have conditions such as asthma, diabetes, heart disease or lung disease, or who are getting immune-compromising treatments, such as chemotherapy.
-
If you smoke, quit. Smoking greatly increases your chance of developing pneumonia. If you're not ready to quit, talk to your doctor about vaccination.
If you think you've got it, take action. Symptoms including fever, chills and cough may mean many things. It will take some detective work to figure out if it's pneumonia, what's causing it and the best treatment for you.
To help doctors and nurses help you:
-
Take your temperature and note the color of your phlegm.
-
Go to the doctor for an examination and perhaps a chest X-ray to look for signs of infection.
-
If you're seeing a new provider, make sure they know about all your health conditions and vaccinations.
-
If you're told to rest, rest.
-
If your doctor doesn't think you need antibiotics, listen because antibiotics don't work against viruses.
-
If you're given antibiotics, take them as directed. If you stop too soon, you could leave the strongest bugs alive, which means they could come back or sicken others.
-
If you're sent home to recover, follow instructions about when to call in if your symptoms don't ease. Pneumonia can last for weeks.
-
If you're sent to the hospital, and sometimes even your doctor's office, you'll need to cough up a good sample of phlegm from your lungs for the lab to test. Bachman notes that his lab team has to try to grow the bacteria in order to identify them. If the sample is contaminated with microbes from the patient's mouth or throat, it's useless.
The "walking" type isn't as bad as others. You may have heard the phrase "walking pneumonia." It's the nickname for a milder form of pneumonia that most often affects young adults and kids, often in the late summer and fall.
Caused by a kind of bacteria called Mycoplasma, this form doesn't lay someone flat like "regular" pneumonia. But it's still a good idea to see a doctor, rest up and take antibiotics only if you really need them.
Research and new technology will make the future even better for pneumonia prevention and care. The vaccines we can get today came from research — and research showed that after one of the newer vaccinations came on the market, the number of infections from resistant forms of the most common bacterial cause of pneumonia decreased, says Washer.
Meanwhile, research on the basic biology of microbes — like what Bachman and his research colleagues do — can help the search for new antibiotics and new tests for specific bacteria and viruses.
"There's increasing awareness that rapid diagnostic tests are important to control antibiotic resistance," says Bachman. "If we can quickly figure out what the cause of a pneumonia case is, whether bacteria or virus, we can appropriately treat it with very targeted drugs, as opposed to broad-based ones that could lead to resistance."

Explore a variety of healthcare news & stories by visiting the Health Lab home page for more articles.

Department of Communication at Michigan Medicine
Want top health & research news weekly? Sign up for Health Lab’s newsletters today!