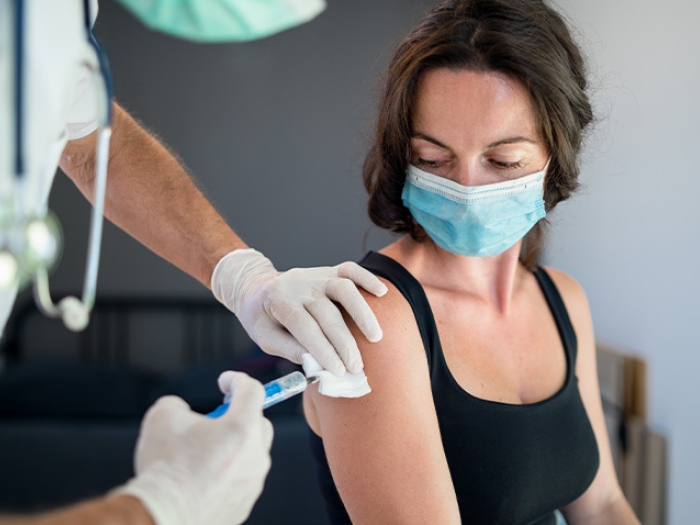
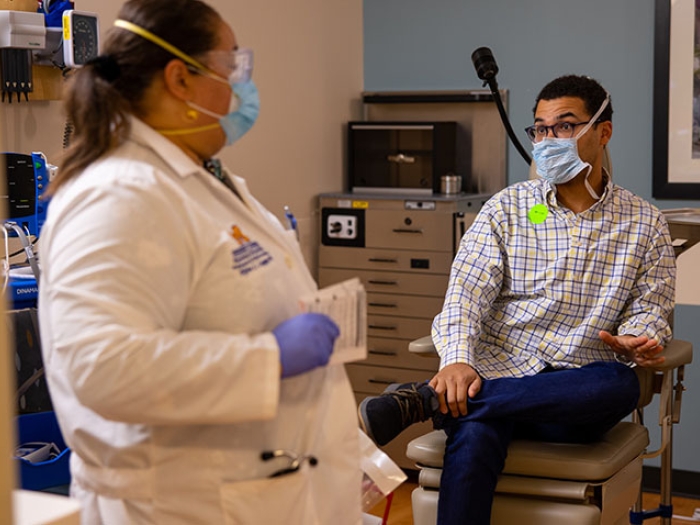
What we know about treatments, vaccines, boosters and more.
10:41 AM
Author |
It seems just about every day there is a new development in the COVID-19 pandemic and new questions about everything from infection to vaccines and boosters, long-haul symptoms and effective treatments.
To ease fears and share more information about what's known and happening with the coronavirus to date, Michigan Medicine infectious disease specialists came together during a live webinar to discuss some of your lingering and current concerns.
What are monoclonal antibodies?
Lindsay Petty, M.D.: Monoclonal antibodies really are meant to augment the immune system to the virus and infection. The ones that have been designed, and there are three currently available, bind to different parts of the spike protein which is the part of the virus that attaches to the ACE2 receptor and gets taken into your cells and can then replicate and cause more damage. The idea is to blunt and block that binding and uptake into cells.
The evidence for them was preliminary back in November 2020, when the first emergency use authorization came out, but there was a signal at that point that they seemed safe and helped prevent progression to severe disease in patients who are at high risk for severe disease. We really were early adopters of this treatment at Michigan Medicine, but I can say now in both our real-world experience of almost 2,000 patients treated, but also many additional publications, have shown consistent benefit, in particular for patients that are high risk for progression to severe disease.
What do you do when someone in your home tests positive for COVID?
Laraine Washer, M.D.: Testing may be done in response to symptoms, and in which case if someone has a positive test, whether it be a home test or a commercial test from a pharmacy or the doctor, those people should first and foremost isolate themselves to prevent spread to others. That includes wearing a mask themselves and having others in the household wear a mask.
MORE FROM MICHIGAN: Sign up for our weekly newsletter
Then, if they are symptomatic and the home test is positive then it very likely is a true positive and they should behave as such by isolating and it's a good idea to talk to your medical provider because you may be a candidate for a monoclonal antibody treatment and you may have questions about what else to watch out for.
If you have mild symptoms—headache, cough, sore throat, fever and no respiratory symptoms, like low oxygen levels—you may be able to tough it out at home.
I do recommend that almost every patient who has told me about a COVID diagnosis get a hold of a pulse oximeter and monitor their oxygen concentrations, and if those fall low below 92%, that's a signal you need medical care and might need to be admitted and might need other therapies.
If you're doing a home test because you've been exposed to someone and it's positive, you should also act as if you are positive and isolate. If you are asymptomatic and haven't been exposed, those are the cases where it might be a false positive, but you should also act as if you are positive and get a confirmatory PCR test.
Should we be worried about other COVID-19 variants and are they going to be worse than the Delta variant?
Adam Lauring, M.D.: I think it's important to follow variants and I personally feel it's important because that's what I do.
I don't think anyone really knows if there's going to be something worse than Delta down the road. I often tell people it's only so bad that the virus can get—there are limits. Even though we've experienced waves of variant after variant, that doesn't necessarily mean it will always be this way. There are other variants in the past few months that have hit the news but haven't proven to be as concerning as Delta.
So, pay attention? Yes. Worry? Not so much.
The thing that worries me more is we've had the tools to control even something as bad as Delta, but as a society we haven't really been able to effectively use or implement them. I think that is going to be an ongoing challenge going forward.
What is the current data on antibody immunity and the rate of decline of effectiveness of the COVID-19 vaccines towards preventing infection?
Lauring: It's clear that antibodies in your blood will decline over time. I can't give data on specific rates because it will depend on who you're studying—certainly it varies with age. Circulating antibodies are a good correlate of protection but they're only a small slice of how a vaccine works.
Just as important, but a little harder to study are the long-lived cells that make the antibodies and ramp up soon after you get infected. There are also T cells that the vaccine train to help you clear an infection, so maybe you'll still get infected, but you won't get as sick. These other factors are important to prevent people from getting sick even if the antibodies don't completely protect from infection.
Watch the full interview for more information on long-haul COVID, the latest data on boosters for the Moderna, Pfizer, J&J vaccines as well as mixing and matching vaccines, concerns about myocarditis after vaccination, and more.
Like Podcasts? Add the Michigan Medicine News Break on iTunes, Google Podcasts or anywhere you listen to podcasts.

Explore a variety of healthcare news & stories by visiting the Health Lab home page for more articles.

Department of Communication at Michigan Medicine
Want top health & research news weekly? Sign up for Health Lab’s newsletters today!